In a blog for a non-medical audience, Lynda Ware, Senior Fellow in General Practice with Cochrane UK, looks at the latest evidence on treatments for cutaneous molluscum contagiosum, a common skin infection.
Page updated 28 January 2022; checked 10March 2023
Take-home points

The evidence is from the Cochrane Review Interventions for cutaneous molluscum contagiosum (May 2017) and is relevant to both adults and children.
Molluscum contagiosum!
Despite sounding like a spell straight out of Harry Potter, molluscum contagiosum is a skin infection caused by a virus called molluscum contagiosum virus (MCV). It is common and can affect any age group, although children are more often affected than adults.
What do the spots look like?
MCV causes raised, dome-shaped spots, usually 2-6mm across, although they can be as large as 2cm. They have a shiny surface and a central dimple and are usually skin-coloured. The spots often occur in clusters and MC spots can appear on any part of the body, sparing only the palms and soles of the feet. They are usually readily diagnosed by their appearance and no tests are needed.
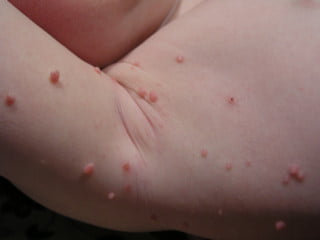
Attribution: Evanherk from nl
This file is licensed under the Creative Commons Attribution-Share Alike 3.0 Unported license.
How do we catch molluscum contagiosum virus?
MCV is highly contagious, in other words it is spread from person to person by touching affected skin. It can also be transmitted by clothes, towels, toys etc which have been in contact with the virus. The virus can also be spread by scratching or picking at the spots. Molluscum contagiosum is more common and often more extensive in people with atopic eczema and people whose immune system is suppressed, for example by HIV infection or immunosuppressant medication, may develop large numbers of spots.
What problems can molluscum contagiosum virus cause?
The infection most commonly resolves over time but it can be doggedly persistent. On the whole, the spots clear within 6-18 months but they can last for several years. If the spots are extensive and/or highly visible they can cause significant psychological distress because of their cosmetic appearance. The spots sometimes heal leaving a scar, especially if they have been traumatised or become infected. They do not usually cause symptoms unless inflamed or infected when they can become painful or itchy. If traumatised the spots may bleed slightly.
How can molluscum contagiosum be treated?
When I was a newly qualified GP (35 years ago…oh dear) one popular treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes. was to poke out the centre of the spot with an orange stick. This aimed to remove the central core, which harboured the virus. Treatments listed in the 2012 NICE CKS (Clinical Knowledge Summaries) for the management of molluscum contagiosum include the following recommendations :
- Treatment is not usually recommended. If lesions are troublesome or considered unsightly, use simple trauma or cryotherapy, depending on the parents’ wishes and the child’s age:
- Squeezing (with fingernails) or piercing (orange stick) lesions may be tried, following a bath. Treatment should be limited to a few lesions at one time.
- Cryotherapy may be used in older children or adults, if the healthcare professional is experienced in the procedure.
This advice is based on pragmatism and expert opinion.
Also :
- The following treatments may be considered by a specialist:
- Surgical (e.g. curettage, cautery).
- Topical (e.g. pulsed dye laser, phenol ablation, imiquimod 5%, cantharidin, potassium hydroxide 10%, podophyllin, silver nitrate paste, benzoyl peroxide 10%, and retinoids).
This advice is based on what CKS considers to be good clinical practice in UK.
Let’s take a look at what the Cochrane Review has to say
In May 2017 the Cochrane systematic reviewIn systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. Interventions for cutaneous molluscum contagiosum was published. The review authors aimed to assess the effectivenessThe ability of an intervention (for example a drug, surgery, or exercise) to produce a desired effect, such as reduce symptoms. of various treatment and management strategies for cutaneous (ie on the skin, but excluding the genital areas) molluscum contagiosum in people whose immunity was not compromised.
Cochrane reviewsCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. are periodically updated and there were 11 new studies to add since the previous version, making 22 in total, involving 1650 participants. 20 of these studies looked at topical treatments and two looked at systemic treatments. Most of the participants were children or young adults.The review considered clinical cure in the short, medium and long term, as well as short term improvement and adverse effects.
