In this blog, Susannah Hopkins Leisher shares her experience of the trauma of stillbirth and impact on subsequent pregnancies and, with researcher Aleena Wojcieszek, looks at gaps in the evidence on how to care for such women and their families. Please be aware that some may find the content of this blog upsetting.
Editor’s note: people continue to share their own stories of loss in the comments. We are thankful that people are finding something helpful here at a tragic time of their lives.
Page last checked 20 April 2023.

Aleena: the researcher
Some may assume that conceiving a new pregnancy after stillbirth might be somewhat of a “cure” for the trauma of stillbirth; that it’s the inevitable “happily ever after” for families who endure the death of their child, and nothing more needs to be done for these families. But does this really stack up?
When I started my PhD on care in pregnancies after stillbirth, in late 2015, I knew I was entering relatively unchartered waters. I wasn’t sure what I might find, just that it was an area of enormous need.
From my early reading, a few things were clear: stillbirth has profound and sometimes intergenerational effects on families; most parents who have a stillborn baby do conceive again; these parents have a higher risk of (recurrent) stillbirth than parents who have no history of stillbirth; and many parents go through intense anxiety and fear in their subsequent pregnancies.
So what care do parents currently receive in pregnancies after stillbirth? And what care should they receive?
For our recent Cochrane Review on care for pregnant women and their families following stillbirth, we looked for all relevant clinical trials and found only 10 trials with data from just 222 women. They looked only at medical interventions. Not one looked at ways to help parents and families in terms of their feelings and experiences, or how to reduce parental anxiety or promote attachment between mother and baby, for example. It has confirmed a huge evidence gap, rather than provided any guidance on what quality care for these women and their families might look like.
We have much to learn.
Through my studies, I have met many bereaved parents who went through a subsequent pregnancy following perinatal death, mostly due to stillbirth. Their stories are all unique, but there are some common themes across their experiences.
Susannah and Craig Leisher, their sons Wilder and Zimri, and the whole Leisher family, all hold a special place in my heart. Their story has stayed with me throughout my PhD candidature. I’ve even been privileged to share a small part of their story in conference presentations and public research seminars during my PhD, sharing with audiences some of the precious family photos in this blog.
It’s families like The Leishers that this research is ultimately for…
But it would be remiss of me to go on here. I would like to now pass on to Susannah herself to share her story, what this research means, and where to next.
Susannah: the mother
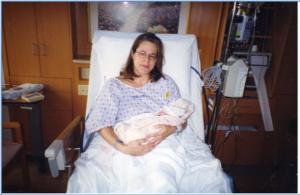
Craig and I started trying for a baby almost as soon as we got married, and I became pregnant quickly and easily. We were living and working in Vietnam at the time. The first time I felt Wilder move, I was in a tiny village in the mountainous region on the border with Laos, doing fieldwork.
I was a new mom, so at first I wasn’t sure – but then it happened again, and I was sure, and thrilled: our baby was real, and making his (or her) presence known! You can see in this photo how excited and happy I was.

The months went by, and my pregnancy progressed perfectly. I was so careful. I eagerly followed the least bit of advice, giving up coffee and alcohol and tracking my weight gain religiously.
About a month before our due date, Craig and I flew back to the States to stay with my parents in Cambridge, Massachusetts, as we had decided to have our first baby back home. On a Thursday, I went for my regular midwife appointment. All checked out. On Friday, I treated myself to a pregnancy massage. On Saturday, Craig and I went downtown to buy sheets. That night, for the first time, I felt a hint of concern.
As we prepared for bed, I mentioned to Craig that I had not felt the baby move, whereas his habit was to move around in the evenings. On the morning of Sunday, July 11, 1999, realizing that I still hadn’t felt the baby move, we consulted our bible, “What to expect when you’re expecting”. It said to drink a glass of juice and wait an hour for the baby to respond to the extra sugar. I made it through about 45 minutes and then we agreed to call the midwife. She was friendly but nonchalant, and told us to go on in to the maternity ward to double-check that everything was okay. On the short drive over to Mt Auburn Hospital, I confessed to Craig how silly I felt, worrying like a stereotypical new mom over nothing.
Nothing. Only the penetrating hiss of static…
In a small room on the maternity floor, the technician smeared the familiar jell on my tummy and began to probe. Nothing. Only the penetrating hiss of static, which I will never forget. Troubled, she smeared more jell on my tummy and tried again from a different angle. She then said she was going to fetch a different machine. I hit the concrete wall hard with my palm and yelled “What is going ON??????” A new person appeared, wheeling a small ultrasound machine. She did another exam, telling us in a monotone, “I see the legs. I see the head. I see the heart. The heart should be beating, but it is not.”
That was 20 years ago. Today, as I type these words, my heart is racing. My grief is ever with me, fresh, just below the surface.
I delivered Wilder Daniel after a two-day induction, on July 13, 1999. The physical pain of my labor was infinitely multiplied as I cried out in anguish, “This is so pointless!” Craig cut the cord. Wilder was 6 pounds, 12 ounces, with a full head of hair and a perfect button nose, as you can see.
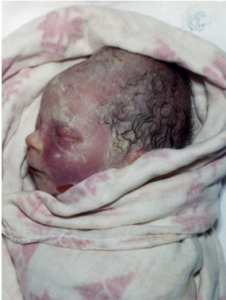
The ‘1-2 punch’ of stillbirth
There was little recognition of the trauma I had suffered, let alone what it might mean for a future pregnancy. I received a piece of paper with a list of local support services and a pamphlet whose title skewered me: “When Hello Means Goodbye”.
Stillbirth gives a ‘1-2 punch’. First, there is the crazy grief of bereavement, and then there are the follow-on effects. For me, these started immediately after Wilder’s death, when our subsequent pregnancy journey began. Dear but ignorant friends told us, “It was meant to be”, and “It’s okay, you can have another baby,” as though that would magically obliterate the actual child I had borne.
There is no expiration date on grief. Each of us is unique and precious, and just because we could never know Wilder’s uniqueness does not erase this fact. Nonetheless, I desperately wanted a live baby and wanted to get pregnant again immediately.
Why did our son die?
We were determined to find out what had happened to Wilder so that we could prevent another tragedy. Craig and I had blood tests done. Nothing. We made the wrenching choice to allow an autopsy to be performed on Wilder’s body – maybe that would give us some answers. Nothing, other than the cruel enduring worry over whether his body had been respected and treated gently.
We were advised finally to consult with a perinatologist. We eagerly prepared “The List” for our meeting with him. On it, we included every factor we could possibly think of that might have killed our son. In the event, the perinatologist accepted our piece of paper, glanced unseeingly at it but did not even read it, and told us that “sometimes these things happen”. A poster child for fatalism about stillbirth in healthcare professionals!
Ultimately, we have had to live with not knowing why our son died. This fundamentally shook my confidence in what science and medicine can do for me.
The short-lived joy of being pregnant again
I became pregnant again almost immediately. I was full of joy but it was short-lived. Where my first pregnancy was thrilling, secure, and joyful, my second pregnancy was wooden and defenseless. If death could strike randomly once, it could do so again, and there was apparently nothing I could do to stop it.
We again elected to return to the States for the birth, to the same hospital where Wilder had been born dead. I asked for extra monitoring and was told it wouldn’t make any difference but I got it anyway. Wilder had died at 38 ½ weeks. I could not bear to go past this date and asked for early induction. My understanding obstetrician allowed it.
One reason I wanted to return to Mt Auburn was my bereavement nurse, Patty Campbell. Patty was with us when Wilder was born and she was the only person I connected with during my heartbreaking labor. She put Wilder in my arms. She took our precious photos of him. She asked his name, and when it was time, she asked if I was ready to let him go, and she understood when I could not answer her, because what mother could ever answer “yes” to that question. I needed her there when our next child was being born, because maybe that one would die too.
Zimri Bhai – little brother
Zimri was born on August 7, 2000. Apparently, he was born with the cord around his neck. It took a while for him to cry. I wasn’t surprised. I felt grim.
Then he cried and Patty brought him to me but I couldn’t smile at first. I felt solemn and icy and unemotional. I felt that he was probably going to die. Patty kept at me until I kissed this new living baby and I did smile then. Zimri’s middle name, Bhai, is the Nepali word for “little brother”.
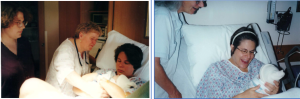
It took me months to call the new one by his name. I probably accepted that he was actually going to live when he was about six months old.
I had two more pregnancies with two more living babies, my sons Kai and Ilem. Each pregnancy was less wooden but with the specter of possible death ever-present. No one ever again can tell me “it will be okay”, because I know that sometimes it isn’t.
What we still need to know about pregnancy after stillbirth
This Cochrane Review is important first because its very existence makes a statement to the healthcare community that subsequent pregnancy after stillbirth must be an area of concern. Subsequent pregnancy is not a cure for the trauma of stillbirth. It’s its own new and hugely complex life event.
Today we have a much better understanding of how stillbirth affects families and communities than we did in 1999, when my son died, but there is so much more work left to do, as illuminated in this review.
“It wasn’t meant to be” and other platitudes are not helpful. There is always a cause and it’s science’s job to find out why. We need to know the causes of deaths to help families understand and to help provide care in subsequent pregnancies. As this review shows, though, research on medical interventions to reduce the risk of recurrent loss is incredibly limited. Worse yet, in my view, is the near-complete lack of research on psychosocial interventions that can help women and their families navigate subsequent pregnancy, childbirth, and life with living children beyond.
I am permanently scarred by Wilder’s death. I and my loved ones have done our best to make our way and seek help and advice, but it has sometimes been a hard road. The medical community needs to understand that parents have unique needs in subsequent pregnancies, yet as this review shows, more research is needed to know what’s helpful for different types of families and situations. For instance, for me, planned early birth was crucial (none of my kids went past 38 ½ weeks, thanks to understanding doctors in three countries), and yet this brings its own risks, so we need more research to help understand and compare the risks and benefits of this intervention.

Wilder’s 20th birthday would have been July 13, 2019, around the time I started writing this blog entry. My three living sons remember him every year as they tend to him on the family altar, a practice we learned from our time in Vietnam. Wilder died so long ago, and yet my trauma remains with me, always just below the surface. This important review illuminates the complex mix of actual tragedy and potential joy that is subsequent pregnancy after loss, the woeful state of knowledge about what can help families, and the importance of action.
Some support groups
- https://firstcandle.org/online-support-groups/
- http://nationalshare.org/online-support/
- https://www.mend.org/virtual-support-group-links
- https://starlegacyfoundation.org/support-groups/
Stillbirth Advocacy Working Group
The Stillbirth Advocacy Working Group (SAWG) is a group of bereaved parents, clinicians, researchers, and others who are interested in raising awareness of stillbirth globally so that we can help end preventable stillbirths and ensure appropriate respectful care when these deaths do happen. SAWG is co-chaired by the International Stillbirth Alliance (ISA) and the London School of Hygiene & Tropical Medicine (LSHTM).
Susannah Hopkins Leisher and Aleena Wojcieszek have nothing to disclose.
Reference and further information:
- Wojcieszek AM, Shepherd E, Middleton P, Lassi ZS, Wilson T, Murphy MM, Heazell AEP, Ellwood DA, Silver RM, Flenady V. Care prior to and during subsequent pregnancies following stillbirth for improving outcomes. Cochrane Database of Systematic Reviews 2018, Issue 12. Art. No.: CD012203. DOI: 10.1002/14651858.CD012203.pub2.
- Sands is a stillbirth and neonatal death charity providing support, as well as a list of organisations for anyone affected by the death of a baby: https://www.sands.org.uk/usefullinks
- Readers may also be interested in Something good enough, by Tamarin Norwood. Her moving essay reflects on the birth and death of her son, who died shortly after his birth.



Hi, I’m Geraldine from Papua New Guinea. Lost my baby at 30 weeks: 15/05/2021. I was 25 years old. It’s now 2years and I am really trying to get pregnant again but it doesn’t work out. Could you please help me in this matter?
Thank you,
Best regards
Dear Geraldine
I am so terribly sorry for the death of your baby two years ago. I remember myself when I was trying to get pregnant again after the death of my first son Wilder. It was very stressful and a hard time. I am so sorry for the delayed reply. Geraldine, there are a few resources that might be helpful for you. You can look over the Australian Stillbirth Centre of Research Excellence website at https://stillbirthcre.org.au/ and also their support page here: https://stillbirthcre.org.au/parents/care-after-loss/support-groups/ There is an organization, the Burnet Institute, which works throughout the Asia/Pacific region including in Papua New Guinea including on maternal health issues (https://www.burnet.edu.au/global-impact/where-we-work/papua-new-guinea/). I would be happy to reach out to my contact there to see if there are suggested providers who could help you with pregnancy after stillbirth in PNG–please email me privately if you would like me to do this (shleisher@aol.com). Sending my best wishes to you,
Susannah
Immune thrombocytopenia (ITP) affects 0.1 to 1 per 1000 pregnancies and severe ITP, with platelet counts less than 10,000/µL, is difficult to manage.
Two pregnant patients with ITP who were successfully treated with thrombopoietin receptor agonists (TPO-RA) at a tertiary institution are discussed.
The first patient had chronic ITP, achieved complete remission with eltrombopag, but was resistant to intravenous immunoglobulin (IVIG) and steroids in her second pregnancy.
Romiplostim was effective, and she had an uneventful cesarean section.
The second patient responded well to eltrombopag at 35 weeks of gestation and had a vaginal delivery.
ITP in pregnancy is managed based on clinical expertise, and TPO-RA use during pregnancy is largely from case reports.
For severe ITP, eltrombopag or romiplostim from around 34 weeks can be used if other treatments fail, with a goal of achieving a platelet count of over 80,000/µL.
The mother’s response to medication may vary in different pregnancies.
Induction of labor may be appropriate in some cases.
See More: immune thrombocytopenia
Hi and thank you for your story and work in this area. I lost my son Freddie in Nov 2022 at 26 weeks. His heart had stopped beating and I noticed he had stopped kicking. The sense of helplessness is unbearable and it truly demonstrates just how fragile that tiny spark of life really is. I am pregnant again now with my second pregnancy (6 weeks). I was interested to see how you found hot weather and air travel with your living children. Myself and partner had a holiday to Greece and don’t want anxiety to get the better of us. We travel in our second trimester.
Thank you, Jen :)
Dear Jen,
Thank you and I am so very very sorry for the death of your son Freddie. I totally relate to the feeling of helplessness. It is so scary being pregnant again. For me, the support of my partner Craig and my family and friends, and my work colleagues, helped me to manage through my second pregnancy, but it was months after Zimri was born (my oldest living child) that I finally believed he would live. It is such a long road. It is wonderful you have a holiday planned and I would say go for it, as long as your doctor thinks it would be fine. I lived in Vietnam all during my first three pregnancies so hot weather was a given and not a problem for me, but I am sure it depends on the individual. Maybe ensure you have access to air conditioning. Also I always carry a paper fan. It is incredibly useful when I’m getting overheated. Air travel with my kids was necessary given we lived overseas (first Vietnam and then Australia) so we did a lot of long-haul (including 15 hour) flights. Not fun but definitely doable. And way better when they are younger and will sleep. Very very best of luck to you. Wishing you hope and peace,
Susannah
My sweet baby boy, Hudson, was stillborn January 10, 2023. He was 32 weeks old and perfectly healthy. The night of January 8 I had a bad feeling like something was wrong. However, being the worrier that I always have been, I dismissed that feeling since I felt Hudson kick and went to sleep. I woke up January 9 still feeling concerned. I tried all the tricks to make him move, but he wouldn’t. I still didn’t assume the worst because he had been known to not move a ton throughout the entire pregnancy. I coincidentally had an appointment already scheduled for that morning with my OB. Everything about that morning just already seemed so off and unsettling. We went back like normal for our routine Doppler check and chat with the doctor. As soon as the doctor touched my belly with the Doppler, I knew. He had a slight look of panic in his eyes and I immediately freaked out. Ultrasound then only confirmed the news. I replay these moments and mine and my husbands reactions over and over. I delivered my beautiful baby boy January 10 at 1136. He was 4lb 2oz and 17 inches long. He and I both checked out to be perfectly healthy, and all other tests since have indicated nothing but the perfect picture of health. We don’t understand. I can’t stop reliving the whole experience over and over in my head. Like you, I want to try to have a baby as soon as we can, not to replace Hudson, but to fill some of this void. I was supposed to have my baby boy here with me. I’m terrified of this happening again and again with future pregnancies. I can’t imagine not trying though. I continue to pray every day that God will allow us to bring home a healthy, living baby one day soon.
