In this blog for parents of preterm babies, paediatrician and Cochrane UK Fellow Rufaro Ndokera looks at Cochrane evidenceCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. on ways to help preterm babies feed orally.
Page last updated: 21 June 2023 to reflect updated evidence on oral stimulation.
You may have had this experience. Something unexpected – or perhaps expected – has occurred in your pregnancy that means you will see your baby much sooner than planned. Someone from the neonatal team comes to speak to you, and explains what to expect in the coming days, weeks and months, although can you ever be fully prepared? At the end of that chat, there is often the question – how are you planning to feed?
At that point, feeding may be the furthest thing from your mind but over the coming months, it will pose a significant challenge to you and your baby. Regarding what to feed, we all know the old phrase ‘breast is best’, but in the preterm group, access to breast milk is so much more critical.
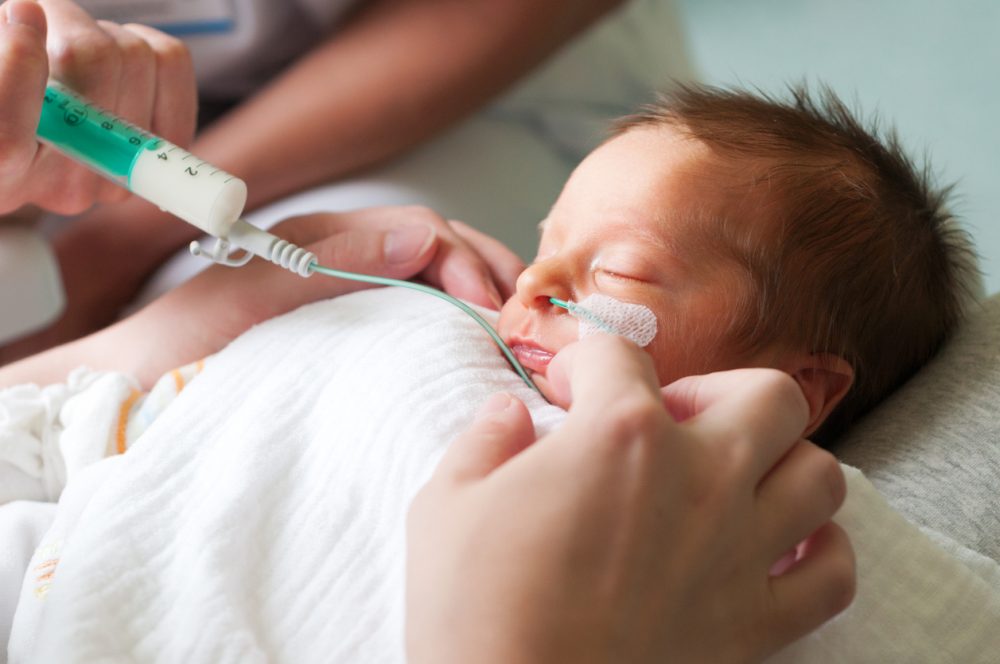
Regardless of whether it’s breast milk or preterm formula, in the run-up to home time you may have been happily tube feeding your baby for the last weeks. For those who may not know, the tube I refer to is a nasogastric tube, from nose to tummy, allowing staff and parents to feed babies who are not yet ready to take sucking feeds. Then the time comes to put baby to the breast or offer a bottle. It may all come naturally to you and your little one but more likely it takes some time. Have you ever wondered if there was evidence about what else we could be doing in the run up to that day to make feeding more successful?
There has been a group of Cochrane systematic reviewsIn systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research., putting all available evidence from randomisedRandomization is the process of randomly dividing into groups the people taking part in a trial. One group (the intervention group) will be given the intervention being tested (for example a drug, surgery, or exercise) and compared with a group which does not receive the intervention (the control group). controlled trialsA trial in which a group (the ‘intervention group’) is given a intervention being tested (for example a drug, surgery, or exercise) is compared with a group which does not receive the intervention (the ‘control group’). together, looking at ways we can hasten oral feeding in preterm babies. So, let’s have a look.
To suck or not to suck? That is the question
So, the question that I’m sure has been in your mind during your time with your new bundle is ‘when is the time to start trying?’. All the reflexes required for a baby to be able to feed orally, that is, to suck, swallow and breathe in a coordinated fashion, develop around 34 weeks, give or take. But apart from that, do we have any other ways of telling if your baby is ready to give it a go?
The first review Instruments for assessing readiness to commence suck feeds in preterm infants: effects on time to establish full oral feeding and duration of hospitalisation (published August 2016) looked into this. The question being asked was: is there a scale, protocolThe plan or set of steps to be followed in a study. A protocol for a systematic review should describe the rationale for the review, the objectives, and the methods that will be used to locate, select, and critically appraise studies, and to collect and analyse data from the included studies. The protocols for Cochrane Reviews are available in the Cochrane Library. or instrument that made it quicker to decide if a baby was ready to start with the breast or bottle? Sadly, the team were unable to identify any studies (randomised controlled trialsClinical trials are research studies involving people who use healthcare services. They often compare a new or different treatment with the best treatment currently available. This is to test whether the new or different treatment is safe, effective and any better than what is currently used. No matter how promising a new treatment may appear during tests in a laboratory, it must go through clinical trials before its benefits and risks can really be known.) that addressed this question. The lack of available evidence in this area may be frustrating, but whilst we wait, taking cues from speech and language therapists, nurses and – of course – your baby will suffice for now.
