In this guest blog, Dr Martin Hirsch and Dr Stuart Spencer explain about endometriosis and treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes. choices for women who have the menopause induced because of it.
Blog last updated: 28 February 2023.
For Menopause Week, we have been summarising the evidence surrounding the menopause to ensure women get the correct facts from reliable evidence. This blog aims to help women who have had the menopause induced through surgery for endometriosis make more informed health decisions at a time of significant change for their mind and body.
Endometriosis – what is it and how do I know if I have it?
Most women have heard of the menopause. They fear it, but for a select few women the menopause is a relief and a respite from the years of agony and pain from endometriosis that few people seem to understand.
Endometriosis is the reason that thousands of women each year have the menopause induced temporarily with medicines or permanently with surgical removal of the womb and ovaries. The disease is characterised by the presence of cells (normally found inside the womb) in areas outside the womb such as the ovaries and surfaces of the pelvis, bowel, and bladder. It affects up to ten percent of females during their reproductive years causing higher levels of pain in and outside of their menstrual cycles together with painful intercourse and difficulties falling pregnant. If there was a condition that made 10% of mens’ testicles hurt, with pain during intercourse, there would be a river flowing out of my GP surgery doors from the volume of male tears being shed in the waiting room.
It’s widely acknowledged that pain is highly subjective with a difficult basis for comparison and considering that most women suffer from a degree of pain during their periods, endometriosis sufferers assume theirs is the same as everyone else. It’s not.
To compound matters, getting diagnosed with endometriosis is difficult. There is currently no accurate non-invasive test that your GP can request. The formal diagnosis of the condition is reserved to keyhole surgery and laboratory analysis of biopsies as ultrasound scans have limited accuracy. The pathway to get referred to a hospital specialist and then get referred for keyhole surgery results in an average waiting time of 10 years between first symptoms and diagnosis.
Endometriosis – what can be done about it?
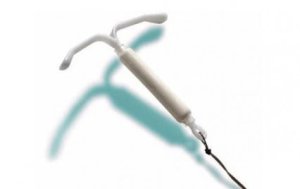
The disease is believed to be dependent on oestrogen which is a hormone produced from a woman’s ovaries. Common treatments aim to prevent cyclical fluctuation in these hormones by inhibiting ovulation and the most readily used treatment is the combined contraceptive pill. The progesterone releasing coil, Mirena, has been thought to have beneficial effects on endometriosis-related pain, and like other coils prevents conception. However, an update to this Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. Levonorgestrel‐releasing intrauterine device (LNG‐IUD) for symptomatic endometriosis following surgery (updated December 2021) found a lack of high-quality evidence to support this. The authors conclude that there is insufficient evidence that inserting a Mirena coil after surgery for endometriosis reduces pain. It suggested a need for further high-quality studies to better inform this practice.
Surgically treating these cells via keyhole surgery with techniques to burn or cut out the lesions of endometriosis has a beneficial effect on pain and fertility. However, the recurrence rateThe speed or frequency of occurrence of an event, usually expressed with respect to time. For instance, a mortality rate might be the number of deaths per year, per 100,000 people. of pain following surgery is up to 30% within the first 12 months. For some women these treatments are ineffective and stronger more invasive methods are required to stop the pain. Surgically removing the ovaries and inducing a permanent menopause or medically inducing a temporary menopause is often the final option for many women. These induce a dramatic fall in a woman’s oestrogen levels and improve pain.
Inducing the Menopause – what are the risks?
The risks of artificially and prematurely inducing the menopause include osteoporosis, along with the side effects of the menopause resulting from low oestrogen levels that include hot flushes, night sweats, skin dryness and insomnia.
Osteoporosis is the thinning of the bone density that increases a woman’s riskA way of expressing the chance of an event taking place, expressed as the number of events divided by the total number of observations or people. It can be stated as ‘the chance of falling were one in four’ (1/4 = 25%). This measure is good no matter the incidence of events i.e. common or infrequent. of fractures. Our bone strength and density is reliant on calcium that is constantly in balance between blood calcium forming bone and calcium released from bone to maintain blood levels. Oestrogen reduces the amount of calcium released from the bone, and this prevents thinning and reduces the risk of osteoporosis and fractures.