Dear Darienne,
I am terribly terribly sorry for your son’s death. It rings all too familiar. I know much of what you went through. I have taken so long to reply because my beloved mother died on February 2 and I am now the caregiver for my father who has Alzheimer’s. My only sibling, my younger sister Alyson, died suddenly in 2014. So death seems my constant companion. I share this because I can tell you with even more certainty now that my experience is that the terrible grief marches forward alongside the rest of my life, with ‘the rest of my life’ slowly becoming larger and the terrible grief never gone, but the forward march through time allows it to become less prominent, less excruciating, in comparison to ‘the rest of my life’. What I mean is that the passage of time does appear to soothe, even when nothing else helps.
Sending wishes for hope and some peace, in solidarity,
Susannah
Hello, my name is Delia. I’m from Istanbul. And I have just lost my son 3 days ago, he was at 20 weeks. I was at the hospital a week before his death and he was perfectly healthy. His heart has stopped beating in one week. I had a perfectly healthy pregnancy before this moment. I still don’t understand why this has happened to my baby. Doctors reply was just sometimes this happens
Dear Delia
I am so so sorry for the death of your precious son. It is now 15 days ago. I remember very well the pain of that time. As with your situation, we also were told that ‘sometimes this just happens’ and it happened after a perfect pregnancy. It’s not true that death occurs without reason. There is always a reason, usually more than one, but unfortunately the science has not caught up with our reality yet. There is so much work to be done to investigate causes and ways to prevent more babies from dying. I am so, so sorry that this has happened to you and your family. I wish you peace, and I hope that you are able to find others who have faced similar losses, as it can be so relieving to talk to others. Courage to you,
Susannah
Hello, thank you for your story. I just lost my first baby at 25 weeks on May 9 2022. Like you, we got pregnant immediately. We got married October 2022 and conceived November 2022, our first time trying. I had an anterior placenta so I didn’t feel him much but I had an at-home Doppler. I couldn’t find his heartbeat on May 7 2022 so I went to the ER. That is where I saw the ultrasound and saw the hole for his heart – not beating. I’ve done ever test and I have no answer.
My life feels like a cruel joke. It seems I can’t escape happy families and pregnant women. I don’t know how to even work through these thoughts and feelings. I’m in therapy and a support group but there’s no cure for this experience. I’m convinced it’s found to happen again, and again, and again, if I am even fortunate enough to get pregnant again.
I’ve read all your replies and thank you for creating this community. I wish us mothers got a pass from death for future pregnancies.
Dear Maryam,
I’m so sorry to know of the death of your baby. As you can tell from reading my story, I know how it felt when I found out. A dreadful, cruel joke. Something that simply cannot be, but it was true. So shocking and so hard.
I’m glad that you found a support group. It can be a way to navigate through time to a point where it is more bearable to live with your loss. There is no cure. Only time marching forward. It is so harsh to have to see happy families and pregnant women and babies. They seem to be all around us. I remember so well, the first time that my husband Craig and I had dinner with our friends who were also pregnant at the same time as me, only they had a healthy baby girl and we had our dead Wilder. Their lovingkindness overflowed for us. When we came over, they had put away every hint of baby in the house, and their daughter was fast asleep in another room. We didn’t mention anything about babies during the whole visit and it was such a generous kind gift they gave us, the relief of not having to face it. At the end of the evening I did peek into their daughter’s room for a moment but that was on my terms and it felt okay, just for that moment.
Sending you fellowship and wishes for strength and courage to move forward in time,
Susannah
I lost my baby girl, Lucía, on January 25th, 2022. My pregnancy and my baby were healthy, as many women here. I went to the doctor the day before everything was normal, in the afternoon I started having back pain and mild contractions, which I thought they were Braxton’s. Later that day I went to bed, felt the baby moved, and felt asleep, later I woke up a few times with pain and urge to use the restroom, I realized I was in labor, started timing my contractions and got ready to head to the hospital. When I got there there was not heartbeat, I was 38 weeks along, I gave birth to the most beautiful girl. After the autopsy, nothing was found. I still don’t know why it happened or if we could of prevent it. We will try again soon. I miss my baby girl everyday, and I will hold her in my heart forever.
Dear Adriana,
We’re so sorry to hear of the death of your precious daughter Lucia, and that you don’t know why it happened – that must be so hard. Thinking of you and sending all good wishes to you and your family.
Sarah and Selena [Editors]
Dear Adriana,
I am so terribly sorry for this devastating loss of your beautiful daughter. I too know the pain of not knowing why it happened, as my son Wilder Daniel’s cause of death was unknown. I send you my wish for strength and peace in the months ahead. (Also I am sorry to reply so late as I was on leave.)
Sincerely,
Susannah
I lost my son last october 31 2021 34weeks/5dys. It hurts me the most when none of my Ob’s knw what really happned😭. They couldnt gve me an accurate ans once I was told the cause of death(abruptio placenta sort of) since she (ob) wasnt the attending doc that time. Not around bec that day (oct 31 2021) was his son’s bday😭
Ps. I was admitted at the hospital 0ct 30 2021
Dear Mae,
I am so very sorry for the death of your son. It is a terrible thing. The story of the cause of his death and the doctor’s not being available is so very hard to bear. I feel your pain. I send my wishes for the passage of time to ease your heartache.
(Also I am sorry to reply so late, as I have been on leave.)
Sincerely and sending strength,
Susannah
I have four kids all of them from c-section. I can feel that pain of loss, a great article that helps in many ways GOD bless all women who have been through this.
Dear Sophia
Thank you so much for these very kind words.
Warm thoughts to you,
Susannah
I just lost our baby girl at 20 weeks. I’m utterly devastated. My husband also is In so much grief. I went In for a regular ob appointment and they couldn’t find her heart beat. It doesn’t feel real. She was born at 11:08 ( the same time I was born) aug 12 2022 . I laboured her out for 16 hours and the cord was wrapped around her neck three times.
Dear Rebecca,
I am so sorry to know of the devastating death of your daughter. Your loss is so very fresh and at the surface. I hope you are surrounded by love and support. For me when the grief is closer to the surface it is helpful to feel the community of those who understand or have the capacity to empathize with our tragedy. Sending strength in the days to come,
Susannah
Hiii
All your four CS is whithin howmuch time gap…
Howmany still birth you have…
We lost our fourth child on November 16th at 25 weeks to Bilateral Renal Agenesis. We had a delay in our 20 week scan which meant that we were excluded from the RAFT trial. With that it all seemed so useless to have extra scans and so on. We had the grace of knowing ahead of time that he was going to pass and that no matter when he was born that the outcome was never going to be different. However, it didn’t make those first few days afterwards much easier. We are still waiting on genetic results from his umbilical cord to see if it is a factor which we will have to be mindful of in future pregnancies. And even though the odds are in our favor that it was a spontaneous event it still makes us nervous that something could happen again. We never had a thought cross our mind that something like it could even happen at all considering our 3 other children and pregnancies were perfectly healthy. I personally think we need to move up the standard 20 week scan to 16-18 weeks across the board, that way if there is a delay like one we faced that the parents will have a chance to enter a trial or some other form of care if their child has BRA, etc.
Dear friend, I am so very sorry to hear about the death of your son and the surrounding circumstances. It is a truly terrible shock that none of us is ever prepared for. Sending wishes to you for peace and strength,
Susannah
Hi Susannah,
I too recently experienced a loss of a child a little girl, Alianna. She had been the pregnancy that i had longed for. Everything was going great. Every doctors appointment was all normal my girl had a very strong heart beat. Last week Wednesday i left work early because i hadn’t felt her move. Friday i gave birth to my princess and unfortunately the umbilical cord was the cause of her death. It has been the toughest pain i have ever had to endure. Today marks a week that i gave birth to her, and it never gets easier. We were 7 months along and the day we went to the hospital her crib had just arrived and i was si eager to see it built.
My question to you is while i was reading your article i read that you got pregnant almost immediately, how long after did you get pregnant ? We are also desperate to have another chance of having a baby of our own once again
Hello Tatiana, Susannah has sent us the following reply to post here for you (technical problems with the site mean she’s been unable to reply directly). Sarah [Editor]
“Dear Tatiana,
I’m so very sorry for the devastating stillbirth of your baby Aliana. It is still so recent for you… Yes, for me too, I wanted to get pregnant again right away. However I had tested positive for TB during my pregnancy with Wilder and I was told I needed to be treated for TB before trying again. We visited an infectious diseases specialist soon after Wilder was stillborn and she explained the usual treatment course takes 6 months but they had just introduced a newer treatment that took ‘only’ three months. I was extremely upset to have to wait that long and I remember crying in the parking lot outside the doctor’s office. Once the treatment was over, we started trying again immediately and I ended up becoming pregnant right away with my oldest liveborn son Zimri (who is just 13 months younger than Wilder). Everyone is different of course. Some people do not want to try again at all, some want to try but later, and some want to try right away. Of those who try right away, some have an easy time getting pregnant again and some have a very difficult time or it does not happen at all. And then there is the subsequent pregnancy itself, such a morass of emotions. Anyway, for me it was just 4 months later. That subsequent pregnancy was so different from my first. Wishing you strength and courage in the days and weeks ahead, Susannah”
Hello,my name is abigail.i have read so many heart touching stories from different mums going through truamas similar to mines.i appreciate those mums for sharing their experience.i already have a duaghter who is 1year 5months now.was expecting my second baby.i refuse to know the sex of baby until delivery day.my last check with the doctor says everything was fine with the baby.at 28weeks 6days I notice something was wrong,your Tommy have reduced said my husband and I wasn’t feeling the movement of the baby.i was worried.that was on Saturday night,we called the doctor,but couldn’t reach him so decided to wait till the next morning.by morning I started feeling pains under my stomach and my waist.when we got to the hospital,doctor checked the baby and said there was no water in d sac and no heart beats.my baby is Dead.at first I was shocked,I refuse to accept the news.i was crying I told him that my husband checked for the baby’s heart beat last night and baby was fine
i was crying intensely because unlike my 1st pregnancy this one was very different in everyway.i was always on pains,weak,bedrest I was told to stop working.i was always careful in everything I do.had to under go a surgery where my celvix was stich to prevent possible miscarriage.immediately I was induced.as i was passing through the painful labour i was crying and thinking about the sad reality of not birthing a life baby.i couldnt belive it.i still have it in mind that the baby will cry immediately it comes out.i finally push out the baby,no cry,I was disappointed and couldn’t look or even ask about the sex of my baby. whenever I think about it all am emotionally down I can’t sleep at nights.the thought of how could this have happened?am the cause for not resting enough,for stressing myself.what I should have done to prevent it.this happened on the 30th of August 2021.till now still trying to recover.it just difficult being pregnant and going back home with out a baby.some persons still ask me,have you delivered?hmmmm so sad.
Dear Abigail,
I’m so very sorry to hear of the death of your baby, so very recently and so devastating!
I completely relate to the total unbelievability of the death of your baby—it seemed unreal when Wilder died, yet terribly real and true at the same time. Being sleepless and tormented by how this could have happened. Know that it was not your fault!! It is so incredibly painful when people ask about the baby. I remember coming back to Vietnam (where I lived at the time that my son was stillborn, but I had returned to the US to deliver him). Everyone back in Vietnam was expecting me to return with my newborn baby. We got picked up at the airport by a friend and driven back to our house in Hanoi, and we got out of the car, and immediately our neighbors saw us and called over to us, “Where’s the baby?” I yelled back, “The baby died!” and went inside. It was so raw. They didn’t know and they didn’t mean to cause pain, but there was so much pain… I can only say that moving forward in time, day by day, brought me farther away from the acuity of it and I hope that moving forward in time will bring you a bit of peace and rest. Sending strength and courage,
Susannah
My baby boy’s heart stopped beating at 25 1/2 weeks and I delivered my son Hank (Henry is his official first name but we were planning on calling him Hank) a few days later on June 8, 2021. I really appreciate the original article and reading everyone’s stories in the comments. I have two living children (almost 5 and 2.5 years old) and my 20 week ultrasound and the pregnancy in general had been smooth and without complications. I was so scared of something going terribly wrong with my oldest daughter’s pregnancy since we had an early miscarriage a few years before I got pregnant with her, but everything went very smoothly with her pregnancy, birth, newborn days, etc even though I was always anxious. We had another smooth pregnancy/birth and I assumed this third child would also join our family safe and alive.
I was out of town visiting a friend when I realized I had stopped feeling regular movement/movement at all. I was awake most of the night begging my baby to move even a little bit to let me know he was ok. I downloaded one of those heartbeat apps that may or may not actually work and heard nothing but my own heartbeat. I caught my flight home the next day as scheduled (it felt like the longest day of traveling ever…) and a friend met me at the airport and took me to the hospital to be checked since my husband was with our kids and we didn’t want to change up their routine any more than we already had with me being out of town. A nurse tried to find the heartbeat with no success, then the doctor came in with the ultrasound machine. After a few seconds I knew he had died before she said anything–a hot wave sensation ran through my body as it really hit me then she said “I’m sorry, but there’s no heartbeat…” I didn’t even cry at first. I just sat there kind of puzzled like “huh… so this is what it is like to find out your baby died…” My next thought was how I’d rather do anything else in the world than tell my older daughter that her brother had died. He was all she talked about for months and months and she had so many plans for how she’d help him and love when he arrived. I finally started to cry when I thought about telling my daughter the news.
We were able to go home for the night since my body was fine otherwise (never had cramping, bleeding, or any indication something was out of the ordinary other than no baby movement) and checked into the hospital the next day in the early evening for the delivery. I took some pills that induced labor and the next morning at 5:50am he was born. He came out inside the sac of water fully intact with the placenta. It was incredible to look at, if you could get around the fact that inside the perfect sac was my perfect son who was no longer alive. The doctor broke the sac, wrapped, him up and gave him to me to hold. He was absolutely perfect. Every single part of him was tiny and beautiful. He had blond hair just like my younger daughter and I wonder if he would have grown up to look like her. His toes were the same as my other two kids. Once he was born the doctor pointed out that there was an obvious problem with the way the umbilical cord had grown. It was big and normal looking until right where it entered his body where it was very small and constricted. The doctor said there was no reason why that happens and it is very rare but it can sometimes grow in such a way where eventually the baby couldn’t be sustained by the blood flow the cord supplied. The 20 week ultrasound showed no problem with the cord since the three vessels they check for were present, but the cord had grown incorrectly for some unknown reason. Seeing the issue with the cord did provide me with some peace of mind because I had been beating myself up for traveling and going on a hot walk that afternoon before I stopped feeling movement even though every single doctor I talked to told me that couldn’t have been the cause of his death. Once we saw the cord, my doctor pointed out that no travel or walk could have caused it to grow like that, it just grew like that over time for some reason. We didn’t go through with an autopsy or genetic testing since my doctor said that we likely wouldn’t learn any more information than the cord had grown incorrectly which we could see just by looking at it. My parents were able to bring my kids to the hospital to meet their brother which was so special. My husband and I spent the day at the hospital with him then left to go home that evening. Having to decide when we were “ready” to leave was awful and something no parent should ever have to do but it felt as right as it would ever feel to us.
The last month has been a whirlwind of raw feelings. I am so sorry there are so many people here sharing similar stories. We do want to get pregnant again, but going through another pregnancy feels like signing up for the most vulnerable thing possible. I am so jealous of people who are pregnant and assume they’ll bring home a healthy baby then get to do it. I was that person with my second pregnancy and I am jealous of my past self. I was that person with this pregnancy until everything ended so abruptly and tragically. I appreciate everyone sharing their stories.
Dear Stacey,
Ohhhhh…. I am so so sorry for the death of your beautiful son. Thank you so much for sharing your story. As you know perhaps from reading my story, this is the end of the week in which I remember my own son Wilder Daniel most acutely, as it is the week he was stillborn 22 years ago. Many parts of your own story are so similar to mine. I completely remember our bereavement nurse Patty asking me if I was ‘ready’ for her to take him for the last time. As I have written elsewhere, I did not answer her, because how could I ever answer ‘yes’ to such a question? It is her tender skill which allowed her to know when it was permissible for her to take Wilder from us, without her forcing me to verbalize any answer to that truly terrible question–knowing that it would be the last time we would ever see him. I feel your anguish Stacey and I can only say that time progresses forward. A dear friend told me that just this morning, “what choice do we have” but to continue forward, and we do. It is our fellow members of this crazy community of loss who help us, knowing that at least, we are not alone. Stay safe and have courage,
Susannah
I lost my baby boy, Charlie, on June 7th, 2021 he was 26+5 weeks. My pregnancy had been completely normal, all the scans and ultrasounds had come back with no causes for concerns. The morning before my husband and I were supposed to go to Hawaii for our babymoon I woke up at 3:30am with my sheets soaked in blood. When we got to the hospital they checked his heartbeat and said it was fine but wanted to keep me for monitoring since they couldn’t figure out what caused the bleeding. About 3 hours later I began bleeding again but this time when they checked his heartbeat they said it had dropped and I had an emergency c-section and within that 10 minutes from when I was bleeding to the surgery he was gone. Afterwards they told me I had unicornuate uterus and when we received our autopsy results it revealed that I had velamentous cord insertion and that while my son was in the 80th percentile, my placenta was only in the 10th percentile, they said the combination of these is likely what lead to his death. I want to have another baby but I am so scared that the same outcome will happen, that my body will once again not be able to safely grow a baby and the thought of adding more grief and heartbreak from another loss is terrifying.
