In this blog for people with endometriosis, Dr James Duffy, Clinical Fellow at King’s Fertility, discusses the latest Cochrane evidenceCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. on blood tests for diagnosing endometriosis. He reflects on the need to develop accurate blood tests, the current research evidence, and the potential of a blood test called CA125 for diagnosing endometriosis. This blog is the second in our #MyEndometriosisQuestion series running throughout March, with blogs about endometriosis and an invitation to ask your questions, which will be addressed by a panel of experts. More details at the end of this blog.
Featured image: ‘One in Ten – My friends don’t understand’ by Margaret Kalms* http://www.endowomanart.com
Page last updated 24 March 2022 and last checked 30 June 2023

What is endometriosis?

How is endometriosis currently diagnosed?
Diagnosing endometriosis is a critical step in ensuring people receive appropriate treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes.. The first step is to arrange a telephone or in person consultation with your GP if you are experiencing symptoms which you think could be caused by endometriosis. In my experience, people describe many different endometriosis symptoms including:
- Painful periods
- Lower abdominal pain between periods
- Painful bowel motions
- Discomfort when passing urine
- Fatigue
One of the reasons why many people experience a delay in diagnosis is that they are reluctant to arrange a consultation with their GP. I often explain to people to review the GP practice’s website to see if any of the doctors have a special interest in this area, for example, have completed additional qualifications including the Diploma in Obstetrics and Gynaecology (DRCOG) or Diploma in Sexual and Reproductive Health (DFSRH). Doctors with these additional qualifications have spent a considerable amount of time developing knowledge, skills, and expertise in this area and are often more experienced in endometriosis diagnosis and treatments.
The GP should offer you an internal examination and ultrasound scan and offer referral to a gynaecologist with a special interest in endometriosis. In England, you have the right to be referred to any hospital using the NHS e-Referral Service, further information can be found here: www.nhs.uk/nhs-services/hospitals/book-an-appointment/. Choosing a particular hospital is based on your circumstances and preferences and factors you may wish to consider, including their expertise in the diagnosis of endometriosis.
Ultrasound scan: the first test for diagnosing endometriosis
The National Institute for Health and Care Excellence produce evidence-based guidance and advice for health professionals. The current NICE guidelines for endometriosis recommend people with symptoms suggestive of endometriosis should be examined by an experienced healthcare professional and offered a transvaginal ultrasound scan.
A transvaginal ultrasound scan is a safe and straightforward procedure that uses ultrasound waves to produce images of the womb (uterus), fallopian tubes, and ovaries. During the ultrasound scan, you will be asked to either lie on your back, or on your side with your knees drawn up towards your chest. A small ultrasound probe with a sterile cover, not much wider than a finger, is then gently passed into the vagina. Many people describe the transvaginal ultrasound scan as uncomfortable, not painful. It is important to know that a normal ultrasound scan does not rule out endometriosis. I will be discussing the accuracy of ultrasound in diagnosing endometriosis in a future blog later this week.
Some people decline a transvaginal ultrasound as they feel uncomfortable. It is important to appreciate this is completely OK and there are alternative options including a MRI scan or keyhole surgery.
There is a vibrant online community of healthcare professionals who share knowledge of diagnosing endometriosis using ultrasound you may want to look at their twitter pages: Dr Susanne Johnson (@GynaecologyUS), Mathew Leonardi (@MathewLeonardi), and Joel Naftalin (@JoelNaftalin).