Menopausal side effects can be debilitating and are associated with hot flushes and reduced emotional wellbeing. These symptoms are often more severe with abrupt surgical removal of the ovaries compared to the natural menopause, with these symptoms lasting up to ten years. For this group of women who go through the menopause naturally, Hormone Therapy (HT), formerly hormone replacement therapy, may be an option if the menopause occurs early or if symptoms are very severe. This combination of oestrogen and progesterone protect women from osteoporosis and the symptoms of low oestrogen.
The risks associated with HT are blood and cancer related. A recently published Cochrane systematic review found very interesting and divided answers depending on the age of the groups analysed. When examining the results of all women that take HT there is evidence of increased risk of suffering blood clots in the legs or the lungs or having a stroke. But for women taking it close to their menopause or younger than 60 the risks and benefits look different.
The headline news over the past few years surrounds a very small associated increase in breast cancer and ovarian cancer with HT. This must be put in to context: several very large reviews have found that of those women using HT for over 5 years and around the age of 50, there is one extra case of breast and ovarian cancer compared to those women who do not use HT. This does not imply that HT causes breast or ovarian cancer but there is a very small increased risk that women need to be aware of.
HT after surgical removal of the ovaries in endometriosis – what research is out there?
The use of HT for women after the surgical menopause for endometriosis has been debated and theorists are wary that providing hormones that mimic the natural hormones released by the ovary will result in further endometriosis symptoms and disease recurrence.
A Cochrane Review Hormone therapy for endometriosis and surgical menopause brought together the evidence from all published studies looking at women who have had their ovaries removed for endometriosis and then taken HT to prevent the risks of osteoporosis and menopausal symptoms. The authors searched only for those studies that randomly allocated patients to groups of different types of treatments or no treatment. These studies are called randomisedRandomization is the process of randomly dividing into groups the people taking part in a trial. One group (the intervention group) will be given the intervention being tested (for example a drug, surgery, or exercise) and compared with a group which does not receive the intervention (the control group). controlled trialsA trial in which a group (the ‘intervention group’) is given a intervention being tested (for example a drug, surgery, or exercise) is compared with a group which does not receive the intervention (the ‘control group’). (RCTs) and reduce biasAny factor, recognised or not, that distorts the findings of a study. For example, reporting bias is a type of bias that occurs when researchers, or others (e.g. drug companies) choose not report or publish the results of a study, or do not provide full information about a study. affecting the results of the studyAn investigation of a healthcare problem. There are different types of studies used to answer research questions, for example randomised controlled trials or observational studies.. One study examined the recurrence of pain and need for repeat surgery between patients randomly allocated to either HT (115 women) or placeboAn intervention that appears to be the same as that which is being assessed but does not have the active component. For example, a placebo could be a tablet made of sugar, compared with a tablet containing a medicine. / no treatment (57 women). The second, smaller study, examined only pain recurrence between two randomly allocated groups, those who used traditional HT (11 women) with those who took a synthetic HT called Tibolone (10 women). Regrettably, both of these studies examined separate treatment interventions making direct comparison very difficult.
Key message
- Neither of the two studies found significant differences in the pain nor need for further operations experienced by women following HT when compared to no treatment or different types of HT.
Where does this leave us?
For this small group of women who have exhausted their options with conventional treatment, spent years in pain and finally found relief in permanent removal of the ovaries, a difficult decision lays ahead. Whether to take HT to prevent osteoporosis and side-effects from low oestrogen is marred by the lingering possibility of their nemesis returning to haunt them. Studies have not yet answered the question completely. The evidence from the two studies is not strong enough to deny HT to women who have had the surgical menopause, but the authors recognise from the trends in statistics that these women may be at increased risk of their pain returning and the need for further operations. Further studies are recommended.
Resources on menopause
The Editors have added these in April 2022. With thanks to @drhannahshort, GP Specialist in Menopause & Premenstrual Disorders, for her suggestions.
- You can find our other blogs on menopause here.
- Balance: Founded by Dr Louise Newson, “a GP and Menopause Specialist who works to increase awareness and knowledge of the perimenopause and menopause, and campaigns for better menopause care for all women”.