Dear Courtney,
I’m so terribly sorry for the death of your baby. Your story is just devastating. It happened so very recently, just 5 weeks ago. In fact, you posted on the 22nd anniversary of my own son’s stillbirth, Wilder Daniel who was stillborn on July 13, 1999. The trauma of your son’s birth… and your fears about what might happen again… I can hear those fears, and while I did not have the same experience that you did, I remember the fears for myself of ‘what now’… I hope that you have a doctor or midwife or other healthcare provider whom you feel you can connect with, to listen to you and discuss your thoughts and concerns. It’s so important to have someone you can trust, and so hard when there are no answers. My heart goes out to you. Wishing you strength in these hard hard days,
Susannah
My name is Elisa and I gave birth to our sweet Ava Mae who was born sleeping at 38 weeks and 4 days on May 15th this year after discovering there was no heartbeat at a routine doctor’s appointment the day before. At 37 weeks, I had an ultrasound because I was measuring small at 36 weeks, which was strange since I had been right on track all along. The ultrasound went fine and they determined that she was “just small” and not growth restricted. We got to see her heartbeat on the monitor, and her measurements were proportionate and the technician said she had plenty of fluid- nothing to worry about. We relaxed, but 10 days later on May 14th we got the horrible news. I had started feeling her slow down a bit but we were still feeling her move enough, but looking back on the few days leading up to it, I just know that something wasn’t right. I will always feel like I did not know enough or do enough. It was my first pregnancy and I just did not know and did not want to over-worry. It is my biggest regret. We will likely not get the answers we are looking for and the doctors can only guess it was some kind of cord accident, although she wasn’t born with it wrapped around. We have had many tests that can not confirm a cause. On all accounts I was healthy and so was Ava, even with her small size. I recount those last days and can’t stop over analyzing if I did not see the signs that something was wrong. I will never know if I could have saved her or if this truly was a terrible accident. We are confused and angry at times, we were so close to bringing her home. Thank you for sharing your story and for continuing your work and spreading information and hope to families who have experienced this loss. There is still so much to learn yet. It brings me hope for the future that we will be able to give our Ava healthy living siblings. We know a subsequent pregnancy will be extremely challenging, but we are committed to bringing a healthy child into the world.
Dear Elisa,
Oh, I am so sorry for the devastating death of your dear daughter Ava Mae. As you know from reading my story, I can relate all too well. The perfect pregnancy, the perfect last check-up (mine was with a midwife the Thursday before we found out that Wilder had died, on a Sunday), the immediate start of cataloguing every possible thing we could have done–or did not do–that might have caused his death, and now, 22 years later almost to the day (July 13 is fast approaching and every year it is hard), I have had to adjust to the permanence of not-knowing. I am so sorry for your terrible loss. I can only say that as each day progresses, the nature of the grief shifts and things become more bearable. Thank you also for sharing your story. All over the world, mothers and families whose babies have died find some strange and ironic comfort in knowing that–sadly–we are not alone. Wishing you strength and courage in the days and weeks ahead,
Susannah
Hello my name is Diana from France , in October 2020 after our 1st year of marriage , my husband and I found out I was pregnant. So excited and nervous at the same time but so deeply in love since I knew we were expecting our beautiful baby.
I gave birth to a stillborn beautiful baby girl , on May 16th 2021 , at 35 weeks+ , her name is Camille and first baby . My whole pregnancy was perfect , I had no healthy problems , my baby girl was developing in the right way through the pregnancy , I did all I should do during this time and take care of my self , my doctor never reported a problem during our appointments / ultrasounds just the 3rd ultrasound (33w+) the doctor remarked that will programmed at week 37 a 4th ultrasound because my baby already weighted 2.460 kg (4.409 pouds) and I could be induced earlier from my due date June 22nd 2021 but it never happened .
On Monday May 10th 2021, I was so excited because I was going on maternity leave from work , normally she liked to moved in the night but this day in particular moved a lot during the morning ( I thought she was excited liked me, because we were going to take a break ) between this day until Thursday , May 13th 2021 I was at home preparing the final stuff before her arrival as Mom I had this feeling something was not right I didn’t feel her moving at all , my husband and I went to the hospital in the afternoon shift , a midwife on this shift attended us and explained I did not feel at all the movements of my baby , she checked with 2 Doppler machines and brought another colleague and I remember asking why they don’t find the heart beat of my baby??!! , all naive I told them my doctor with the Doppler quickly finds my baby’s heartbeat , They said will bring the doctor in the night shift (ours was on vacation) .
The midwives sent me to the ultrasound room , the doctor came in… and 5 seconds after said without any filter, tactless to my husband and me: indeed there is no heartbeat of the baby!!! . I felt my world fell apart and one part of me died with her… this day changed my life forever a long with the day I gave in birth my baby ( induced giving birth naturally 2 days after to my baby) , those days I will never forget.
It has been 1 month + 5 days already since I gave birth to my beautiful princess and truly speaking it has been very difficult , a situation I don’t wish any one to happen or pass through.
After a month we got the results of my little baby Camille´s autopsy ( it was a hard decision to make) I needed to know what happened , what I have done to her ?? , all this guilty.. Our doctor came back from his vacation and the first thing he said , I’m so sorry for your loss ,I’m very touched for what had happened to you I know how much you loved Camille ( he showed empathy, all the opposite from that night shift doctor gave us the first unforgettable and horrible news of our lives) …complementing that they had not found anything in my baby, that she was a perfectly healthy baby that the only thing they had found in the placenta was a bacteria, that they do not know how it had gotten there , since there is not source of infection by any of the possible routes, all my tests were negative or within normal values the bacteria is ruled out as a factor that has affected my baby, since it was in a very early stage and the amniotic sac never broke … leaving the same unknown ,sadness and emptiness as a fathers.
Here I’m as many mommies ,sharing my history and experiencing the pain of losing my healthy and perfect baby girl Camille..and asking me why…why her ? It so hard to wake up every day and know she won’t be here and coping the rest of my life with this emptiness in my heart .
Dear Diana,
Your terrible story brings back all my own memories. Our stories are so similar, and the 22nd anniversary of my baby Wilder’s birth is just a few weeks away, so I think back to this time in my first pregnancy, 22 years ago, when I too was so terribly naive, not knowing what could happen and what does happen to so many mothers and families. You are in a dreadfully hard part of your grief right now, still so fresh, and I am so sorry. There truly are no words, only as I have said before to others, to continue moving forward in time. Things change and it becomes easier to bear and more manageable. I am so sorry you have lost your darling Camille. You are not alone. Others reading your words here can also know what you went through and are going through, because we have gone through it also and are still going through it. Wishing you comfort and courage,
Susannah
I gave birth to a stillborn son, five days before his due date, this May 2021. Everything was going well during pregnancy, full bloodwork was good, no concerns, no gestational diabetes, regular checkups, ultrascan showed a lively happy baby. May 10th, I woke feeling sad, crying, and just very emotional, but he was still moving with regular, frequent kicks – my babies are usually quite lively, and so the fetal movement count was great. Perhaps it was premonition or mother’s intuition, but while all was well, I was so emotional that it concerned me. I had a breif nap in a sitting position, carefully, and when I woke up he was too quiet. No kicks. But wiggles – occasionally – or so I hoped. My body began to have mild contractions, then by 8:30 am the next morning I was in full on labor. I didn’t tell anyone. My midwife called to see if I wanted to come into the hospital. I said no. Why? Becuase of covid. Not the disease but the hospital policies that refuse my husband entrance. I went into full blown labor, the midwife came to the house to check me, found no heartbeat, called EMS, and my son was born within 5 mins of her arrival. It was a brutally hard birth. The hardest thing I have ever done, the most intense pushing. He was perfect, but blue, she and my husband did cpr until the EMS arrived, they continued to the hospital. The coroner confirmed death had occured about 24 hrs before – just as I had suspected. Now, three weeks later, I am healing well – with just pelvis and hip pain (I didn’t tear, even though he was 7 1/2 pounds). Mentally, I am strong, I am a realist and I understand that life and death are part of life. I miss by precious, beautiful boy. But I am well. The autopsy report (full scheudle of bloodwork done as well) showed no infection, no deformities, he was 100% healthy, not wrapped in the cord, all organs were healthy, no infection: my bloodwork was the same – normal. The placenta was whole and healthy. So what went wrong? Nothing, there are no answers, but I didn’t order the autopsy report to find out why he died. I ordered it to find out that nothing was wrong, this helps me be strong for future pregnancies. The Covid19 pandemic has seen a rise in stillbirths, the majority have been undeterminable as to why. Now, I don’t smoke, I don’t drink, I wasn’t around anyone with covid. I have been healthy during pregnancy and post pregnancy. So, what went wrong. I am going to suggest that stress may have played a bigger role that most people would imagine. My province shut down banning “non-essentials” just 2 weeks before his due date. I rushed out to buy what I could before the stores closed. I was afraid to give birth in the hospital because I REFUSE to be alone. I advocate for myself and due to a past trauma with an unscrupulus male doctor, I ALWAYS take my husband with me, as a witness. The hospitals are robbing women of their rights, they are forcing them to choose between their safety and their comfort. This stress, this fear is taking a huge toll. And afterwards – isolation – unless you break the rules. Which I have, and do, and plan to from now on. I refuse to be shut away with my grief, I refuse to be denied a hug, personal comfort, etc. Why? Because covid isn’t a danger? No, because while covid patients matter – so do I . So do we. Everyone matters, and if politicians and health professionals had truly believe that, I am sure there would have been less suffering. Stillbirths are on the rise, because we are scared to go near the hospitals. This is an utter shame, and a travesty, one that could have been avoided.
Dear Ashley,
I am so terribly sorry for the death of your precious son, just mere weeks ago. Your bravery in sharing your story shines out. My son Wilder died just 11 days before he was due, and was crazy active throughout my ‘perfect’ pregnancy, and after he was stillborn, we did every test we could including autopsy, and found absolutely nothing wrong with him. It is what literally drives me to do the work that I do, to this day. Covid has made everything worse, and the lack of human contact has been so very hard to bear, and you are right that it seems clear that stillbirths are increasing with Covid for many reasons including the ones you point out. I wish you every strength in the coming weeks and months,
Susannah
Hi I’m Kristy from Australia. 8 months pregnant & on Monday the 15th March 2021 I couldn’t feel any movements from our little girl so I went to the hospital and I was told there was no heartbeat. She was so active and I thought everything was fine I just didnt want to believe it, I never thought this would happen to me I was in shock and I knew I had to give birth to her. I wanted a c section but they said it was to risky for me and this was the safest way, the cruelest way ever.
Last Thursday 18th March 2021 at 12:15am I gave birth to my little girl Amirah weighing 4 pounds she was so beautiful and I could see my almost 4 yr old son Lachlan, they were so much alike. I really wanted to give him a little
sister, he kept saying to me all the time when is baby sister coming. Breaks me heart.
This last wk has been the worst time of my life I feel so empty and just want answers to what happened. I keep going over and over the days before I couldn’t feel any movements what if it was something I ate or something I did because it was all going so well up until then.
My husband and I tried 8 yrs to fall pregnant and nothing until we decided to go through ivf which Is how we had our son Lachlan, it worked first go and we were so happy then we decided to use the frozen embryo and the whole pregnancy was great all was well she was moving so much more then my last pregnancy so I just thought everything was fine.
I feel like my heart has been ripped out I miss her so much and leaving her at the hospital was the hardest thing I’ve ever had to do.
Everything I see or things around me remind me of her and when anyone talks about it I break down, I want to be strong for my little boy but it’s hard to cope. I know he senses something is wrong and I don’t want to upset him but I can’t control my emotions I just feel so lost and wish I had my Amirah with me.
Dear Kristy,
My heart aches for you. I am so very sorry for the devastating death of your beloved daughter Amirah. I remember feeling those feelings. For me, in the first days and weeks after Wilder’s death, I sought soothing in actions related to Wilder–planning and holding a small ceremony to scatter his ashes with family and friends, composing and sending out a birth/death announcement to friends and family, creating an album of photos and keepsakes, buying and reading books about stillbirth, meeting with a perinatologist to review what had happened, etc. These actions were helpful for me in bringing me forward in time each day. In Australia there are many excellent resources and organizations to help families whose babies were stillborn. These include https://rednose.org.au/, https://stillbirthfoundation.org.au/, and https://www.bearsofhope.org.au/ and you can also find more resources at https://www.stillbirthcre.org.au/ It was also a great comfort to me to find people to talk to who understood.
I am so sorry for what has happened and send you strength,
Susannah
I just lost my twins 3 weeks back. I was 25 weeks. One was still alive at the time I went to the hospital but had passed on the time he was out. I kept on hoping that he could still have been saved!. We had been in and out of hospital due to placenta previa but all the tests and scans showed that all was okay. All I needed to do was to be on bed rest which I did. It was hard to tell that there were no kicks from the other twin since one of them was still moving. I only got to know that one the baby’s heart had stopped after the scan and there was no water in his sac. Again the doctor informed us that he had passed on 3 days back after removing the stitch. I feel a lot of pain, I hurt every single day, I just realized that however much someone may have gone through a similar experience, the pain is always different. My babies were physically fully grown. I have never understood why the live twin couldn’t be saved!. It just hurts.
Can you bring your counseling services to Uganda too. I surely need someone to talk too.
Dear Monica,
My heart goes out to you. I am so terribly sorry for the death of your precious twins. I can hear how your heart aches. My group at the International Stillbirth Alliance (www.stillbirthalliance.org) is just completing a Registry of all stillbirth parent support organizations in the world, but it is not yet online (soon though). I checked our information and found 1 organization located in Uganda, Hope for Woman in Crisis, that you could try, although it looks like this is only accessible via Facebook. HOWEVER, a dear friend and colleague from the US works with a team of nurses in Uganda on stillbirth care, and she would be happy to connect with you directly. Please let us know via a comment whether you would like this, and our blog managers can help to arrange it. Also, there are other resources you can access. If you have access to Facebook, search for First Candle Stillbirth Support where moms connect directly, or visit the website of my dear friend Wanjiru’s stillbirth support organization based in Kenya, Still A Mum (https://stillamum.com/). You are not alone.
Peace,
Susannah
Hi Monica,
I recently lost my twin boys at 21 weeks (3 weeks today). So I can relate to your story and pain.
We had been using fertility medication so I am terrified that I will not get pregnant again.
Unlike you I can’t talk to anyone. I haven’t spoken to any friends, family and have been trying to block out the experience from my brain.
I desperately want to be pregnant again and trust my body but I also feel like I want to give up and accept that I am not to meant to be a mum.
Only being 21 weeks also makes it a difficult experience to process in comparison to women who went full term. It’s been hard to find stories of second trimester loss…lots of my friends have babies/are pregnant so that also makes it very difficult and I feel like lots of my relationships will change.
Wishing you all the best all the way from NZ xxx
Hi Sarah,
I lost my baby at 25 weeks on May 9 2022. I finally felt I was in the safe zone. Recovering from this has been absolutely brutal. 2nd trimester loss does seem less common and all I can think about is the fear this will happen at full term. X
Hello Sarah. I also just lost my little rainbow ruel rose at 30weeks but I was counting 34weeks .the doctors said she had growth restriction or maybe she was just too small for her gestational age .i woke up on the 25th of August 2022 expecting to feel her morning kicks but felt nothing waited a hour and felt nothing went to hospital ,midwife checked with a doppler and heard no heart be at there after it was a race to my hospital to see my OB , went for a scan and there was a heartbeat. The relief .but the water in the sac was was sufficient was admitted for a c section in 2 days but the next morning when the midwives cane to do their morning checks there was no heartbeat again. The agony the grief my heart sunk had another scan and this time there was no heartbeat I was induced and I pushed my little gal not breathing .with tears in my eyes .we still don’t know the cause of death except she also had a cord wrapped once around her neck . so wondering if anyone out there also had growth deviations but am so glad such a forum exits to share and help each other.