Practice makes perfect?
The next review Oral stimulation for promoting oral feeding in preterm infants (published June 2023) looks at whether activities for stimulation of the mouth get oral feeding going faster, and therefore get babies off home sooner. After all, if you have never had to make these movements or coordinate these muscles together before, why should you know how? A strange thought I know, since we all do it at least 3 times a day, every day, but it’s clearly a skill to be learnt.
By oral stimulation, the authors mean activities such as sucking on a gloved finger and stroking of the cheeks and around the mouth before feeding. This stimulates the nerves and muscles around the mouth and stops them from becoming hypersensitive. Although this would require teaching, it could easily be taught to you as parents, allowing you to get even more involved in the care.
However, the review found that – when compared with standard care or interventions not involving the mouth – the evidence is very uncertain about whether oral stimulation:
- can speed up the time it takes for babies to be exclusively breast or bottle fed
- can reduce the length of intensive care stay or hospital stay
- can reduce the need for babies to be given nutrition through the vein
There was no information gathered about parent satisfaction.
With such low-certainty evidence, we need to do more research and we need to do it as best we can. In the meantime, preterm babies benefit in so many ways from positive touch so maybe run it past your team.
A bottle a day keeps the breast at bay?
The next review Avoidance of bottles during the establishment of breast feeds in preterm infants (published October 2021) looks at whether avoiding bottles when you are away (i.e. breast feeding mummy), increases rates of breastfeeding on discharge and for the following months.
The review suggests that babies who are cup fed instead of bottle fed when mum is away may be more likely to be partially or completely breastfed at discharge, and also at 3 and 6 months. However, again, we have to look at the quality of the evidenceThe certainty (or quality) of evidence is the extent to which we can be confident that what the research tells us about a particular treatment effect is likely to be accurate. Concerns about factors such as bias can reduce the certainty of the evidence. Evidence may be of high certainty; moderate certainty; low certainty or very-low certainty. Cochrane has adopted the GRADE approach (Grading of Recommendations Assessment, Development and Evaluation) for assessing certainty (or quality) of evidence. Find out more here: https://training.cochrane.org/grade-approach and again, it seems that most of the evidence is of low certainty, so we need to be mindful of how much weight we put on this. An interesting point raised by this review is that only one of the 5 studies commented on dropout rates, and in this case they were high. Does this suggest that although cup feeding may be better as a way of oral feeding without a bottle, it may be too inefficient for long-term use?
These findings fit with the findings of another Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. Cup feeding versus other forms of supplemental enteral feeding for newborn infants unable to fully breastfeed (published August 2016). The majority of infants included in this second review were preterm, although not all. Here, the majority of babies received both cup feeds and another supplemental feed i.e. nasogastric tube or bottle, during the investigation period. This is reported to be due to poor staff and parent satisfaction. Again, the studies were of poor quality.
So what do we do? Based on these 2 reviews, I would say that the jury is still out. The question has been raised but based on the information at hand here, it hasn’t been conclusively answered. So the question becomes what do you want to do and how can the team around you support you to do it?
Feeding 9 to 5 – what a way to fill your tummy!
Right, still with me? Now, if you have a preterm baby, you will know all about the regular updates on feed frequency. Today, 2 hourly, then tomorrow 3 hourly. A little blip with breathing, back to 1 hourly for a while. Well, before getting off the nasogastric tube and getting home, we usually aim for babies to be feeding 4 hourly and to complete either a whole bottle feed or have a good breastfeed.
Well, the next review is looking to see if that is the right way of going about things. After all, most term babies would usually go home and be fed as and when they want.
The review Responsive versus scheduled feeding for preterm infants (published August 2016) looks into this issue: does feeding based on whether and when your baby is hungry help with growth, intake? Does it improve parent satisfaction and get you home faster?
The review looked at babies who were about to go home and were in the transition phase between tube and full oral feeding.
The findings suggest that babies who were fed on a schedule were more likely to gain weight faster but that babies fed in response to cues were faster to be free of their nasogastric tubes and got home at an earlier corrected age.
Again, it is so important to consider the quality of the papers. Overall, the evidence was of low quality, we can’t put too much weight on the conclusions.
Doing what’s right for you and your baby
I hope this has helped you understand some of the suggestions you may be being given within the hospital a bit more. Although all the reviews have concluded that our confidence in the results is limited, I think what we can say is that there is no clear evidence that one thing is significantly worse or better than the other. It may be that the evidence will exist one day, just not today. So with all that in mind and with your head surely spinning from all of that information, I say do what feels right for you and your baby, engage your nurses in the conversation, raise and discuss the knowledge you have which may be different to theirs, and work together to get you and your baby home as soon as possible as big and happy as we can.
Rufaro Ndokera has no conflict of interest to disclose.