Three of the studies included were unpublished (2005) and had been undertaken by 3M Pharmaceuticals, and submitted to the American Food and Drug AssociationA relationship between two characteristics, such that as one changes, the other changes in a predictable way. For example, statistics demonstrate that there is an association between smoking and lung cancer. In a positive association, one quantity increases as the other one increases (as with smoking and lung cancer). In a negative association, an increase in one quantity corresponds to a decrease in the other. Association does not necessarily mean that one thing causes the other.. Together with another published trial, these studies contributed nearly half of the participants (about 800 in all) and compared 5% imiquimod cream to placeboAn intervention that appears to be the same as that which is being assessed but does not have the active component. For example, a placebo could be a tablet made of sugar, compared with a tablet containing a medicine. (a dummy cream).
The other studies considered a variety of comparisons of treatment including cryospray (this is a freezing treatment), 10% Australian lemon myrtle oil, 10% benzoyl peroxide, 0.05% tretinoin, 5% sodium nitrite, 5% salicylic acid, tea tree oil and several others. The quality of evidenceThe certainty (or quality) of evidence is the extent to which we can be confident that what the research tells us about a particular treatment effect is likely to be accurate. Concerns about factors such as bias can reduce the certainty of the evidence. Evidence may be of high certainty; moderate certainty; low certainty or very-low certainty. Cochrane has adopted the GRADE approach (Grading of Recommendations Assessment, Development and Evaluation) for assessing certainty (or quality) of evidence. Find out more here: https://training.cochrane.org/grade-approach for comparisons of these treatments was low (in other words the findings may be true but are likely to change with more clinical dataData is the information collected through research..) There were no randomizedRandomization is the process of randomly dividing into groups the people taking part in a trial. One group (the intervention group) will be given the intervention being tested (for example a drug, surgery, or exercise) and compared with a group which does not receive the intervention (the control group). trialsClinical trials are research studies involving people who use healthcare services. They often compare a new or different treatment with the best treatment currently available. This is to test whether the new or different treatment is safe, effective and any better than what is currently used. No matter how promising a new treatment may appear during tests in a laboratory, it must go through clinical trials before its benefits and risks can really be known. for several commonly used treatments such as expressing (poking!) lesions with an orange stick or topical hydrogen peroxide.
The authors concluded that:
‘No single interventionA treatment, procedure or programme of health care that has the potential to change the course of events of a healthcare condition. Examples include a drug, surgery, exercise or counselling. has been shown to be convincingly effective in the treatment of molluscum contagiosum.’
With particular reference to 5% imiquimod cream, there was moderate quality evidence (in other words this is probably true, but further trial data could change the conclusions) that 5% imiquimod cream is no more effective than placebo in terms of cure, but leads to more local skin reactions where it has been applied. There was high quality evidence (in other words we can be very certain that the conclusions are true) that 5% imiquimod is not better than placebo in bringing about short term improvement.
So what should we do?
No one treatment emerges triumphant from this Cochrane Review. In the majority of cases natural resolution is the way forward. Explanations about how long it may take to resolve, as well as reassurance that there is usually nothing to worry about, will help encourage patience. Trying to prevent spread to others by not sharing towels etc also makes sense but exclusion from sport, school and social gatherings is not necessary. Advice about resisting the urge to pick or scratch the spots will help prevent further spread.
You can read more about it on the NHS pages about molluscs contagiosum.
Molluscum contagiosum!
So, unfortunately, there is no magic wand (or, perhaps that should be orange stick….)
Join in the conversation on Twitter with @CochraneUK @lynda_ware or leave a comment on the blog. Please note, we cannot give specific medical advice and do not publish comments that link to individual pages requesting donations or to commercial sites, or appear to endorse commercial products. We welcome diverse views and encourage discussion but we ask that comments are respectful and reserve the right to not publish any we consider offensive. Cochrane UK does not fact check – or endorse – readers’ comments, including any treatments mentioned.
Lynda Ware has nothing to disclose.



Calamine lotion! After multiple derm visits, unsuccessfully treatment for years, calamine lotion has almost cleared them ip in 2 weeks!