Dear Rebecca,
I’m so very sorry to know of your daughter’s death. It was so very recent. I can hear your pain through your words and I can hardly imagine the agony of the way it happened. I am also very glad that you found this place to share your experience and perhaps find some comfort. My organization, the International Stillbirth Alliance, is working to build a more permanent place for a parent support network. I hope to share that news as we move forward. When Wilder had just died, I found it to be enormously helpful to talk with and write to other mothers who experienced what I had–unexplained sudden death. It can really help to talk to other moms. I hope that you find this. Sending strength,
Susannah
Editor’s note: received from Susannah to post on her behalf.
I’m very sorry for the loss you suffered.
I hope my questions and comment aren’t deemed inappropriate. My experience is from the other end of the spectrum. I am a Rainbow baby, conceived approximately two months after my brother was stillborn at 20 weeks. Recently a flood of emotions have overwhelmed me about my brother and my conception even though I am in my fifties. If my brother would have developed to full term I wouldn’t be. It isn’t lost on me that my sibling died making way for my conception and birth and the sadness I’ve recently felt over it all is profound. I feel fate played a cruel trick on us because even if he lived we could never have known each other. We were destined to forever to be separated.
My question is do you know of any literature or support groups for people conceived in the timespan of their stillborn siblings due date? I think a certain amount of feelings comes with being a Rainbow baby in general, but in my experience knowing my brother’s death opened up the doorway for my life is incredibly hard. I appreciate any information you can give me.
Thank you.
Dear Betty,
Thank you so very much for your courage in sharing your story and your strong and complex emotions, and my deepest condolences on the loss of your older brother. My eldest living son was also conceived in this time period, about 3 months after the stillbirth of his elder brother Wilder, and I think often of the conundrum you describe–had my Wilder been born living, none of my three subsequent precious and beloved children would have been. After two decades of considering this situation, I have concluded it is unresolvable. Do I wish Wilder had survived? Of course I do. Do I love and protect my three living sons with all my heart and soul? Of course I do. These are unresolvable and they make me realize anew that life is just really complicated. I also consider the fact that my studies and my career, as a global stillbirth advocate and perinatal epidemiologist, would never have been, if Wilder had survived. Do I love my work with great passion? Yes. Would I rather have had Wilder survive and I had never found this passion? Yes. These again are unresolvable. I share all this just to try to express that I can glimpse your travails. I do not know of any support groups for people in your particular situation. However, I am thinking of several groups that do provide support for parents of “rainbow babies”, and these may be a starting point for you: Tommy’s in the UK (https://www.tommys.org/pregnancy-information/help-and-support), SANDS in the UK (https://www.sands.org.uk/support-you), Star Legacy in the US (https://starlegacyfoundation.org/), and Share in the US (http://nationalshare.org/). You really raise visibility on this nearly invisible group who also are part of the burden of stillbirth. I thank you for this.
In closing I would just offer the thought that it is possible, as I personally know, to deeply love individuals whose mutual existence is literally impossible–in my case, Wilder, and my other three sons. Courage to you,
Susannah
Susan,
Thank you so much for sharing your story and shedding some light on the very real problem that has been plaguing women and families for years. Even at this point in our society, pregnancy loss is still not supported adequately and women and families are left feeling isolated and empty. Almost a month ago my husband and I had our dreams and our hearts shattered. After being told by our fertility doctors that we couldn’t get pregnant on our own, we got our miracle baby girl. We thought for sure that it was for a reason and that everything would be okay. At every check up I’d sit there(by myself because of Covid) holding my breath bracing myself for bad news. But my first trimester passed and the baby continued to progress, the 20 week scan passed and we were told she was perfect. No complications just that she was a little small but doctors and the specialists weren’t concerned, we were told “she’s proportional and you aren’t big, so you won’t have big babies”. We left that day feeling elated and finally able to let our guard down that everything would be okay. I continued to plan as I had been doing for weeks, planning her nursery and everything that a new mom is supposed to do. A week after the check up I started to feel like something wasn’t right, I couldn’t feel her move as much, I wasn’t ever sure if it was her or just my stomach gurgling. But every time I’d bring up the concern, I was told to relax and not to worry, that every baby is different. Despite feeling that something wasn’t right, I didn’t want to call the midwifes to ask them given that I was afraid of being viewed as paranoid, and I wanted to continue to be optimistic and hopeful. At my 24 week check up, I went in feeling confident and that she was okay. At first they couldn’t find her heartbeat with the doppler, but I still wasn’t worried. It wasn’t until I saw it for myself on the screen that I knew my gut feeling had been right. Something wasn’t right. When I heard the words “I’m sorry there’s no heartbeat” I could hardly believe this was real. Everything from then on moved so fast, I delivered her the next morning on 11/6/2020. Of all the hard parts of this journey, one of the most difficult parts is not knowing the “why”. Doctors have no explanation, no reason, and we’re just left with more anxiety and wondering what happened and how we can ever expect to trust medicine and doctors when they tell us everything is fine. The grief feels so deep and like it can consume us and all I want right now, is to have my baby back, to be part of the “pregnancy club” and to be the happy slightly naive person who thought everything would be okay and that I would get my “happily ever after”. But I know that I won’t ever be the same, every day I wake up I’m reminded that my life has changed, and that I’m a mother of child but I’m left with empty arms.
Now I start again the conception journey and hoping and praying I won’t have to turn to fertility treatments and that by some miracle, I own’t have to endure a loss of this magnitude again.
Once again, thanks for sharing your story, helps those of us who are going through the grief journey to not feel so alone and isolated.
Dear Sujai,
Thank you so much for your generosity and courage for sharing your story of the loss of your beloved daughter, just one month ago, so very fresh. I really relate to that worry of ‘bothering’ the doctors and nurses with our concerns, that is how I felt that final morning before knowing, when I realized I couldn’t feel our baby move but was worried to ‘bother’ our midwife–as if that was not in her job description! I just felt so kind of small and uninformed and shy to speak out. Not any more!!! I also so relate to your agony over not knowing…wondering how ever to trust that ‘it will be ok’ when we know that sometimes it is not ok. For me, it was a fundamental shift in my world view. I don’t even really remember how I used to be; ever since Wilder died, I think I’ve been much more cautious and alert. I know from my own experience that hearing the stories of others who have had to endure this crazy grief can help; somehow it helped me a little bit, knowing I was not alone, and I am glad that it helps you a little bit too.
Wishing you strength and courage,
Susannah
Hello, I just had my first child a week ago and she was stillborn at 23 weeks. I am devastated. The amount of decisions we had to make in such a short time frame was overwhelming. However. I am glad I decided to labor and deliver to see her and hold her. I was so scared I wanted to have the D&C and be out to sleep but my husband encouraged me to not be afraid of pain. I was well cared for by him and the medical staff. The entire experience seems like a blur now a week later and I struggle daily. Because of covid 19 my pregnancy had been very isolated and still continues to be. I am slowly working on myself and not expecting too much from myself while I process this tragic loss. This was my first pregnancy ever and a long awaited one. My husband and I have been together for nearly 10 years. Any advice on how to process this grief and when to try again? Thank you.
Dear Susan, I am so terribly sorry for the death of your daughter, just a week ago. There are no words at all, even though we all attempt to find ‘the right words’. I can only say that I keenly feel your devastation and remember how I felt in those first numbing weeks. I am so glad that your partner and caregivers have provided you with helpful support. Each person is different in what helps them to move forward in time. For me, reading everything I could get my hands on about stillbirth was very helpful, though I’m not sure why. I also found another mom whose daughter Emily was stillborn just a month before my son Wilder, and the two of us were very close for the first couple of years (though we have only met in person once, and that was years later!). So finding others to talk to was very helpful. I also did a lot to keep Wilder’s memory green, including sending out a birth/death announcement to many people, holding remembrance ceremonies for him, and creating an album of cards and other memories related to his short life. There are also many support organizations out there, depending on where you live, that provide places to share experiences and grief, including through virtual support groups. Some of these are listed just below the blog above. In terms of trying again, again this is extremely personal. Aside from discussing with your doctor in case there are medical concerns to account for, it’s just whatever feels right to you and your partner. Some people feel it is best to wait for quite a while. I tried again as soon as I could, and that was right for me. You are in the throes of the shock and grief right now, and I send all best wishes for courage and strength,
Susannah
I’m am so sorry for your loss. Thank you for sharing your story and creating a forum for us parents to talk about our beautiful angel babies. You are an inspiration and have certainly helped me during this difficult time.
Dear Sophie,
Thank you so much for your kind and generous words which really warm my heart. I really feel the warmth of sharing our stories–which is terribly ironic since they are so desperately sad–yet for sure, sharing what we have all endured in some way truly does help-
Susannah
Thank you for your story, It makes me feel a little more sane knowing someone else went through this as well. On July 14,2020 we lost our son Maverick John at 36 weeks and 3 days pregnant. I went into labor the night before and did not know he had passed until we got to the hospital. I was 9cm dilated when we got to the hospital and they got out the doppler to check for the heartbeat. The nurse couldn’t find it so she got a doctor and an ultrasound machine and the doctor said “Im so sorry it’s what we thought, no heartbeat”. Maverick was born less then an hour after we got to the hospital weighing 5 pounds and 15 oz. When I held him, I felt relief and joy and then the sadness hit me. We have just recently started to feel normal again but understand that there will always be a hole in our hearts, something within me was taken that day. We just recently found out I am pregnant again (I am 7 weeks now) and am actually due on Mavericks birthday. Any advice on how to get through a second pregnancy? Thank you!
Dear Hannah,
I am so sorry for the death of your beloved son Maverick John four months ago. Thank you so much for posting. I can hear the words of your doctor telling you there was no heartbeat. Even though it is 21 years later, I still can hear the calm words of the technician telling me the same thing about Wilder’s heart. Your new pregnancy is about the same spacing as my second pregnancy was–I got pregnant about four months after Wilder died, pretty much as soon as I could. What an irony that your due date is Maverick’s birthday. For me, I managed to get through my second pregnancy very methodically. I felt cynical about all the care I had taken with my first pregnancy, since that seemed to be a complete waste, but I knew that I had to maintain the same care for the sake of my new baby anyway, so I just did. I decided to go back to the same hospital to give birth, because despite the death of my baby, I really felt very cared for there. I really wanted my bereavement nurse, Patty, to be with me for my next delivery, and she was, and that was absolutely critical for me. I asked to be delivered early via induction at around 38 weeks because I felt that I could not bear to deal with passing the 38 1/2 week mark when Wilder had died. However, I was unaware at the time that there is a substantial risk of problems when a baby is induced early–for instance, the baby’s lungs may be immature and this may cause problems for the baby’s survival and future health, if it is delivered early. My doctors agreed to the early induction (which was still technically full-term), but I wish they had discussed the risks with me, as I might not have decided to go with induction if I had realized this. So, I want to strongly underline that I recommend discussing risks and benefits of all delivery options with a doctor whom you trust and feel comfortable with. I also asked for extra monitoring of my pregnancy. My doctor somewhat reluctantly agreed, just to make me more comfortable. Now we know that under some conditions, a prior stillbirth can increase the risk of a subsequent stillbirth, and so it is really important again that you have a doctor you feel comfortable with to care for you during this pregnancy. I also had a really special friend, Lisa, whose daughter Emily was stillborn a month before Wilder was stillborn, and we helped each other through our subsequent pregnancies. Just emailing each other was incredibly important.
Wishing you strength and courage,
Susannah
Hello ma’am!
I am Richa from Jodhpur, India. I recently had to endure the grief of stillbirth on 7th November 2020. Me and my husband were never prepared for this. All the scans were well till 16 October and yet on 6th November I was informed of my child’s death. The doctors don’t know when or why my baby passed away. All my reports are normal.
Ma’am what I feel unsure and guilty about is why I couldn’t asses there were less kicks. I felt some kind of movement for sure coz me and my husband discussed that daily but my doctor attributes that to just baby floating in water and not kicks.
I feel if I had understood kicks better… I could have saved my child…. maybe…
This was my first pregnancy and there were some family problems around and so no one guided me about kicks… I do feel guilty towards my husband .. Everyday he asked me if his baby was fine and I replied …yes.. even after the baby passed.
Dear Richa,
I am so terribly sorry for the death of your baby. Your story is so familiar to me. My husband Craig and I were utterly unprepared for the death of our son Wilder. Everything was perfect–until it wasn’t. All my scans and other antenatal care were all completely normal, just like yours. I don’t know exactly what day Wilder died… I think it was probably Saturday, the day before I found out that he died. But it could have been earlier. I will never know. I too felt agonized over wondering what I could have done differently to prevent Wilder’s death. I remember sitting and waiting to “count the kicks” that Sunday morning, kicks that never came. But Richa, I want to share with you the really important fact that there is no fixed number of movements (e.g. 10 per hour), NOR is there a fixed type of movement (e.g. a ‘kick’) that magically means everything is well. Rather, exactly what you did–being aware of your baby every day–is exactly what is important in assessing your baby’s wellness. One excellent resource for information about this is at the Stillbirth Centre of Research Excellence in Queensland, Australia (https://www.stillbirthcre.org.au/). Richa, I also want to share that it can be so hard after our babies die to relate to our partners. We were the ones who carried our babies and sometimes the feelings after our babies die can be extremely different between the mother and the father or other partner. Craig and I have had some hard times over the years when we grieved differently for Wilder but we have managed through those times, trying to keep the lines of communication open between us, and sometimes seeking help from a counselor. Richa, guilt is such an excruciating feeling. As mothers, I think we must be patient and kind towards ourselves. We did the very very best that we could for our babies. It is so hard to live with their loss. I wish you strength and courage in the days and weeks ahead,
Susannah
Thanks ma’am for the guidance. I did visit the Australian site that you mentioned ans it was indeed helpful.
Since I am in India and there are no local support groups , I wanted to know if there are any online support groups like yours where I could chat and interact and share my questions and concerns.
Dear Richa,
It is good to hear that the Australian site was helpful! My group, the International Stillbirth Alliance (ISA), is very aware that there are currently no local support groups in India for stillbirth mothers (and others). In fact, we are currently implementing the Parent Voices Initiative (PVI) with 2 projects to help with this situation, in India and globally. One of the projects is a ‘registry’ of all parent support organizations in every country in the world. So far, we have found over 500! And in countries such as India, where we know there are no formal support organizations, we are gathering links to informal support organizations (eg Facebook groups) and identifying ‘point persons’, people who aren’t associated with organizations but still can help to identify support for bereaved parents. We will be finishing and publishing our Registry on the ISA website hopefully in January. The other project we are doing is in India and Kenya, to create toolkits to support clinicians and parents to talk about stillbirth. In India, we are partnering with friends at the Postgraduate Institute of Medical Education and Research in Chandigarh. Also, at ISA we are right now discussing how to provide some modality for people to talk together about stillbirth and newborn death–not only parents but also other groups of people, for instance researchers–and maybe to provide different spaces for people to talk together in their own languages, or groups of people from the same geographic region. Sorry to write so much, but your question is so important and it is one that we at ISA really want to have a good answer for… For now, you can email ISA directly at info@stillbirthalliance.org (that way we will get your email address and can connect with you directly rather than through this comment board). When you email, we can connect you with any resources we may have found in India as well as online groups that are not dependent on where you live.
Warm regards,
Susannah
May God help us get through this
After losing a baby ,it won’t be the same again.
Dear Faith,
Sending you strength and courage to move forward. It is so hard, but you are not alone. Thank you for posting.
Sincerely,
Susannah
Hi Susannah,
I am so sorry for your loss. Thank you for so sharing your story,it will somewhat help me to come out of my grief which I am currently going through.
I am Saloni ,I live in Netherlands ,I had a tragic incident in my life with that I am totally broken now.
In Jan 2020 I got pregnant so was thinking myself fortunate.As this was the corona time so I was working from home for the whole pregnancy tenure so was bit relaxed. We both were very cautious and we didn’t disclosed the news to anyone before the first trimester is finished except our family as we heard that if we pass the first trimester the rest of the pregnancy is quite safe. So we were bit relaxed after that.
Everything was going very fine all my echos and tests were good but again we were scared before going to every echo but our midwife used to say everything looks perfect to her that was a great relief for us ,as our child was doing good.
After my 20th week scan we got to know that we are having a girl so we both were super excited for her and started planning things for her. There was a fun echo planned that we requested in 26th week on 22nd July 2020 so we went to our midwife ,during the echo midwife noticed a heart rate dip of a baby so she immediately asked us to go to hospital for heart rate registration we both rushed to the hospital unaware what is happening. The heart rate for me and baby was monitored for 1 hr and also they did the echo they still found the dip and referred us to a big hospital and told us there can be chances that we might need to go for C section we both were surprise to hear that what had happened immediately everything was fine ,she was healthy and now C section but we had no other choice just to believe and follow what the doctors were saying .