- British Menopause Society: tools for clinicians and Menopause Care Resources Toolkit
- Daisy Network, a charity providing information and support to women with Premature Ovarian Insufficiency, also known as Premature Menopause.
- European Society of Human Reproduction and Embryology – Guideline on the management of premature ovarian insufficiency.
- Global Menopause Inclusion Collective
- Healthtalk – Menopause. Here you can see videos of women in the UK talking about their menopause experiences.
- International AssociationA relationship between two characteristics, such that as one changes, the other changes in a predictable way. For example, statistics demonstrate that there is an association between smoking and lung cancer. In a positive association, one quantity increases as the other one increases (as with smoking and lung cancer). In a negative association, an increase in one quantity corresponds to a decrease in the other. Association does not necessarily mean that one thing causes the other. for Premenstrual Disorders: Surgery and surgical menopause for premenstrual disorders.
- Rock My Menopause (created on behalf of the Primary Care Women’s Health Forum)
- NICE guideline – Menopause: diagnosis and management.
- NHS – Menopause
- Women’s Health Concern factsheets
Links:
Gibbons T, Georgiou EX, Cheong YC, Wise MR. Levonorgestrel-releasing intrauterine device (LNG-IUD) for symptomatic endometriosis following surgery. Cochrane Database of Systematic ReviewsIn systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. 2021, Issue 12. Art. No.: CD005072. DOI:. DOI: 10.1002/14651858.CD005072.pub4.
Al Kadri H, Hassan S, Al-Fozan HM, Hajeer A. Hormone therapy for endometriosis and surgical menopause. Cochrane Database of Systematic Reviews 2009, Issue 1. Art. No.: CD005997. DOI: 10.1002/14651858.CD005997.pub2.
For Further information on Endometriosis or the Menopause please see these links:
Brown J, Farquhar C. Endometriosis: an overview of Cochrane Reviews. Cochrane Database of Systematic Reviews 2014, Issue 3. Art. No.: CD009590. DOI: 10.1002/14651858.CD009590.pub2.
Marjoribanks J, Farquhar C, Roberts H, Lethaby A, Lee J. Long‐term hormone therapy for perimenopausal and postmenopausal women. Cochrane Database of Systematic Reviews 2017, Issue 1. Art. No.: CD004143. DOI: 10.1002/14651858.CD004143.pub5.
Martin Hirsch’s biography appears below. Read Stuart Spencer’s biography.



My daughter suffered endometriosis for years. About 10 years ago she had her womb cauterised which stopped the bleeding. She is now menopausal (49 yrs). She is suffering severe hot flushes and losing sleep which she can I’ll afford being a farmer. Can she safely take hrt gel without causing everything to start over. Her doctor has not been able to give her an answer. She cannot have coil as for her it would mean hospital procedure as womb is tilted and twisted.
I just ran across this article. I am in the percentile that is not doing well with any estrodial. I am actually doing ok most days without it. Although I am scared to get osteo. Is there anything extra I can do to avoid it?
I had a hysterectomy and ovaries removed in November 2019 due to severe pain from endometriosis. Consultant confirmed that I still have endometriosis on my pelvis. Following the operation I struggled with severe hot flushes throughout the night and pain in my hip bones so I started HRT Tibilone 2.5 mg 6 weeks after surgery prescribed by my gp. I have since gone back for a review of my op with my consultant and she mentioned that Estrogen in hrt May cause the endometriosis to grow so to stop hrt once I have the hot flushes have eased.
Can you please suggest what hrt will be best for me. I am 47 and fit and well
Thanks
Sharon
I had a total hysterectomy at 35, this was 20years ago. I have never taken HRT and never had one symptom of the menopause is this unusual? Why is this?
Can I take hormones when I had endometriosis and I had done an abdominal hysterectomy and bilateral Salpingo-oophorectomy for endometriosis?.
This is something you’d need to ask your clinician.
