In this blog for people with moderate to severe psoriasis, Robert Walton, a GP and Senior Fellow in General Practice at Cochrane UK, assesses the latest Cochrane evidence on treatment with biologic drugs.
Take home points

These new biologic drugs are staging a quiet revolution in the treatment of psoriasis – a skin condition causing patches of skin that may be dry, itchy and sore. When psoriasis is mild, it can be no more than an inconvenience. However, moderate or severe psoriasis can have a major effect on quality of life, particularly when it also causes inflammation in joints and tendons which happens in up to a third of people with the condition. As psoriasis is relatively common, affecting 2-3% of people in the UK, effective new treatments are a big step forward. This blog is mainly relevant to skin problems – I’ll leave joints and tendons for another time.
The immune system and psoriasis: both problem and solution?
Although we don’t know the exact cause of psoriasis, overactivity of the immune system plays a large part, triggering the release of chemicals called cytokines which cause inflammation leading to discomfort and swelling. It’s a disease which probably hasn’t changed its form much over the ages, nor has the form of the word itself which is exactly the same as that used by the Greeks and Romans. The ‘psor’ part of the word reflects the itching that the condition causes.
As the immune system is the cause of the problem, it seems strangely appropriate that the same immune system might provide a solution. The biologics are drugs developed from antibodies which are proteins made by immune cells that recognise either the cytokines that cause the inflammation themselves or receptors on cells affected by the cytokines. When the antibody latches on to either of these targets it will block the action of the cytokine and prevent inflammation.
Current drug treatments for moderate to severe psoriasis such as ciclosporin or methotrexate also prevent inflammation but the way that they work is less specific than the biologics and they affect the functioning of many other cells in the body, so as a result come with a relatively high risk of side effects which tends to limit their use.
Which are the best biologics for psoriasis?
A recent Cochrane Review Systemic pharmacological treatments for chronic plaque psoriasis: a network meta‐analysis (published July 2023) gave a nice summary of data from 179 individual studies of biologics for psoriasis which included over sixty thousand people and helps to sort out which of the biologics are most effective.
One group of biologics came out ahead of the rest in terms of how well they controlled the area of skin affected by psoriasis and the severity of the disease in the affected areas (PASI score). The drugs most effective are infliximab, bimekizumab, ixekizumab and risankizumab. Infliximab is one of the first of the biologics developed and is widely used for a range of different diseases. People taking any of these drugs can hope for a marked reduction in symptoms from their psoriasis.
The review found little to no difference in effects between these different drugs and there was no evidence of a difference in serious adverse events between any of the drugs. There is still uncertainty about side effects in the long term though, as all the studies available for the review were relatively short and the quality of reporting for side effects was poor.
All the drugs need to be given by injection at about monthly intervals, but most people do these injections themselves without trouble.
Not all treatments work for everyone and there may be individual differences in the way that the different drugs are tolerated, so it’s good that there is a range of very effective treatments that work in different ways meaning that options are available for switching drugs when necessary. The review goes into some detail about other drug treatments and here’s a handy summary of all the different biologics and risk of side effects from the British Society of Dermatologists.
If these drugs are so good, why can’t everyone have them?
Unfortunately, a country can only spend a certain amount of money on health care so if we want to spend more on one treatment, we inevitably have to spend less on another. All the antibody drugs are very expensive costing several thousand pounds a year for each person. There is a difficult balancing act to be done so the treatments are only available to people with moderately severe or severe disease after they have tried more conventional medication and have either found it ineffective or been unable to manage side effects.
But options for less expensive versions of biologics called ‘biosimilars’ are starting to become available which may bring costs down and increase the range of treatment options.
Find out more
The Psoriasis Association have patient leaflet on biologics (and they also have them for individual drugs).
Read more Evidently Cochrane blogs about psoriasis.
References
- British Society of Dermatologists. Decision Aid for Biological Therapy for Psoriasis. Web. 23 August 2023. Available from: https://cdn.bad.org.uk/uploads/2021/12/29200150/Decision-aid.pdf
- NHS. Psoriasis. NHS.uk, last reviewed April 2022. Available from: https://www.nhs.uk/conditions/psoriasis/
- Psoriasis Association. Biologics for Psoriasis and Psoriatic Arthritis. Web. 23 August 2023. Available from: https://www.psoriasis-association.org.uk/media/InformationSheets/Biologics_for_Pso_and_PsA.pdf
- Sbidian E, Chaimani A, Guelimi R, Garcia-Doval I, Hua C, Hughes C, Naldi L, Kinberger M, Afach S, Le Cleach L. Systemic pharmacological treatments for chronic plaque psoriasis: a network meta‐analysis. Cochrane Database of Systematic Reviews 2023, Issue 7. Art. No.: CD011535. DOI: 10.1002/14651858.CD011535.pub6.
You can join in the conversation on Twitter with @CochraneUK @rtwalton123 or leave a comment on the blog.
Please note, we cannot give specific medical advice and do not publish comments that link to individual pages requesting donations or to commercial sites, or appear to endorse commercial products. We welcome diverse views and encourage discussion but we ask that comments are respectful and reserve the right to not publish any we consider offensive. Cochrane UK does not fact-check – or endorse – readers’ comments, including any treatments mentioned.
Robert Walton has nothing to disclose.
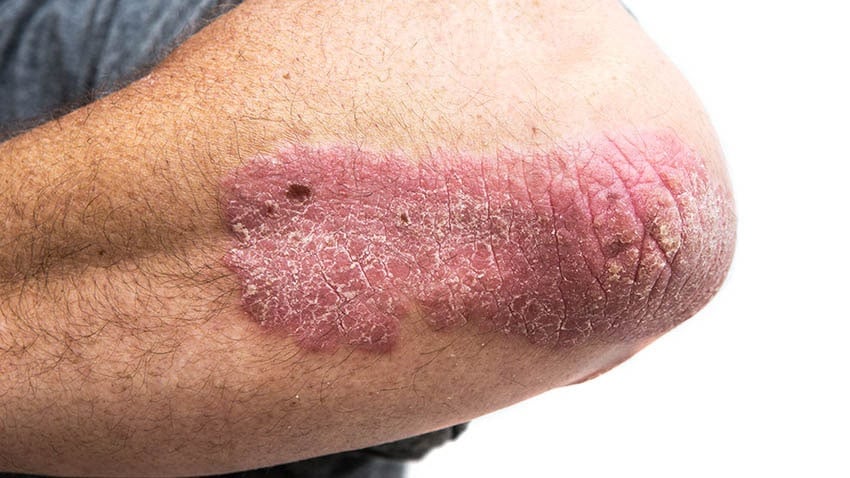
Image credit: ‘Psoriasis on elbow‘ by Hayley Otman, is published under a Creative Commons Attribution 3.0 license.


An informative exploration of biologic drugs for psoriasis! Your evidence-based insights shed light on the efficacy of these treatments, offering clarity for those considering or currently undergoing such therapies.
[…] for psoriasis – are these new treatments any good?’, Cochrane UK, 24 August. Available at: https://www.evidentlycochrane.net/biologic-drugs-for-psoriasis-are-these-new-treatments-any-good (Accessed: 27 November […]
Thank you.