I was admitted in this new hospital for one day on 22nd july and again registration and echos were made everything was fine next day and doctor’s words were”Thank God we didn’t took this baby out” and we were asked to go home and they gave us assurance that everything is fine now and case is transferred back to mid wife ,we both were so happy and thanking god.
Then after a week on 30th July I had the appointment with my midwife, she did the echo and we saw the heart was pumping and could also hear but one thing which we both noticed which haven’t noticed before that she was not moving as before she used to be super active always, we were surprise to see her like that so we asked the mid wife so she told she might be sleeping so we got relaxed,also in the night I felt her movement.
Next day on 31st July since morning as I got up I was not feeling her movement but I waited for a day as we just had the scan the previous day but for the whole day I didn’t felt her movement did all I used to do to feel her kick but nothing happened.
On 1st Aug,in the morning I told my husband I still cant feel her movement I am calling the midwife,so she came in 30 mins at our place ,she measured the heartbeat with the small instrument and felt the heartbeat and she told its a protocol to go to the hospital to be sure so my husband said that we will surely go to the hospital ,so we went to the hospital thinking everything is fine as she just checked we are just following the protocol. We reached the hospital and again heartbeat registration was done for 1 hr after an hour nurse came and told there is something wrong as we are not sure this my heartbeat or baby’s so we need to do the echo to find where is she. So they did the scan and saw baby was not moving and also there is no heartbeat we were told by the doctor at first we both were not ready to believe what she was saying and asked her to do the echo again but she confirmed and said ”she is no more”
We both lost our senses and my husband called our friends as our family were in India to the hospital everyone was in shock, we were asked to go home and to come back after 48hrs and I was given a medicine to prepare my body for the delivery. For 2 nights I was having my baby with me but dead ,I was totally not in senses with no emotions
On 3rd August we went to the hospital and doctors wanted to do normal delivery so they induced pain and also provided me epidural so that I could get some relief from the physical pain and they were checking after every 6 hrs the dilation which was not increasing much so they induced the medicines 4 times till 4th August finally at 20:21 our daughter MEHER (the name we gave to her) was born . I had to go for a small surgery for placenta removal and lost so much blood and after I came back from the surgery nurse asked us to say final goodbye to her ,so we both took Meher in our arms and talked to her , she was so beautiful and every body organs were fully developed , she had same black hairs like me..
After 2 days our family came from India for the funeral of their grand daughter Meher which was planed for 10th August as we wanted to bid a goodbye to her in a proper way and also her soul should rest in peace. This was most difficult moment for us as we never thought that we will be doing all this ,burring a child is a worst thing that any parents need to do.
Doctors are still investigating what might have happened with the MRI etc but till now the only reason they gave was that umbilical cord was around her neck 3 times and tightly untangled so they think this might be the reason of death.
I am not sure whether we will get the answers to all our questions that are in our mind right now , why this happened ,why again but one thing for sure I know I think having a baby soon is the only healer for me, not sure if that can be possible anytime soon”
Dear Saloni,
Thank you so much for sharing your story of your beloved daughter Meher. My mind is with you as I read about the moments before, during and after your finding out that your daughter had died. The numb days of waiting before you delivered her, and the urge to have another child quickly, the bewilderment at “why”. I am so sorry for your loss. I am glad that your family was able to come and be with you to say farewell to Meher. It has now been just over a month since she was stillborn. Those early days, I remember well. They are dreadfully harsh. I too was desperate to get pregnant again and to have another child, a living child. Due to health issues I had to wait three months before trying again, and it was so hard; that time felt like an eternity. I was lucky that once we did start trying, I fell pregnant again very quickly. But the second pregnancy was utterly different from the first, realizing truly what could happen. My eldest living son, Zimri, is now a sophomore in college… yet none of us forget Wilder, ever. Thank you for sharing your daughter Meher’s memory with this community. I try to help keep green the memories of the babies who are stillborn so that the world remembers them. Strength and courage to you in these hard, hard days,
Susannah
Hi Susanna
Its sad to loose pregnancies and babies because all we have hope to meet with our precious babies after all those months.. but lets all have hope God have purpose for that. Its past 5wks and days now l lost my baby l was full term(40+6) l can say because of negligence of nurses if they had listene to me l hope they could save my baby. It all started a night friday when I was feeling labour pains till the whole day of Saturday bcoz l was told to wait till l see water or blood before I go to hospital so l was waited till sunday 2am then l decided to go to hospital bcoz the pains was too much so went there with my husband bcoz of this covid-19 they couldn’t allow my hubby to get inside. So when they checked me they said l am 2cm l hv to wait l waited there the whole day of Sunday till 8pm they checked me again said l am still 2cm and l asked them to take me to theatre bcoz my fist child l gave birth thru csection and they refused said the theater is closed so l was kept going to them asking to help me but no one attended me.. till 3am on Monday one sister came and check me she said now ur 5cm then let’s go to labor room l said what l wanted is to go to theatre she said no let’s go to labor room and then she said now is 3am by 5am will delivery ur baby and something to 5 l feel was coming and l called her she came and she said now ur 9cm u can start pushing l push push nothing came out and my baby she was very active and strong she was pushing herself also but nothing and that nurse said sis u have to wait 1hour again l said no take me to theatre she said no wait and she left l was there all alone so something to 6 l started feeling something happened in my stomach l call her several times she couldn’t come she came the time she want that time my baby starts going back to my tummy and she said now we can go to theatre and we went there so what l saw in that theatre is only changing my mask and one was wiped my handy thats all till afternoon 01h30 when l wake up l saw my husband and doctors they said u had a baby but she passed away..can u margin this l wasn’t believe that still now am still shocked it happens on 15june2020. So to loose a baby hmm is so much painful😭😭😭
Dear Cecilia,
I am devastated to hear your tragic story of the loss of your precious daughter. You tried so hard to protect her. I am also so very sorry your husband was not allowed to be with you due to Covid-19. Of course you are still in shock. It is a terrible shock and grief to learn that our babies have died. I wish you strength and courage to continue through these early painful days. You are not alone.
Warmly,
Susannah
Hi Susannah,
My first baby, George, was born dead at full term (39 weeks and 2 day days) on June 2, 2020. Six weeks into this grief journey, I find myself searching the internet looking for stories to relate to, both in an effort to not feel so lonely, and also for reassurance that I will be able to feel joy again. Your story and the work you do is inspiring, and I appreciated your heartfelt responses to everyone’s tragic stories here. Mine is a similar tragic tale. After a perfectly low-risk, uncomplicated pregnancy, I woke up on June 1st (my first day of my maternity leave) and didn’t feel George move which was unusual. I didn’t panic. I waited. I made a smoothie. I had a shower. But after an hour, I announced to my husband that I was going in, just to be sure. He didn’t come with me. When I arrived, multiple midwives tried to find a heartbeat, and I was ultimately told George had died. I’ll never forget the eyes of the midwives – all wearing masks because of coronavirus. I knew what they were going to say before they even said it. I was alone with three masked strangers and was just told my baby had died. No one can hug or comfort you. I just sat there, crying and asking if they were sure. It was the worst day of my life. I was induced and gave birth to him the following afternoon. I got to spend some time with him. He was perfect in every possible way. He had dark hair and my nose. He looked like me. I’m still trying to process what’s happened. I fluctuate between overwhelming sadness and seething rage. I’m 36 and worried that I’ve left it too long and that I won’t be able to get pregnant again. I worry that even if I do, I’ll be so overcome with worry and anxiety I won’t make it through 9 months. I’m trying to remain hopeful that the future won’t be so dark, and this post has given me a bit of hope. Thank you.
Dear Miranda,
Ohhhhh…. I have been there…. I feel your agony. I am so sorry George has died. Continue forward in time, is the only advice that I can give. I was 35 when Wilder was born, and I went on to have my three living sons when I was 36, 37, and 39 years old. I was also afraid for all these subsequent pregnancies and to this day, 21 years later, I still fear unreasonably for my kids. It is just one of the many ways that Wilder changed me irrevocably. George sounds beautiful. It’s desperately sad. Continue forward, find people who are in our ‘club’ to talk to and tell the story of George. Heartfelt wishes to you in this crushing time.
Miranda, I’m so sorry you didn’t get to take your sweet George home. I too had an uncomplicated pregnancy/low risk. I am 37 and this was my second child (my oldest is 7). My baby girl was a week overdue just like her big sister. I had an appointment on a Monday where they gave me a stretch to induce labour and her little heart rate was a strong 139. I had a routine 41 week ultrasound scheduled for the following day since the Monday was actually a holiday and the diagnostics office was closed. I had felt her moving that night and also went into labour, but by morning my labour had kind of petered out. I called the midwife and she told me to go to the ultrasound appointment. We packed the hospital bags before we hopped in the car. My husband was so excited. Because of Covid he had to wait in the car so he decided to catch a nap, after being up all night with me and expecting more sleepless nights to come. I went into a tiny small town hospital – one I’d never been in before, but I had met the tech many times over my pregnancy. She turned on the machine and all seemed normal except she held the Doppler my stomach very still for longer than normal. Then she told me she had to send off a report, asked if I was fine, then quickly left the room. Instantly I knew something was wrong. I went looking for her and couldn’t find her. I started to panic. I tried to nudge the baby to move and nothing. As she came back I started yelling at her telling me to tell me my baby was ok. She told me she couldn’t tell me anything and then the phone rang. It was my midwife calling. I was in shock. At that point the tech had run outside to get my husband. He thought I was having the baby. Pure devastation. I don’t know another word. We had to drive to a hospital that was an hour away. My midwife hugged me. She didn’t care. I was induced and had my sweet girl Leah the next morning. Perfection. And the autopsy report confirmed that she had nothing wrong. I had a blood clot in the umbilical cord and some in the placenta but they could not confirm if this was the cause. We also were able to spend a few hours with her and have photos done through a hospital program. The last thing I remember with Leah was kissing her all over her face knowing I would never be able to kiss her again. Almost harder than having me daughter stillborn was telling my daughter who was expecting to be a big sister. This happened on May 20, 2020. I’m still struggling, and about to start counselling. I worry that I waited too long to give my child a sibling. We want that for her and for us so desperately. My husband and daughter are doing well. We all have moments we cry and are sad, but we are also a family who believes in God. Our faith and faith family have been the only thing that has helped us keep going. But as we try for another – we tried as soon as they said it was ok – every month is devastating when I know yet again I’m not pregnant. I have many more days that are good than bad after almost 6 months. My hormones are the one thing that sends me spiralling. Also my brother and his wife are due any day. It’s so hard to see babies. To constantly want to know why mine was taken. Why my daughter and husband have to be hurt like this. Please feel free to reach out to me Miranda. I would be glad to talk to you any time. You are going to be okay. And I know it doesn’t feel like that at all. But you will be ok. I pray for both of us that we will be able to dull the hurt with healthy living babies in our arms again. I too found this post has given me hope.
Dear Heather,
So very much of what you wrote, I can truly say I imagine it, because it happened to me too. Even after nearly 22 years it is all still right there. The perfect wanted pregnancy and the devastation and shock, and then never knowing…the desperate desire to be pregnant again, and the waiting and uncertainty. I am so sorry for your loss of your dear daughter Leah. The only thing I know is that the forward progress of time was ultimately sustaining for me…and the fellowship of other moms who were forced into this ‘club’, along with very dear allies in the many clinicians who, though they have not personally experienced stillbirth through their own losses, have experienced caring for those who have, and who work so hard to support us as they have to also manage through their own emotional responses to our losses. I have somehow found my way through meaningful work that keeps Wilder’s memory green, and I have also been so very lucky to have my family and friends supporting me. Stay safe and take heart,
Susannah
I’m really sorry for the loss of your daughter Leah, Heather. Thank you for offering to connect with Miranda. If Miranda would like to do this, it could be done by each of you emailing us at feedback@evidentlycochrane.net and we could put you in touch.
Very best wishes,
Sarah Chapman [Editor]
Dear Miranda, I am so sorry for the loss of your son George. You’ll see another bereaved mum, Heather, has replied to you and offered to connect with you. If you’d like to do this, if you both email us feedback@evidentlycochrane.net we could put you in touch with each other.
Very best wishes,
Sarah Chapman [Editor]
Today Wilder would have turned 21 years old. The grief is immediately accessible even after all these years. One of the only places I want to be today is on this site. I am again beyond grateful for my dear friend Aleena who, through her research and this blog post, gave life to a rare new green shoot of Wilder’s own life; and grateful to our compassionate hosts behind the scenes (Sarah), and to all of you, who green the memories of your own children through what you read and write here. I so wish I were not a member of this club, yet it sustains me.
Dear Susannah, I’m sorry not to have seen your comment yesterday and to have sent this message then, but wishing you much strength and comfort at this painful time. We are so grateful to you for having turned this space into one which provides much needed comfort to many women. Selena (Evidently Cochrane).
Dear Susannah, I’ve been on leave and have just seen this. I just want to echo Selena’s reply, for we are so grateful for the work you, Aleena and colleagues do, and that you have shared yours and Wilder’s story here. We are so moved by the experiences you and all the other women have shared here – we think about each one and hold them and their babies in our thoughts. We are really thankful that this is a space where people who have been through, and live with, the pain of stillbirth are finding each other and finding some support, comfort and hope. Thank you. Sarah (Evidently Cochrane)
Susannah,
Thank you for your vulnerability in sharing the raw emotion and details of your loss. I can relate to so much of your tragic experience having just lost my son. He was stillborn at 36 weeks following a problem-free pregnancy that posed no concerns whatsoever. I find myself here 6 weeks pregnant after 6 months of trying to conceive and although I knew we were in for a bumpy ride through a subsequent pregnancy, I was not prepared for just how much anxiety and fear would cripple me. With no answers as to why or how our son’s heart just stopped beating, I am wondering if you have any advice on testing/scans/extra care as I navigate through this pregnancy with fear gripping every ounce of my being. Is there any specific care we should request that you think would be helpful to us through this pregnancy? Any resources you could point us towards or recommend? I sure appreciate the work you have devoted yourself to.
Brooke,
I am so sorry for the loss of your son. So much of your story is similar to my own. The subsequent pregnancies are so hard. I always say that no one can ever tell me again “Don’t worry” because I know that the worst can and does happen. In terms of advice, critical is to find a prenatal midwife/nurse/doctor who takes all of your issues and concerns very seriously. Medically, given the lack of knowledge of the cause(s) of your first child’s stillbirth, there is only additional monitoring to be done (since prior stillbirth is a risk factor for its recurrence). However, many stillbirth moms including me ask for more. For instance, I insisted on being tested for Group B strep with my subsequent pregnancies (this may now be standard though). I also asked to be induced at 38 weeks as I couldn’t bear to go longer. This is quite controversial though, as induction brings its own significant risks (which were not explained to me at the time…). There are many resources for subsequent pregnancy, and a good place to start is my friend Aleena’s research described in our post. I also strongly recommend that you regard your mental and emotional health as in need of support and safeguarding during this subsequent pregnancy, as much as your physical health. In the US, other resources can be found at organizations such as http://nationalshare.org/ and https://starlegacyfoundation.org/ and http://www.the2degrees.org/about-us.html
I wish you strength and courage during this pregnancy,
Susannah
Wow your story is so similar to my own. I too was pregnant and had recently found out it was a girl. My husband and I watched on in amazement as she moved around vigorously during an ultrasound. My due date was estimated at August 16, 2020. I had had a pretty easy going pregnancy aside from some expected symptoms. So on May 24 at 28 weeks along when I mentioned to my husband that I had not felt the baby move all day, we both didn’t panick but decided to wait it out and see. I lied down and drank something cold, pressed on my belly, and like you said even tried to “will” the baby to move but there was nothing, I woke up at 6am and took a walk but by the time I made it back home, still.. nothing. That’s when I realized something was terribly wrong, my husband was still asleep I told him I was going straight to the ER and I did not wait to see if he was coming as I began to feel a bit panicked. He still was moaning in his sleep that everything was alright. In the ER room I was hooked up and checked for the baby’s heartbeat, I heard nothing but the faint pitter patter of my own heart. My stomach dropped. By then my husband had caught up and was at my bedside. The Dr came in and did an ultrasound, I teared up seeing my baby lie motionless on the monitor screen. She was not moving. By then I was already in tears. “Nothing.” The Dr said. My husband held me and we both broke down as we could not believe it to be true. I had to be induced the next day and got to hold my baby girl she looked as if she were sleeping and i cradled and held her for what seemed like forever. There were days I woke up and instantly would start crying for my daughter, it’s hard and even harder when your questioning what went wrong and there is no definite answer.