Best wishes,
Sarah Chapman [Editor]
Hello, after having 9 surgeries from the age of 18 being the first, for cysts on my ovaries. The last being at the wonderful age of 42, when I begged for a hysterectomy. By the time that happened I had severe endometriosis. Surgery lasted 4.5 hours trying to separate my bowls and bladder from scar tissue. Well it didn’t work, they had to leave a lot of it behind.. including my cervix. Removed ovaries and uterus. I was immediately put on Premarin the highest dose possible for about 3 months… then cut off cold turkey… since then my life has been hell, lack of sleep, hot flashes and extremely moody… I am Bi-Polar as it is….I am at my wits end…I’m thinking about tryng to get on Delestrogen or Tibolone.. what do you think? I am now 49….
Hello, sorry to hear you’re struggling. These are questions you’ll need to take to your healthcare professionals.
Best wishes,
Sarah [Editor]
I had a total hysterectomy at 35 similar operation and found that Fluoxetine worked well to counter the menopause issues and made me feel normal again.
Hi I had endometrosis surgery in 2016 removed ovary uterus crevice . my age was 43 I did not take any hormonal tablets after that. Im perfectly alright. Is any hormonal tablets required for my future
Hello Meeta, this is something you would need to ask your doctor.
Best wishes,
Sarah
I have undergone laparoscopic hysterectomy with bilateral salphingooophorectomy.
My age 44 years surgery done before 2 months.
I have symptoms of stress mentally and physically. I have so much sleep disturbance.
So please give your opinion what medicine l should take tibolone. Or only estradiol therapy?
I’m afraid we can’t comment on treatment options for individuals. You might wish to look at whether there is any Cochrane evidence that could help you and your clinician in your decision making http://www.cochrane.org. Best wishes, Sarah
Hi, I had endometriosis and hysterectomy in 1984, I was 27 yrs old. Started on HRT soon after and now at 60 yrs old on pellet therapy. I have tried it all. Never had any pain or problems after hysterectomy. Diagnosed with thyroid harshimoto auto immune disease in my 30s.
Hi,
I’m now 21 and been struggling with endometriosis diagnosed since i was 13, I was put into a 6 months menopause and since haven’t been able to sleep, its now been 2/3 months since it wore off I still cant sleep correctly, I’m in a load of pain more than I was whilst in the menopause and as much as I try and push for a hysterectomy they wont because of my age I’ve had more laparoscopy’s than I can count so the menopause was the last straw for me as they didn’t want me to have anymore surgical procedures, I’m now at my wits end I was lucky to carry and have my daughter who is now 19 months old, and I am unsure of what to do I’ve tried every over the counter painkiller and nothing seems to work I’ve been rushed into hospital with the pain 3 times drugged up on morphine witch helps a bit and then sent home can you offer any advice
Hi Terri, I’m so sorry to hear this. Have you been in touch with Endometriosis UK? You’ll find them at https://www.endometriosis-uk.org It’s probably a good place to start. They can offer support and direct you to a specialist centre in your locality. I really hope you get some help.
With very best wishes, Sarah (Evidently Cochrane’s Editor).
Why no.mention that you absolutely need to have any remaining endo excised at the time of hyst and also use.of.progesterone as well as oestrogen thought to be more protective.
Hi Lesley Percy,
Thanks for your comment. You are correct that all endometriosis should be removed at the time of surgery but this can often be clinically very difficult with lesions imbedded into the bowel or bladder. Removing these areas can result in a patient needing that part of the bowel removed and remaining portion brought out to the abdominal skin (stoma). This then requires a repeat major surgery for reversal and increases morbidity (illness / suffering to the patient) both physically and psychologically. Endometriosis is thought to also occur from hormonal stimulation of cells which line the surfaces of the pelvic organs (Coelomic Metaplasia). This means that even if all visible endometriosis was removed at the time of surgery it could reoccur under the stimulation of the oestrogen hormones within HT.
It is difficult to say which HT is best for women following this surgery as there have been very few studies addressing this issue. However, the theoretical and scientific argument that adding progesterone is valid and held by many clinicians. From our clinical experience, Tibolone 2.5mg per day offers good clinical symptom control. Larger studies are needed to assess the impact of different types of HT on both reoccurrence of endometriosis and also development of osteoporosis.
I hope this has helped.
Thanks again,
Martin
It helps if have an.endo.gynae and.urology and.bowel specialist at the time of hyst.like i did. You need to.research your surgeons. All my.consultants highly recommend taking progesterone.