MRI scan
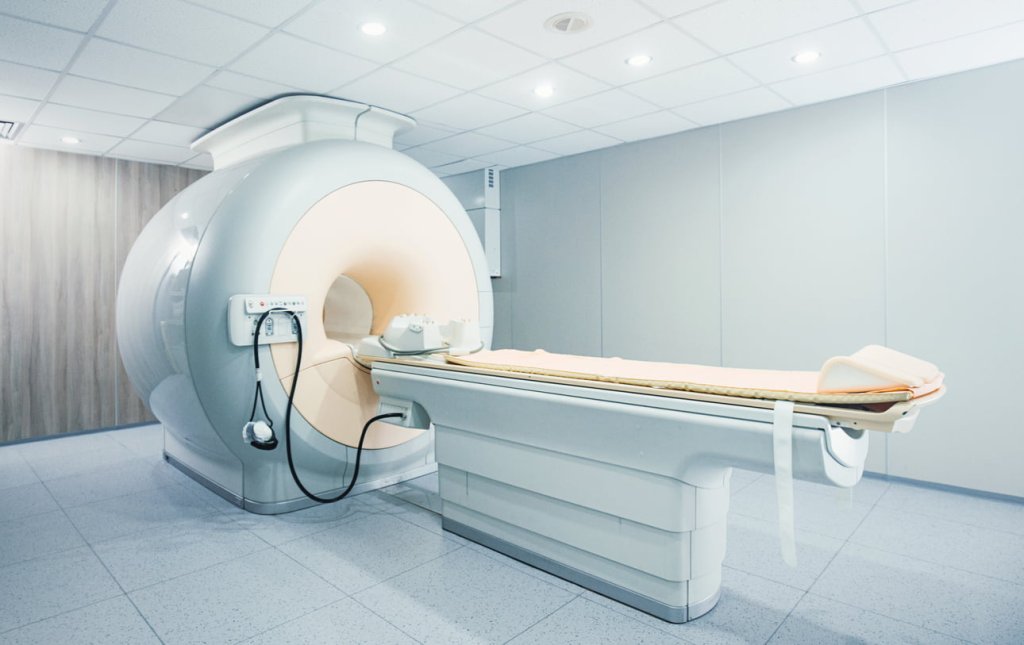
If there is any suggestion of endometriosis involving the bowel, bladder, or ureters, the NICE guideline recommends people should be offered an MRI scan. It is a type of scan that uses strong magnetic fields to produce detailed images of the inside of the body. The MRI scan is quite loud and you will be offered headphones. Some people find the MRI scan quite claustrophobic as you enter a large circular tube. If claustrophobia could be a problem for you please let your doctor know as there are different ways they can help make the experience more comfortable. The MRI provides detailed pictures which can help assess the location and severity of endometriosis.
Keyhole surgery for diagnosing endometriosis
Currently, the only reliable way of diagnosing endometriosis is to perform keyhole surgery and see the endometriosis inside the abdomen directly. Endometriosis has many different appearances and it can be challenging for a gynaecologist to tell the difference between endometriosis and other conditions. Taking a tissue sample of the suspected endometriosis and examining the tissue using a microscope is the very best way to confirm the diagnosis of endometriosis. Although keyhole surgery is the best way to diagnose endometriosis, it is invasive, associated with risks and complications, and expensive.
Some people decline a keyhole surgery as they would prefer to avoid surgery. It is important to appreciate this is completely OK and treatment can begin with a suspected diagnosis based your symptoms and other investigations, including ultrasound scan and MRI.
Delays in diagnosing endometriosis
Many of the people I see in my clinic have waited a long time to be referred to a gynaecologist and have felt they had not been listened to during many parts of their journey. This needs to change. There have been many reports, including a recent report from the All-Party Parliamentary Group on Endometriosis, that people with endometriosis experience substantial delays in securing a definitive diagnosis. A contributory factor is the need to be referred to a gynaecologist and for them to perform key-hole surgery to definitively diagnose endometriosis.
Developing an accurate blood test, which could hopefully be requested by GPs, could help tackle these delays.
Is there an accurate blood test to diagnose endometriosis?
In the Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. Blood biomarkers for the non‐invasive diagnosis of endometriosis (May 2016) Vicki Nisenblat and colleagues brought together the evidence from all published research studies evaluating blood tests to diagnose endometriosis. They included research studies which evaluated blood tests as a replacement tests for keyhole surgery. They identified 141 research studies which evaluated 122 different blood tests.
Only four blood tests (anti‐endometrial Abs, IL‐6, CA‐19.9, and CA‐125) were evaluated by enough research studies to provide a meaningful assessment of their accuracy. No blood test was judged to be accurate enough to replace keyhole surgery (for diagnosis). Within their conclusions they emphasised the need for further high quality research to evaluate the accuracy of a wider range of blood tests.