Dear Heaven,
I am so sorry for your loss of your precious daughter. Your due date is slowly approaching and I remember well reaching that devastating milestone after Wilder’s death and birth at 38 weeks… I remember in the hospital when Craig and I heard that sound during the scan–the lack of sound where we expected Wilder’s heartbeat. We both immediately broke down also, in utter disbelief, as the opposite of what should happen was happening. It is bitter indeed not to know why our babies died and for me, I am pretty sure that I will never know. I work to try to make this less likely for other moms and dads but it is an uphill battle. Strength and courage to you and your husband,
Susannah
Susannah! This is my first time writing about my grief in a social place! But you and everyone else made it easier for me to talk about it! My son Shayan was stillborn on April 4, 2019 when I was 38 weeks. He was absolutely healthy, my husband and I are healthy and active people and my first son is absolutely healthy. My pregnancy was flawless and no issues. I read you said that you treated yourself with a massage few days before the lost of your beloved son. I did the same and I have been thinking that could have been the reason! I’m now 41 and still trying to get pregnant but too afraid , and it’s breaking my heart when I imagine my son living his life with no siblings😭😭he even says this that I wish I had a sibling like my friends😞😞I’m almost giving up hope as I’m too afraid of getting pregnant with complications due to my age now, on the other hand I don’t know how to overcome this want to have another living baby and a sibiling to my son❤️I really appreciate yours and anyone dealing with these complicated feelings advice🙏🏻
Dear Mahsa,
I am so sorry for the death of your precious son Shayan last year, and I am so glad that you decided to write. As you read in my story about my son Wilder, after he died I went through every part of my pregnancy in my mind to try to come up with anything that could have explained his death. It was so crazy that my pregnancy was absolutely perfect, with me and my husband in perfect health, yet my baby could still die for no reason at full term–38 1/2 weeks, almost the same gestational age as your son Shayan. I think that one thing that is known about stillbirth is that often, multiple factors work in combination to cause the death, rather than one single thing. This is also true of deaths of those who were born alive, including adults of course. I don’t know what combination of factors led to Wilder’s death and I have had to adjust to the fact that for me, I will almost certainly never know. Instead I try to look to the future and do what I can to raise awareness of stillbirth and contribute to research about possible causes, so fewer families have to endure this awful grief. I hear your worry over trying to get pregnant again. I had my last child just before I turned 40 and I was very worried throughout his pregnancy about complications due to my age. This is very different for each individual and I think one really helpful thing is to have a physician you really trust and feel comfortable with, if that is possible, in order to discuss the possibility and the potential risks. Guilt, perhaps for your living son who says he wants siblings, is a very very difficult emotion (I was writing a little about that in a prior post today) and I would offer my hope that you can overcome and put aside that feeling, if possible, and try to replace it somehow, with patience and kindness for yourself. Finally I would say that what helped me the absolute most in the first few years after Wilder died was finding a friend (Lisa) who had gone through the same loss, the stillbirth of her beloved daughter Emily. We supported each other so much through those early years because we really knew what we were going through. So many people have experienced stillbirth; once you start to talk about it you find that they are people you already know, but there is such stigma that people are shy or afraid to discuss it. I hope that you can find a friend to support you in this time.
Wishing you strength and courage,
Susannah
My story is a bit different but I can still relate to yours after I read it. I gave birth on April 14th 2020 to my first son Elyan. It was early birth in 29th week of pregnancy. He was born alive. I was not able to see him or hold him due to corona virus situation. He stayed on intensive care unit. We were able to see him on video call made by nurses for 10 sec daily, which was the waited moment of the day. For 11 days he was doing great. Everything seemed to be going good. Suddenly on April 15th at 6:44 in the morning we receive a call from a hospital. The doctor informed us that suddenly he started collapsing. 5 hours later he passed away. We don’t know the reason of my early birth or his death. For now just a bit over 2 weeks after the only thing I can think of is getting pregnant again. It makes me feel guilty and worried at the same time. What if I can’t? What if it happens again? We don’t know the reason, will I be ever able to deal with such stress and worry?
Reading your story helps a lot. Thank you very much for that.
Dear Simona,
My heart breaks for you and your beloved son Elyan. It is always so crazy to me that although there can never be any words to express our grief and devastation, still we seek out words. I am seeking words of comfort for you, though I know there is sometimes no comfort to be had. All I have are words of experience. Your Elyan did live for 11 days, while my Wilder died prior to birth, but these deaths are on a continuum of death and loss with many similarities. The unknown–why did Elyan die? What if it happens again. I can completely relate to these anguished queries. I had the identical reaction of immediately wanting to be pregnant again and fearing if I could not. For me, Wilder was not only my first son but my first child; not sure if this is also true of Elyan. Due to the fact that I was found to be positive for TB during my pregnancy with Wilder, I was told by my infectious diseases doctor that I would have to wait to try to get pregnant again, after Wilder died, in order to be treated for the TB. I vividly remember that doctor’s appointment in excruciating detail. I was utterly devastated to have to wait even a second to try again. In terms of not knowing the reason why Elyan died… Wilder would be turning 21 this July 13 and so I have lived 21 years not knowing. The way I think of it, I have learned to accommodate the not-knowing, and to live with it alongside me. It does not now interfere with my daily life on a regular basis, yet at the same time, the not-knowing has become an integral part of me. The cruel aspect of COVID-19 that increased your separation from your son, I cannot imagine. I am so sorry for that. I can only offer my experience that as you move forward through time, things will change and I believe that they will become more bearable. With warm thoughts to you,
Susannah
I lost my beautiful baby girl Zaela Gwendolyn 3/26/2020 due to cord accident, her due date was 4/6. She was perfect. We’ve been devastated. We’re already trying again because the loss took such a psychological toll on me and they said the benefit outweighed the risk, plus since the loss wasn’t to do with anything with my body they said it should be ok. I think I already may have reconceived and I’m terrified but hopeful. A new baby is certainly no replacement, but I am desperate to be a mother. I feel guilty though as if I am. These months have been the hardest of my life, and I’ve had a hard life as it is. I almost didn’t hold or see her because I was afraid of what she would look like, but through my eyes she was still amazingly perfect despite the effects of the trauma of her passing. They handed her to me immediately after her birth and let us see her some, then went and cleaned her and brought her back a couple more times. I’m so grateful for those moments. And also so destroyed that I never got to “mommy” her—bathe, change, burp, feed her.. but her skin was so delicate and I was so afraid to hurt her beautiful little body. She had her daddy’s curls and eyes and nose, and mommy’s mouth. Thankfully they allowed daddy in the room despite coronavirus and my nursing and obgyn team was wonderful, caring, and as gentle as they could be. I had been so scared to give birth, but my emotional pain caused me to boss up for the physical part (although I did get an epidural) and that was the easy part. I never got to hear her little cries or know who she would’ve been. And I feel like they should’ve caught it. The week before I messaged my midwife with hour+ long strong contractions two nights in a row and she dismissed it as Braxton Hicks (for over an hour, twice?) When we discovered that her heart had stopped beating, the ultrasound showed her head in my pelvis, as if she had been trying to be born. The signs were there. It had been a routine weekly checkup (3/24/2020) when we found out and Daddy was at home. So I came home to him, we cried, packed our bags, I showered and we went to be induced. We were there for 2 and 1/2 days. Leaving empty armed and coming home to a home with no cries was one of the hardest parts. They have been attentive to my psychological state though and I am on an antidepressant that has helped some. She was supposed to be the first grand baby for both sides of our families. We were so ready for her. Her nursery was jam packed with everything she ever could’ve needed. We had her cremated and got her a beautiful little wooden urn with her photo on it, and each member of the family has a little piece of her in a piece of urn jewelry. I have 2 pieces and a tattoo now in her honor, and I’ve started “Zae’s corner” in my bedroom with many lights and photos and candles that I hand vinyled to remember and honor her. I’ve just been keeping as busy as I can. I have good days and bad days. I’m not through it, but I am further away from it and I have seen much kindness from friends, family, and acquaintances. This loss has caused me to struggle with my faith as well, so this has just totally devastated me. My thoughts are with all you other mamas as you mourn your babies. A mother should never have to lose her child. I hope we all find some peace.
Dear Kerensa,
I am so very sorry to learn of the death of your beautiful daughter Zaela. Your story brings back the vivid memories of my son Wilder’s birth and the few hours that we spent with him before I had to say a final goodbye. I wish I had had the strength and courage to really ‘mommy’ him, to take off the clothes the nurse had put on him, to bathe him, to dress him, to caress his beautiful hair and examine his toes–which I never saw. I was too afraid and too in shock… and no one suggested that I do any of those things. I am so glad that your husband was with you despite COVID-19. It is horrifying to think of mothers who are right now suffering through the deaths of their babies all alone. Yes, there is all the subsequent pain and sorrow of not knowing who she would have been, or who my son would have been. He would be turning 21 this summer! A man… What would he have looked like? Who would he have loved? What might his passions have been? What would his friends know him for? Such a lifelong, endless loss. Yes, and coming home empty-armed. I left the hospital in a wheelchair as per protocol, with a horrible bunch of flowers in my lap. I hated those flowers but said nothing, fearing to hurt someone’s feelings or more out of shock. I didn’t want flowers, I wanted my baby in my lap! I too found help in keeping busy, those first days and weeks and months–sending out letters, designing ceremonies of remembrance in the US and Vietnam, writing in a journal. It helped. Thank you very much for sharing your story here. Peace to you,
Susannah
Reading your story makes my heart ache as our stories are so similar. I wish I could give you a giant hug.
We had our little Hannah on July 22nd 2020, today was her due date. She was 39+0 weeks when she was born asleep due to a cord accident. I woke up at 7:30 am and noticed I could not feel Hannah move so I did what they tell you to do in the event that you experience decreased fetal movement. I drank juice and had a power bar and rested on my left side only to feel nothing. I was told to immediately go to my Doctors office. I didn’t have an appointment so I anxiously waited for 45 minutes before I was called in to have an Ultrasound. The ultrasound tech pressed firmly on Hannah’s little back to prompt her to move… nothing. A midwife was summoned quickly into my room where she confirmed Hannah’s heart was no longer beating. I was in labor for 12 hours, pushed for 5 hours. Hannah was sunny side up and was stuck in my pelvis. My epidural became disconnected from my back for two of those hours… all back labor. Finally, an OB unknown to me delivered Hannah using forceps and episiotomy. No one prepares you for that emptiness you feel when your baby has submerged from your body.
Immediately they placed Hannah on my chest, I was able to hold her for 4 hours. I studied her face, little fingers and toes. She looked just like her daddy. We had her cremated and hope to spread her ashes at Big Sur.
I still wake up at 2 am and 5 am and cry. I catch myself staring at her picture trying to make sense of everything that has happened. My husband and I have already started talking about trying as soon as we possibly can. I know we will have debilitating anxiety with our next pregnancy (if we’re blessed with another one).
Dear Brenda,
The story of the death of your beloved daughter Hannah is just devastating. I’m so terribly sorry for your loss. So very fresh, just a week ago. I remember those early days. Exhausted, sleepless and stricken with grief. The thought of scattering Hannah’s ashes at Big Sur (in the sea or mountains I think?) is very beautiful. We have not been back very often to the place where we scattered Wilder’s ashes, in a lovely meadow clearing in the woods, but we are planning to go in just a couple of weeks. Being there, knowing his ashes mingled with the grass seeds and the dirt, is a very special feeling. My mother found out that sheep graze on that hillside and a local artisan cards the wool from those sheep, spins it, and makes blankets out of the wool, and she purchased one of the blankets for me. So special. Yet nothing compared to our empty arms. I am glad that you had that time to hold Hannah and look her over as a mother would. I understand the urge to try again immediately, coupled with the fear of doing so. I have been there… Wishing you strength and courage to move forward through time,
Susannah
Hi Simona
My story is similar to yours. Our son Harrison was born 24+5 owing to a spontaneous labour. We don’t know why this happened. He was born alive and fought for his life for 9 days before passing away. He fought so hard, but contracted sepsis and just as he was getting over that, his little bowel developed a hole. We watched his medical team complete 3 rounds of cpr on him before his tiny body couldn’t take anymore.
I’m absolutely devastated and miss him incredibly. Each day just feels like going through the motions and the only time I feel any peace is when I’m asleep.
We have a strong network around us and Harrison’s death has certainly made our relationship even stronger than it was. However I just know that this has changed me forever and I can feel in my heart that I will never stop grieving for our beautiful baby boy.
I too feel the conflicting emotions of wanting to get pregnant again straight away, but then also feeling guilty about it and so frightened of future pregnancies and not wanting to put another child through what Harrison has to go through.
Reading all of these sad stories makes me feel like I’m not alone with the thoughts and feelings I’m experiencing. I send love to everyone and it makes me so sad that other parents have had to experience such loss xx
Simona if you want to link up Iet me know.
Hello again Sophie,
I just wanted to thank you so much for sharing your story of your dear son Harrison and his life and death. Your story also displays the reality that stillbirth and newborn death are really on a continuum of loss. So many of the causes of stillbirth also cause newborn death–and the grief and devastation of these deaths are the same… as well as the complex and confusing questions about when to try again. As usual there is no one right answer and we must all feel our way forward. It is so good that you have a strong network surrounding you and closeness with your partner as you move forward in time. Wishing you courage,
Susannah
Dear Susannah,
I came across your blog and felt compelled to post my story too regarding maternal stress and stillbirth.
I am a Mother of 5 children, 15 pregnancies and recently had a stillborn baby girl Emberly. The previous December, not even 5mths prior, I had lost my teenager daughter and was under severe stress, in hospital daily but being told I was fine, desperately crying out for help yet feeling nobody was listening to me. I believe the stress I was under directly contributed to my daughters demise and that if I had greater support as I was asking for and a place I felt safe, then my daughter would still be inside me today.
Regards, Courtney.
Dear Courtney,
I am so very sorry for your loss of Emberly and your teenaged daughter, such traumatic and devastating deaths and so close together. The severe stress of your older daughter’s death sounds nearly unbearable. We know that different kinds of psychological conditions can affect health and wellbeing in similar ways to physical conditions, but the effects of psychological conditions are in general somewhat less well understood. I am hoping that my research on stress and stillbirth might play a small part in helping to shed some light on possible connections, so that doctors and other caregivers will be better able to support pregnant women in identifying and alleviating problematic conditions. But I think it is also important to realize that stillbirth, like all kinds of deaths, is usually not due to a single thing that happens, like a light switch turning a light on or off. There tend to be a number of factors that all together result in death and our loss of our babies, rather than a single factor. And there are countervailing forces as well. Your love for your Emberly and your protection of her within your body for many months, like my love for and protection of Wilder, were, I believe, so important in trying to keep our babies safe and healthy.
Sending you courage,
Susannah
Hello Susannah,
You’re story was so familiar, I also had a stillbirth at 33 weeks. This happened on 04/02/2020. Like you I did everything I had to make sure this pregnancy was perfect. I had previously had many miscarriages that had taken place before there was a heartbeat. So, when my son’s heartbeat was there my husband and I could not be happier. The picture of you holding Wilder I could feel you’re pain and devastation. Right now I feel so lost, even my clothes that fit so snug now are so baggy it makes me so sad. I know I will probably never get over it. I don’t know if I will ever be able to remain calm during another pregnancy because I will be so fearful of what has happened. It scares me to think about it because I am not young, I am 37 and that might have been my last opportunity. I try not to feel bitter, angry, and lost but it is so difficult to control all of my different feelings. Thank you for sharing your story, I felt as if it was my story and it helped me know there are other who know what my suffering is like and how emotional this is.
Hello Kallai,
Thank you so much for sharing your story. I’m so terribly sorry for the death of your son, just three weeks ago. So fresh and vivid and hard. I think only the forward motion of time can support us as we grieve. Things become less excruciating as we adjust our minds, bodies and spirits to our new reality. I never have got over Wilder’s death but I have learned to live alongside it. I was just under 40 years old when I had my last child. There is still time, I think. Subsequent pregnancies are so very hard, as my dear friend Aleena outlined in her important research. I think there is no escaping that fact. But for me, I found it is still possible to adjust, to move forward, and to endure my subsequent pregnancies with all their worry and uncertainty. Sending you hope and strength,
Susannah
Hello Susannah. I gave birth to my son recently after being diagnosed with sudden onset pre eclampsia. My story starts a week exactly before I went into the ER to have been told Atlas’ heart was no longer beating. My beloved dog of 15 years was taken to the vet after shortness of breath, lethargy and a terrible cough. I was told he had fluid in his pluerial cavity from cancer and a weak heart. He was in extreme discomfort and I decided to put him down the next day. That night I stayed up all night in intense pain that my best bud was no longer going to be in existence with me as I listened to his labored breathing. The next day I went through the agony of doing what I knew was right but could not control my immense sorrow. The following week to the day I noticed decreased movement in Atlas, and an on and off again headache and swelling all over my body. Immediately the ER put me on magnesium for seizures due to my high blood pressure. I started my induction that night and the next night at 8:59pm I gave birth to Atlas. He was 35 weeks and his head was already down so four good pushes was all it took. He was such a handsomely formed babe. All they could tell me was that I had pre eclampsia but I know that the extreme sadness and the stress related to my pooch dying caused my high blood pressure that subsequently decreased his blood oxygen intake. I simply wanted to give you a case study where the relationship between extreme loss of a loved one brought about such stress and/or my fight or flight response that it caused my precious boy to perish inside me. I’m so sorry to women who have no answers at all. And I’m sorry I was ignorant to what my greif did to my Atlas. Thank you for your work my fellow mother.