How long do you leave band aids on for after applying potassium hydroxide 10% gel to molluscum
Hi, We can’t advise on this but here is the NHS page on MMolluscum Contagiosum – I think it doesn’t have the answer your looking for, but there is an opportunity at the bottom of the page to comment on how they could improve their information https://www.nhs.uk/conditions/molluscum-contagiosum/
Best wishes,
Sarah Chapman [Editor]
My six year old daughter had mulluscum and they finally healed up, but left behind a white patch of skin when they healed. She has tan skin, and the patches are very pale and noticeable. Any one else experience this?
I did that with my boys when they had it, the one that had the most has lots of pit scars because of it. I did find that clear calamine lotion actually dried them out and made them go away after a few days.
My son seems to have developed a red rash that is spreading fast around his. It’s painful to touch and he’s developed a fever today and is off his foot. We see the go in 2 days..But I’m worries as he’s limping to now in pain and wanting panadol for the pain
I just removed 2 from my daughter arm. They had a hard core center that I had to tear off. It was awful, but the pain lasted for a second she said. I hope she doesn’t get them back. It left an empty hole.
My granddaughter had molluscum contagiosum all over her stomach. I caught her eating a scab from one that she had scratched. Within a few days they were all gone. Her brother and sister had them and we did the same with theirs. A few days gone! I know this is gross and sounds crazy. We have cows ( this was many years ago) and had one that had warts on her and an old farmer told us to shave them off and feed them to her. We didn’t do it but I remembered it after this happened.
Hi, things I’ve learned. Hope it helps.
Peel clothes off so they come off inside out by the sleeves as opposed to sliding them off.imagine the virus like ink-be mindful of what you touch that is potentially contaminated before and after you wash your hands. But don’t err on such caution that you have an OCD manic episode of cleaning. Frustration can make it tempting. Keep a photo journal every couple weeks. Or just journal for mental health too.
Use liquid bandaid to contain the spread and cover high friction areas or places accessible to scratching with a bandaid after it dries, if it is possible to bandage, so as to avoid accidental irritation.
Dimpled raised lesions or pusfilled/recovering lesions can still be contagious until it is a nice sealed red bump that is flattening.
Alcohol must be 70% +for viral effectiveness.
But gentler rubbing liquid soap and warm water are THE best. Pat dry not reusing paper towel but using new paper with each pat.
Keep areas cleaned by gentle showers not baths.
Then when you dry infected areas, use TP/paper towel to dab so as not to spread the virus elsewhere. Moisturizer freely around the rash right after shower. Especially if you have other skin disease, keeping things like eczema under control will be a key help in preventing spread. Drink lots of water (not more than daily recommendations). Then take a qtip and break in half. Drip liquid bandaid on the stick region. Use it to apply a generous amount of the liquid to multiple spots at once before throwing away the tip. Then take a new tip and dip into Vaseline jar (new qtip per dip) and cover dried liquid bandaid spots. If near a joint, cover with bandage so it doesn’t rub onto other area of body. Repeat wash daily or every other day. Wash face daily and make sure to apply liquid bandaid on face before bed so that rolling around on your own pillow at night doesn’t spread it on your face. Wear long sleeves that cling socks if on feet. Wipe down room surfaces daily.
Wipe down sink areas and counters and lights once daily. Change clothes daily and sheets weekly.
Keep your hope alive and be intentional to share mental health concerns of your child and equally you as a caretaker with your dermatologist. Skin disease and its intersection with psychology is real. It’s a marathon of a disease. We can do it!
If bumps are not dimpled/near heading then its safe to gently dry off all those bumps with a cloth towel. Then put towel in hamper. Saves timenif you only do the paper towel drying for the contagious stage bumps.
Directly applying apple cider vinegar (with the mother) on a tiny cotton ball to the spots and applying a bandaid over night completely rid my son of this disease. Zero scarring, absolutely ZERO scarring. He had it all over his trunk, arms and legs. Disease gone overnight, skin looked smooth in less than a week. A flat, red mark may appear the next day but they are clear in less than a week
Did you leave cotton balls on overnight with bandaid over spots or just applied ACV with cotton ball and then coveted with bandaids?