CA125: A potential blood test to rule in endometriosis
I was part of the research team which prepared another diagnostic review, Diagnostic Accuracy of CA 125 for Endometriosis, published in May 2016, in BJOG: An International Journal of Obstetrics and Gynaecology.
We identified, evaluated, and combined research studies evaluating the accuracy of CA 125. We took a different approach when compared with the above Cochrane diagnostic review by only including studies which compared the blood test CA 125 with keyhole surgery for diagnosis and tissue sample (histologically) confirmed endometriosis. We included 22 research studies which included the results of 3626 women with suspected endometriosis.
We discovered women with pain symptoms suggestive of endometriosis and who had a positive CA 125 test (>30 units/ml) were almost always found to have endometriosis. Therefore, this blood test can be used as an accurate diagnostic test, facilitating a quick diagnosis, and could provide women with endometriosis earlier access to specialist treatment. Unfortunately, a negative CA 125 test (<30 units/ml) does not exclude the possibility of endometriosis and these women will require further investigation.
Looking ahead
Reflecting upon my research, I think it would be reasonable to offer an examination, transvaginal ultrasound scan, and the blood test CA125 in a GP setting to help rule in endometriosis at an earlier stage. This remains my own opinion and I am hoping NICE and other organisations which prepare endometriosis guidelines will consider changing their recommendations.
Questions to ask your gynaecologist
- What is the most likely cause of my symptoms?
- What could be the other causes of my symptoms?
- Please explain how you have ruled in and ruled out these causes.
- If you identified endometriosis during keyhole surgery would it be treated?
- What are the risks of keyhole surgery?
- What are the alternatives to keyhole surgery?
Support for people with endometriosis
There is a vibrant online community of people with endometriosis, commonly known as #endosisters, who share knowledge and offer support, along with charities such as Endometriosis UK and grassroots organisations such as Fair Treatment for the Women of Wales.**
Further information about endometriosis
- Cochrane Gynaecology and Fertility: Endometriosis Awareness Month
- Endometriosis UK
- The British Society for Gynaecological Endoscopy (BGSE) maintains a list of accredited endometriosis centres.
- As of March 2022, specialist endometriosis nurses have been appointed in each Health Board in Wales to improve services for those with the condition.
More about #MyEndometriosisQuestion – and ask yours
You can find out more in the blog Endometriosis: #MyEndometriosisQuestion – a special series, including how to ask your question on our social media platforms, or you can post your question below this blog. While our experts cannot give specific medical advice, they can provide information about endometriosis, relevant evidence and guidelines, and tips for discussing endometriosis with your own health professional. Our expert panel will do their best to answer your questions individually. They will also reflect on some of the submitted questions in a blog to be published at the end of the month. No individuals will be named or identified in this blog.
**Editors’ note: From March 2022, specialist endometriosis nurses have been appointed to each Health Board in Wales, to improve health services for women with endometriosis.
Join in the conversation on Twitter with @JamesMNDuffy @CochraneUK and @CochraneCGF or leave a comment on the blog. Comments are checked by the Editors before they are made public on the blog.
Please note, we cannot give specific medical advice and do not publish comments that link to individual pages requesting donations or to commercial sites, or appear to endorse commercial products. We welcome diverse views and encourage discussion but we ask that comments are respectful and reserve the right to not publish any we consider offensive. Cochrane UK does not fact check – or endorse – readers’ comments, including any treatments mentioned.
James Duffy has nothing to disclose.
References and further reading (pdf)
*Featured image used with permission and cannot be reused without permission from the artist.



[…] is currently no routine screening for endometriosis. Research suggests that the tumour marker CA125 (often included in health screening packages in Singapore for […]
Helpful post for my problem
I had a hysterectomy 14 years ago leaving one over. Similar pains throughout the years but now about 8 was of pain Resembling that of endometriosis. Can o have that again even though I had a hysterectomy?
Yes, you can. Endometriosis is endometrial tissue that grows outside of the uterus so removing the uterus does not take care of the problem and the tissue can continue to grow in other areas of the body.
My wife had a CA 125 test 18 days after her endometriosis surgery, it read 205, I just want to know how long the CA125 level usually remains after this surgery, before the surgery the ca125 was 161.