Hello Nicole,
I am so very sorry to know of the death of your precious son Atlas. Please also accept my sympathy for the loss of your dear canine companion. Grief is such a powerful emotion that can overtake us and overpower us. I have learned that very often it is a multitude of complex and intertwined factors at many levels, from social to biological, that can sometimes lead to death. For myself, I still wonder and ponder over what factors led to Wilder’s death, and this is a strong guiding force in my current doctoral studies. Wilder died nearly 21 years ago, and what doctors know now about risk factors such as cholestasis of pregnancy were not well-known then, and this helps me understand how medical and clinical knowledge are constantly evolving. I try to play a tiny part in urging for increased research of causes, as a way of trying to prevent stillbirths in other families. Thank you so much for sharing your story. Wishing you peace and the passage of time to support you in your great loss,
Susannah
we have same reason i also have pre-eclampsia, at 38 weeks i went to my weekly check up and found out theres no heart beat. it was May 24, 2020 i delivered my son sleeping. i cant move on and everyday i cry and i think im gone crazy. guilt, anger jealousy all the negativity is everyday with me i don’t know how to handle no one in my family understands me. everyday i search on google about stillbirth, why God allow this? whats the reason?, where baby goes now? where are there now? they will rebirth? all i ask google about it. (crazy right?) till i came to this page. i want to get pregnant too soon but this covid right now i don’t want yet but how i move on without pregnant again? this my first time and i expect i have a baby right now but my arms are empty! my baby is perfect but i did not hold him bcoz im scared now i regret i did not hold him when he was born. why i did not hold him or touch him. I did not even watch him longer than 10 sec. i only have a picture of him and he’s 3D scan. i watch it everday whenever i miss him.
Dear friend,
I am so sorry for your loss of your beloved son. My son Wilder would have turned 21 on Monday and even after all these years, the pain is still there. I hear and feel your fresh agony. I also felt the same way, wanting to become pregnant again immediately, and for me, the reason I could not was that I was positive for TB and had to undergo a course of medication for three months before I could try again. The forced waiting was terribly painful. I was “lucky” that the medication course was new and replaced the usual treatment which would have taken six months. I also searched everywhere, everywhere to find out anything I could about stillbirth and to find anyone with whom I could share my story. I ended up on the site of one support organization, Mommies Enduring Neonatal Death (MEND.org), where I found another mom whose daughter Emily had been stillborn just a month before Wilder, on June 10, 1999. Emily’s mom and I started corresponding and we became each other’s rock through that first terrible year. There are support groups online these days. Here are some, in case they are helpful.
https://firstcandle.org/online-support-groups/
http://nationalshare.org/online-support/
https://www.mend.org/virtual-support-group-links
https://starlegacyfoundation.org/support-groups/
Sending courage and strength,
Susannah
I just came across your post. My little baby boy Yash was born sleeping on 10/26/2020. I was 38+3 weeks pregnant. I noticed decreased movements and told my husband to check. He is a doctor himself. We just thought to go in ER and get me checked. Even he was casual about it, so we had our dinner, fed our 2 year old girl dinner and left for ER. The rest of the story is as traumatizing as everyone else’s where they couldn’t find his heartbeat and declared him dead. He was such a healthy and beautiful baby – 21 inches long and 7lb 8oz. There hasnt been a single day that I have not missed him or cried not being able to hold him in my arms. I cant wait to try and be pregnant again to be able to hold him again in my arms. Just before he was born my husband and I used to think that our baby girl is perfect for us and now even with her there around us he is being missed every single minute. I still dont know how to behave, how to get over this grief. Everyone around me is way too supportive but I still struggle every single day. I see your baby would have been 20 years old. Does it ever stop hurting? Or with time you just learn to live with the pain? There are moments when I feel like snatching out my heart because the pain/grief is so intense. The only thing that really helps me is a hug from my baby girl.
Dear Swati,
Thank you so much for reaching out (I feel this network of everyone who writes on this blog, weaving together across the globe and across the miles, somehow). I am utterly sorry for the death of your Yash, just a month and a half ago. The story you tell is, as you say, so similar to my own and those of so many moms who have posted here. The certainty that nothing could be wrong, and then the birth of a beautiful perfect baby–but dead. The intensity of the grief afterward. The shock of the loss of a real, individual, unique person whom we will never know in life. Yes, Wilder would have been 21 now, a year older than my oldest living son. Every person’s experience is different so I can only ever answer for myself, but I can tell you that for me, the daily pain did subside, and I live the vast majority of my life now without hurting–but every year, there are a couple of times, like his birthday or the holidays, when I allow myself to really really remember, and then the tears spring up as if it were just yesterday. In a way this makes me feel better because it means that I have not forgotten him… I think for me, I have just learned to live alongside the reality of Wilder’s death. It is very strange because without his death, I would not have had the same living children I have (I would have been pregnant at different times, and had different babies, I assume), and of course I adore my living children. I am not a person who believes in ‘things happen for a reason’, so for me, it is just a matter of living with the strange reality of being grieved over the death of Wilder, while simultaneously living my life and doing my best…
Wishing you strength and courage,
Susannah
Hi Susannah. This is probably the first place I am sharing my story at. I delivered my baby girl Dyuthi (meaning radiant light) on Feb 6,2020 at 39w 2 days. I did not have any sort of complications or problems throughout my pregnancy. I did not have any stress and was super happy all the time. At 39w 0 days, on a Tuesday night, I started getting contractions which came and went every 20 minutes or so. I was asked to wait till it became stronger. And after waiting for around 24 hours, we headed to the hospital (till this time we were not aware that the baby was gone). We stepped into the hospital, I was asked to change into the gown and when the fetal monitor was wrapped around, there was notHing we could hear. She was alive with her heart beating at 148 just the previous Wednesday on my regular OBGYN routine checkup. This picture of getting to know that she is gone has been constant in my mind since then and it’s a fight every morning and night with myself to wake up and try to function normally. Till now we haven’t found any reason as to why she left us. I become clueless and helpless. I’m not sure if I will be normal ever again. I chose not to see her since I had this imaginary picture of her perfect face set in my mind and did not want to disturb it. I am now guilty of not seeing her which comes and goes in waves. The grief has been too much to handle and I am just continuing with the hope of having a live baby in hands in future. Your story made me write my heart out here, Thank you so much, Susannah. Much Love!
Dear Kruthi,
Thank you so much for sharing the story of your precious daughter Dyuthi. Your story is so familiar to me. I know the feeling of a perfect happy pregnancy that inexplicably ends with death. The grief and devastation are overwhelming. For my part, I found sustenance in tending Wilder’s memory. Just two weeks after he died, my husband and I held a small ceremony with some friends and family. We spoke about Wilder and scattered his ashes in a place special to us. We sent out a card to many many of our friends and family to announce Wilder’s birth and death. I carefully created a notebook with memories of Wilder, and for nearly two years I kept a journal of the daily reminders and memories related to Wilder’s birth and death. These acts were soothing to me, and they helped me to progress through time. I also read everything I could find about stillbirth, even though there was not much. I read about other types of devastating losses as well, of newborn babies and children, as reading about how others coped, and the stories of other mothers and fathers, somehow was soothing and helpful to me; instead of increasing my pain, these these reduced my pain. Everyone is different though. Honestly, nearly 21 years after losing Wilder, I’m not sure I ever became normal again. My whole life changed, my career, everything. At the same time, I did have three living sons, and I did laugh again, and smile again, and feel joy again. I always think of it this way: There is the death of my firstborn, Wilder, which can never be anything other than grief, devastation, blackness. Yet alongside this grief, next to it, maybe in some parallel universe, there has been happiness, new life, and even the joys of the new career in epidemiology that I only came to because of Wilder’s death and my laser focus on stillbirth. It is so strange to have grief and happiness coexist in one body, but I have found that they do. Regarding your feeling of guilt over not seeing your daughter, perhaps you can consider that you “saw” her every single day in your mind’s eye and your heart, and held her strongly in your body’s arms. I try to let the pain of not seeing Wilder’s eyes and feet slip away from me like little soft waves on the surface of a great ocean that I am sailing slowly away from. Peace to you,
Susannah
Hi Elizabeth. I instantly connected and share the feelings
of frustration and uncertainty of not knowing what went wrong with the pregnancy, the questions and all the blame of wht did I not do right to prevent my Aidan’s death. I was admitted to our local hospital for two long weeks just to come home without our precious bundle. Crying,feeling miserable,full of unanswered questions the constant reminder of breasts tht are crying out for relief!!!!
Aidan was stillborn at 26 weeks as I was told due to my blood pressure being too high, blood penetrated his brain and he suffered receiving oxygen. His heart stopped beating on the 3 Dec 2019.
We r still coming to terms with his death but it’s very difficult as people always want to sympathize with us.
God’s grace is keeping me, i’m living each day second by second,constantly staying in prayer.
Thank you for sharing your story. It reminded me that other women are also experiencing this trauma and made me want to support them in every possible way I can even if I can only pray for them.
Dear Rosa,
So many thanks for sharing a part of your story and your loss of your precious baby Aidan. I remember that reminder of the baby I should be holding in my arms when my milk leaked even while we were scattering Wilder’s ashes in the grass. So very poignant. I agree with you that it somehow helps to share our stories, so that at least we know that we are not alone. Someone else has gone through what we went through and are going through. Someone else feels or felt the way we feel or felt. We all grieve differently and hearing the many stories of women and men who have suffered the stillbirth of their babies does help us to forge ahead, day by day.
Wishing you peace.
Susannah
Hello my name is lisa,
Our daughter poppy Sunshine was born sleeping 20.11.18 at 34 weeks. Her autopsy was also unexplained, I find this such a hard pill to swallow as what’s there to look out for next time? We are still trying for not a replacement but a baby to hold we are left with such empty hearts and arms. I had gone to the hospital with reduced movements and was put on the ctg machine. Her heart rate was unreasuring so a obstetrician was called in who went over my results and found it wasn’t cause for an a emergency and to go home. When I replied and said I still hadn’t felt movements he said to go home and have a moro bar and to come back in the morning if I was still concerned. Well I did go back in the morning and it was to late.
So heartbreaking thinking about the what ifs. What if I had further monitoring what if I just refused to leave. Waht if the concerned midwifes called me back as they didn’t want me to leave.
I also remember the sound on that heart monitor picking up my own racing heart. It’s a pain that will always be there
Dear Lisa,
I am so very sorry for the loss of your beautiful daughter Poppy Sunshine. What a lovely name. We also tried everything to find an explanation. The decision to allow an autopsy was hard but we felt we had to do it, and of course there was no cause still. Years later, I wrote a letter to the two people whose names were on the autopsy report as having performed it, just to tell them that I hoped and assumed they treated Wilder’s body with respect. Some of the only people who ever touched him… I am so sorry for your agony. The what ifs are very hard. I think there is only time which marches forward and carries us forward with it and eventually gives us a little tiny bit of peace, somehow. With you in spirit,
Susannah
Hi
We lost our baby mukundi at 23 weeks and a day on 26 December 2019.I suddenly had a runny tummy and vomiting,I also had abdominal pain .So I was rushed to the emergency room,I was given antibiotics on a drip and I requested for a scan,they did a scan and baby was in breach position,and my cervix was closed at 17:30pm.The pains I assumed was my uterus stretching worsened and I went back to the emergency room at 10:30pm,then I was taken to ward the pain increased then I had no Idea I was in labor,4:30am I went to the loo and saw some unsual discharge which I learnt was the mucus plug,pushed my baby boy out,he was too small 490g they could not save him…It’s been such a hard time for me,they showed me my baby but he was sleeping…Everything happens sooo fast
Dear friend,
I am so sorry for the loss of your little Mukundi. Such a whirlwind of action that happened around your baby’s birth, with you and Mukundi at the center of it. Thinking of you and sending strength and hope for the days to come,
Susannah
Hi Susannah, I lost my baby boy Neel last month. He was ok till 15th Feb 20 but on 18th my sonography doctor declared that his cardiac activity stopped. I am still finding a reason, as I had completed 37 weeks and everything was normal. I delivered him on 19th Feb 20.. But I refused to see him as I didn’t have courage to see him. I hav this guilt that I didn’t even see him but I never wanted to see my baby who was so active in my womb for 9 months like this… I miss him like anything… I loved him before I saw his face so I wanted to keep those memories alive… I hope he is not angry on me.
Dear Swati,
Please see my comment in reply to your other comment farther down, but I just wanted to say it makes me glad to know your son’s name. I will think about Neel. I think that babies are not angry, they only felt relaxation in our wombs as we carried, fed and rocked them while they were alive. Wishing you time and comfort and peace,
Susannah
Today is Christmas eve 2019. Our daughter would have been 8 days old today. It would’ve been her first Christmas. Instead my husband and i are still in bed just hoping to get through another day. I lost my baby girl Zalayah at 37 weeks and 3 days. We found out on December 15th that her heart had stopped beating. I was induced and gave birth to her on Decembee 16th. I can’t help but think of how i failed her as her mother. How could i not know something was wrong and she needed me. I know God has a plan and i have to accept that this is part of it. I thank you for sharing your story. Knowing wilder has 3 healthy brothers who celebrate him gives me comfort and peace. I already am thinking about Zalayah’s baby sister or brother. I know she will never be replaced but i think it may help us to fill the empty holes in our hearts.
Hello,
I am so very sorry for your loss of your baby daughter Zalayah. I remember so well finding out when Wilder had died, and the time between when we knew and when he was born. Craig and I went through so many thoughts as you describe, wondering over and over what we might inadvertently have done and how this possibly could have happened. I do believe that I did all I could to care for Wilder during pregnancy and I am sure that you did too. Having Wilder’s younger brothers has been just as you say, not a replacement for him, yet on the other hand, an immeasurable comfort. The holidays are a particularly hard time for many of us whose babies have died, because we think so poignantly about what might have been. This would have been Zalayah’s first Christmas, yes. I light a stick of incense for Wilder on the holidays as a way of remembering him, and I decorate his shelf with some of our Christmas ornaments. He is there with the rest of us and is always in my heart. Wishing you peace and strength as you move forward day by day,
Susannah
Thank you Susannah. That is great what you do for Wilder. We did get Zalayah some Christmas ornaments and have two shelves with her pictures, her blanket and castings.
I think its a great idea to decorate her shelves as well.She would have been a year in just 6 days. I can’t believe it has already been that long. I often come back to your page to read your story and all of the comments to bring me some comfort. Its heartbreaking how many have gone through this pain. I am currently 34 weeks pregnant with our second, a boy this time which was hard to find out. The entire pregnancy has been stressful. Sometimes i wonder if we tried again too soon. Thank you for sharing your story and giving women like myself a place to feel some comfort
Hello again,
It makes me smile to think of little Zalayah’s Christmas ornaments. Next week I will put up our ornaments for Wilder as we do every year. I am very happy for you and your husband that you are pregnant again, and I feel deeply for you as you draw nearer to your delivery date. I remember so well how that felt. I can only send you courage and strength. You are not alone. Of course it is stressful, and you will always miss Zalayah (what a beautiful name!). Wishing you peace this holiday season,
Susannah
Now im pregnant again after 4 month delivery. I delivered in 4 aug 2019, now im 7 weeks pregnant. I dont know what to do, is it safe for the baby?
Dear Sandhya,
Thank you so much for posting. I am not a doctor and I am sure that you know that the best person to answer your questions about safety in this pregnancy is your doctor. Sometimes it can be hard to find a doctor with whom you feel really comfortable. And sometimes we don’t really have a choice about the doctor we see. Whether or not you have a choice about your doctor, I think it is really important to ask a lot of questions. Don’t be shy about asking many questions, or asking the same question over and over. Maybe we don’t understand the answer the first time, or we do understand, but we just need to keep talking about our concerns. There are unfortunately many risk factors for stillbirth, and it is also true that having had one stillborn baby does increase the risk that this will happen again. But this depends on many other things, such as the reason for the stillbirth happening in the first place. For me, we never found out the reason for Wilder’s being stillborn, so we could not rule anything out for my next pregnancy. This really increased my anxiety. In the event, you can see that I did go on to have three more babies, all liveborn and healthy. The chances that this next pregnancy will be fine are very good… but we know, who have suffered the loss of our babies from stillbirth, that good chances do not always translate into good outcomes. Stress and anxiety during a subsequent pregnancy are so normal and understandable. Sometimes doctors don’t want to talk about the possibility that “it might happen again” because they don’t want to alarm us. But, we are already alarmed and stressed. It is my feeling that the best thing you can do is to talk to your doctor (or doctors) and also if possible, to other moms who are going through, or have gone through, the same things. The next pregnancy is challenging, no matter what the outcome. Talking through your concerns, and knowing that being anxious is a normal feeling, can maybe help a little bit. Other than that, we can only keep moving forward in time, taking care of ourselves the best way possible.