I need some help I took my daughter to her pediatrician and I know this is what she has because my son has a fever too but recently it I think it’s infected it’s all red and swollen and has 2 lumps underneath I don’t want to make the trip to the hospital because of the corona virus and ideas or similar cases? She prescribed her antibiotics
We have exactly the same problem. One very infected lump on my sons leg preventing him running or moving much. We are finishing antibiotics and it’s not done much to help. Also don’t want to to go hospital due to coronavirus… seems not much we can do. Back to doctors today….
I am a mother of four and all my kids got molluscum.. I couldn’t stand seeing the bumps on their skin so after bath I popped them all. As soon as one would come on, I would squeeze it and the core would come right out. By the next day you could barely tell they had any bumps. Just took two out yesterday and my daughter’s leg looks so much better. My pediatrician said to keep doing that, freezing them is more painful and last longer. This is very quick, and even though the kids might cry for a bit the pain goes away within seconds and are very happy to have them gone.
hi, my daughter is dealing with the same, it looks awful. she’s on oral antibiotics but she’s half way done and not any improvement.. what was the outcome? how long did it last? what meds worked? pls help…
Hello, I’m hoping you can help me. My son is 10 years old, and he has never had this before. We tried to talk to the pediatrician about it, but got only the name of this disease and very little information about it. It started as a bump or two, but now has spread from his ribs area, up through his armpit, and down his arm. There’s a few bumps, but it’s more rashy-like. We also thought it was eczema, but now after reading your page, maybe it’s not. I spent $75 on a product called Conzerol, which is a brown cream and soap to wash with.
I’m getting so frustrated now. The whole situation started about 4 months ago. I put the medicine on him before he went to bed, and this morning he woke up scratching! I just don’t know what to do at this point! Is the medicine a good product? If not, I need a name of a good product, not general “get some cream or antibiotics.”
And, on a whole other level of problems, he’s in karate. Like this is his life karate! He competes in tournaments at State and Nationals. When I read that combat sports should be removed from his life on another site, we hit the roof! I really need some help, please!
As Lynda says in the blog, the Cochrane Review found that no single intervention has been found to be effective in treating this condition, and in most cases it will get better by itself.
I’m afraid we can’t comment on products (apart from reporting what the evidence says) or on individual cases; this is something you’d ned to discuss with your doctor.
I do hope your son gets some relief soon.
Best wishes,
Sarah Chapman [Editor]
Go to a dermatologist. My daughter had a cluster under her chin was there for months. I was so fed up. The dermatologist froze them all off with spraying liquid nitrogen on them. They blistered and went away!!! We had maybe one follow up after for one that lingered. But I would highly recommend trying the liquid nitrogen… talk with you dermatologist. Hope that helps!
Put clear calamine lotion it all affected areas! It dried them out and made them vanish in a few days!
avigate this article
What is HPV, and how is it spread?
How effective are HPV vaccines?
Why is HPV vaccination recommended only through someone’s early or mid-20s?
What concerns have you heard about the HPV vaccine?
What about people who don’t want their kids vaccinated because they don’t think the HPV vaccine has undergone enough safety testing?
Are there other reasons that vaccination rates are not higher?
Why is it so important to bring immunization rates up?
I don’t know if you have seen our blog about HPV vaccination, which is here https://www.evidentlycochrane.net/hpv-vaccination/
There is also a recent Cochrane Review on different HPV vaccine types and schedules https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD013479/full?highlightAbstract=withdrawn%7Chpv
Best wishes
Sarah Chapman [Editor]
Hi
My 13year old granddaughter has these and she has atopic eczema as well !
However some of her spots get infected and she has to go on antibiotics
She has a few on her thigh that get infected and her gland in her groin is swollen!
Her dr prescribes more antibiotics!
But surely if the infected spots is re occurring then surely another plan of actio would be best instead of keep prescribing antibiotics??
Hello,
It is good to question whether there are alternatives to antibiotics, but I’m afraid we can’t comment on individual cases and this is something that would need to be discussed with your granddaughter’s doctor.
Best wishes,
Sarah Chapman [Editor]