Wishing you strength and courage,
Susannah
Thank you to everyone who speak up openly about their pregnancy loss. I am happy that Wilder got to have 3 more brother that gives us hope that pregnancy and life after a stillbirth is possible. I was 26 weeks and gave birth to my stillborn baby girl on 20 August 2019 after a miscarry on 3rd December 2018. The umbilical cord got twisted and tangled like a telephone line nd took my babies oxygen support. It has been 3 month and 1 year altogether since our first lost of miscarry at 8 weeks. The year has not been easy…doctors have no answer as to why this happened I had no blood issues was perfectly healthy nd bby too. This breaks my heart to see that some women has to go through what we do…I am married fr 2 years and we don’t have children yet and Wilder’s existence and his brothers that came thereafter gives me hope. Lord please bless our wombs in childbearing….
Dear Georgia,
I am so happy that my story gives you hope. I am very lucky to have my three beautiful living boys. It is not easy and it is made so much harder not to know why. This is why I went back to school, to study and learn more so that I can try to make a difference by uncovering some of the “why” so that maybe some day, fewer people suffer the loss of our babies from stillbirth. But I still have to face the fact that I will never know why Wilder died at the very end of a perfect pregnancy. I wish you peace and strength,
Susannah
I delivered my sweet baby boy Kaden on 11/27/2019 at 37 weeks 2 days. I went in for a routine visit alongside my husband the day prior. Our doctor had us watch a delivery video in the waiting room because of my intense fear of childbirth (I’m 26 and this is my first pregnancy). It never crosses my mind that I wouldn’t be taking Kaden home healthy and well. I had a very easy pregnancy no complications – however I always had decreased movement. During our visit our doctor commented my stomach suddenly was measuring almost five weeks behind. He went to listen to the heartbeat – and nothing but static filled the room. I felt a hotness of nervousness overwhelm me as I looked in my husbands anxious eyes. We were sent to the hospital where it was official. I was immediately started on my induction – as I screamed out in pain for what felt like hours. I spent some time with Kaden but I was so hard on me. I am back home now and in disbelief. I don’t know who I am now. I don’t know what to do with myself. I am experiencing my breast filled with milk with no baby. I cry myself to sleep – filled with guilt. Kaden was someone’s son , someone’s grandchild , someone’s nephew. I feel I let him and so many others down. I desperately want to try again but my faith is shaken.
Dear Mariah,
You are not alone. I am so sorry for the loss of your son Kaden. I remember also when my milk came in, during our ceremony for Wilder on a hilltop at sunset where my husband asked me to marry him. This is such a raw time that you are in. Every person is different. For me, one way that I moved forward in time during those first terrible days and weeks was to find actions to take that related to Wilder. It was soothing to get books and read them to educate myself. It was soothing to create his ceremony. It was soothing and purposeful to write the announcement of his birth and death. We sent it to many people. I carefully chose the stationery and the ink for our signatures. Every detail was selected so carefully because these were the only actions that I could take as Wilder’s mother, instead of feeding and changing and burping him. Seek what soothes you and feels purposeful. Move forward in time. Strength and courage to you,
Susannah
I had my baby on 28th May 2019. I had a very normal pregnancy on the 35th week of my pregnancy I started having contractions and when we decided to go to the hospital and later they were checking my belly and the doctor told us that they couldn’t find the heartbeat of my baby and she softly said your baby is dead. Our life literally shattered into pieces. It has been 6 months and I don’t know how to feel. Somedays I am fine and I think I need to move on and some days I find myself in the same hospital room where I deliver my baby. I try to keep myself so busy but I don’t know how to move on. I am so unhappy and empty from inside that when I look myself in the mirror I can see that in my face. We are trying to get pregnant again but I feel so guilty. But reading your article and all the comments I feel like I belong somewhere and I am not alone.
You are not alone.
I always say that I unavoidably joined a club when Wilder died. I didn’t want to be in the club but here I am. And here you are. At least I can assure you that as you already see, in this club there is much shared experience, understanding, compassion. I think I mentioned that I met my dear friend Lisa online after our babies died and despite never meeting until years later, in those early hard hard months we got each other through dark days. It was our shared experience that did it. I found that reading, talking, thinking and writing about Wilder’s death and life helped me. And time. Just forward motion in time.
Thinking of you and wishing you strength,
Susannah
Hi Susannah… I lost my baby too. He was stillborn. The reason is unknown. I keep on asking God why this had as even my doctor dinnt give answer to my question. I did not have courage to see my baby boy with closed eye, so I didn’t see him. But I have this guilt of not seeing him. What to do Susannah I never wanted to see him like this. Nobody can replace him as he is my first child. I loved him before I saw his face so I want to keep him alive in me. He was till 15 Feb 2020 and it he completed 37 weeks in my womb when we went for sonography on 18th Feb 2020 we came to know that he lost cardiac activity… I didn’t accept this that day and we rushed to hospital… I delivered him on 19th Feb 2020 and I refused to see him……
Dear Swati,
I am so sorry for the death of your beloved baby boy. I really feel your anguish. Guilt is so painful to feel. It is agony to have your baby die, to not know why, and to miss him so much. My baby boy Wilder was also my first child. I know what you mean. No one could ever replace Wilder in my heart, even though I have three subsequent sons. We also never found out what the cause of Wilder’s death at 38 1/2 weeks was. I have had to live without knowing for nearly 21 years so far. Although I did see and hold Wilder, I was afraid to undress him and look at his body. I was even too afraid to look at his naked feet which were wrapped in blankets. And I was afraid to open his eyes and see what color they were… the fact that I do not know the color of his eyes still haunts me. So, I can have a little idea of your not seeing your son. For me, it is a comfort to know that at least for many months, I did protect Wilder inside my own body, where he heard my voice and the voice of my husband Craig. I know what you mean that you loved him before you saw his face… It took me a while to realize that I did not have to have my son be born alive and grow up in order to know him and thus love him; instead, I finally realized that I had loved him all along, without ever meeting him in life. I have spent my life keeping Wilder’s memory green, and your little baby boy Talvadekar is green now in my thoughts as well. I have found that naming Wilder was a true help to me in grieving for him. But every parent is different in how they manage this dreadful suffering. I can only say that the passage of time provides a little soothing. Your love for your son is so powerful and clear!
Peace,
Susannah
Hi Susannah,
I am greatful to talk to you and thank you very much for your kind words. I can understand your pain of not knowing the reason… But our babies are special ones, they were so attached to us that they never wanted to be with anyone else, they just came for us, they just came to meet their mom and nobody else. From a wife we became a mom and your Wilder and my Neel did it. My best wishes will be always there with Wilder and I love you Susannah, your words are encouraging to me.
Hi Swati
Thank you so much for your kind words. It makes me very happy to know that Wilder’s memory is green for you, and you know the same is true for Neel. Stay safe and wishing you peace,
Susannah
I also went through the same. I had a healthy pregnancy until i was 38 weeks pregnant. I was complaining to my husband about nt feeling the baby’s movement.so went to the hospital the next day early in the morning.bt the doctor wasn’t able to find her heartbeat. I was shocked didnt know what to do?i wanted to hurt myself as a guilt for not being able save her. I blamed myself for everything that happened to her. I was the one who made her went through an extreme pain.what kind of mother was i??all these question never left me once. I live with guilt. I was supposed to be holding her in her 6 mnths b’day but here i am a mother without her child. Now i am 5 weeks pregnant. I haven’t even thought of visiting a doctor in this epedemic. I am trapped. I am afraid to visit a doctor what if she does not see a heartbeat of the baby. What if its not a proper pregnancy?? All these question are haunting me and i am not ready to face any of these. I hope this time everything turns out well. I hope this time i would be able to hold my baby
Dear Amuda,
I feel your pain and your anguish. Please know that you are not alone. Finding out that Wilder died was totally shocking to me also. How could this happen?? I hope that you are able to separate yourself from the guilt that you feel. I believe there were biological reasons that Wilder died and the problem is that science does not yet know all the causes of stillbirth, nor does medicine know all the ways to prevent it. The anniversaries are so very hard. I remember the first week. The first month. The first 6 months. The first years. This year Wilder would have turned 21 years old…such a milestone. Amuda, I remember what it was like to be pregnant again. The fear and worry. This is a particularly challenging time to be pregnant again after losing your first baby. COVID-19 makes everything scarier. I would like to urge you to consider overcoming your fear just a little bit so that you can reach out to your doctor or midwife for support and advice. The International Stillbirth Alliance has gathered some resources for women whose babies were stillborn and are now pregnant again, in the time of COVID-19. You can find them here: https://www.stillbirthalliance.org/resources/covid-19-resources/ I wish you so much strength in this hard time,
Susannah
Good sharing ….I just delivered my stillborn son Christopher yesterday too… He was 37 weeks plus… The guilt of thinking whether is it something I ate causing this came to my thought too, is it the pineapple ? Is it the waffle that cause high sugar level ? After birth, doctor show me the super twisted cord that could be the cause of lack of oxygen supply and blood flow which I still asking myself why he can’t untwist it ….but I do accept that he had chose his destiny and our family will move on with the cherish moment he brought to us when he is living with us in my tummy, and I know that I will miss him every night B4 I close my eyes…. I’m glad that the hospital give us the privacy moment after birth, I sing song for him, hug him, kiss him, nap with him, tell story before undertaker take him away… I came to this site when I eagerly hope to get an answer the chances and timing to get pregnant again.. thanks for the sharing and the encouragement that we still have the chance …
Hello and thank you so much for posting. I am so sorry for your loss of your baby Christopher. It is really good that your hospital gave you and your family private time with Christopher to show him your love and to make memories for your whole lifetime. I wish that I had thought to sing a song for Wilder and tell him a story and this makes me feel teary! After 20 years. I would have sung the song “I gave my love a cherry”. The last line says “the story that I love you, it has no end”, and the words “no end” are inscribed on the insides of my wedding ring and my husband’s. I sang that song for Wilder later on, at a ceremony we had for him in Hanoi, Vietnam, with many of our friends, and I sang it to my other sons when they were little. Courage to you in your road ahead. I think the “answer” to a subsequent pregnancy is to follow what feels right for you and your family.
-Susannah
I lost my baby girl 3 weeks ago. I learned her heart wasn’t beating anymore on October 18th, I was 38 and a half weeks pregnant. On October 21st I had my baby girl, Jenna. She was my first baby. My husband and I are still finding it very hard to cope with the loss of our daughter and we still feel shocked and confused. I still can’t believe this happened to us. Our hearts will forever be broken but your story me gives me hope and comfort to know that there are other people out there that went through this tragedy and got through it. I hope we can too.
Dear Farah,
I have been there. Wilder was also 38 1/2 weeks when he died. I am so sorry for the loss of your precious daughter Jenna. There are no words but we still try to find words… Yes this is a “forever” condition, and the only way to continue is just to keep moving forward in time. And to keep your daughter’s memory green as you have done here by writing about her. Now others can also think of her. A dear relative of mine was an AA member and from her I tried to learn the wisdom of “one day at a time”. May this forward motion in time help you and your husband.
-Susannah
I had a miscarriage in 2014
My rainbow baby feb 2015
And my beautiful daughter lilia payge sept 4 2019. Stillborn at 37 weeks 2 days due to a true knot in her umbilical cord. I come across this tonight and i just want to thank you for sharing. Some things you typed it was like you read my mind…felt the pain in my heart ..thank you
Hugs
Hi Reilly,
Yes, I remember reading the words of other moms whose babies died, right after I lost Wilder, and it was like they were me. The words they wrote reflected the thoughts I had, exactly. We don’t want to be part of this community but… we are… and at least we can give each other support.
Take care,
Susannah
Dear farah you also went through the same at the same time. I also delivered my sleeping baby girl on 25th oct 2019. Her name is joon shrestha. I hope our children will find peace and love. Thank u for sharing ure story. It feels like we connected through pain and grief.
Hello again Amuda,
Please see my reply to your other comment above; I just wanted to say thank you for sharing the name of your baby daughter. I will remember Joon.
Peace and courage,
Susannah
How soon after your stillbirth did you conceive again? I lost my son Sebastian Michael May 6th 2020. I prior had a normal pregnancy, with complications being I had hyperemisis Gravardium, and placenta previa. Hes currently 3yrs old and happy and healthy as ever. My son sebastian I carried up until 25 weeks. He was due August 17th 2020. April 28th I had a normal anatomy scan he was moving doing flips active as ever. My happy healthy baby boy. May 2nd came and he stopped moving, me being the anxiety ridden momma tried for once not to worry.. tried all the tricks cold water, something sugary, tapping my belly, begging for him to move. Maybe he was just sleeping. Only for 5am to roll around that night and I knew that something was 100% wrong, I had terrible pain in my hips and back and I immediately went to the ER. Static was all I heard on the doppler. That was it he was gone. No explanation three days later when I delivered him other than he looked like he may have had down syndrome and he stopped developing at 24 weeks. But no listed death cause on his fetal death certificate and never another word about went wrong just told me it was something that can just happen… i desperately want my baby back, he will never be forgotten. Is it normal for myself, and my body heart and mind to yearn so badly to fill this void..
Dear Bethany,
I am so sorry for the death of your dear son Sebastian Michael, just a few weeks ago.YES, it is absolutely normal for yourself, your body, heart and mind to yearn in this way for your son. I am so sorry. I am also so sorry to hear that you were told “it is just something that can happen”. This fatalism on the part of medical workers is one of the enormous challenges for stillbirth prevention globally. Just as adults never die because “it just happens”, same thing with babies–no one just dies because “these things just happen”; there is always a reason, although our science still is not able to uncover all the reasons yet. Meaning that continued research on causes is absolutely vital. Other parts of your story are also so familiar to me. I remember trying something sugary as well, to get Wilder moving again, but it did not work for me either, as Wilder had already died. I conceived again just four months after Wilder was born, and my subsequent pregnancy was uneventful and that son survived, as did my final two sons. But that subsequent pregnancy was very hard emotionally. However, I do not regret getting pregnant again quickly. For me, it was the right thing to do. But everyone is different. I mourned greatly for Wilder during my subsequent pregnancy.
Sending you strength and courage,
Susannah
I also lost a baby boy 2 weeks yesterday. His name was Wilder also. He was 28 weeks and they say my placenta ruptured. I am scared to think about trying again but more scared not too. Nothing will ever replace my boy but I have a strong need to be a mother again. We also have an 8 yr old daughter.. she was so excited to be a big sister. So many unanswered questions.. my heart has never hurt more.
Dear Sarah,
I’m so sorry for the loss of your precious son Wilder. How amazing that our sons have the same name… I relate to being scared to try again yet also desperately wanting to. One thing I didn’t mention in the blog is that I wasn’t able to try again immediately because I had been exposed to TB at some point, a fact that was discovered when I was pregnant, and it was recommended that I undergo treatment before trying again for a baby. I was lucky that there was a brand-new treatment protocol that lasted only 3 months rather than the older protocol lasting 6-9 months. But even that wait was so hard, and I remember crying in the doctors’ office parking lot after learning that I would have to wait before trying again. Yet also… the utterly different experience of the second time around.
Two weeks ago yesterday is such a very fresh loss and I send my heartfelt thoughts for strength and courage to you,
Susannah
Hello, thank you for your article.
Our son River was delivered on the 24.09.19 he was stillborn at 42 weeks. I have been frantically searching the internet for baby loss information ever since. I wish I could turn back time and demand there had been intervention at 40 weeks, I was just expecting to go into labour naturally. From what I have read it seems every mum feel a huge guilt; was it something I ate, did, didn’t do? The enormity of our loss is just now really catching up with me but it gives me some comfort knowing people can find a way forward but never forget their sleeping babies.
Dear Rebecca,
Yes. I have been there. I am so so very sorry for the loss of your beloved son River. I went through these same stages of trying to understand what happened–and not being able to have any answers. I ache for your pain right now. There is only one way to manage, and that is to continue to move forward in time with your aching heart. Wishing you strength and fellowship from “the club” of all of us whose babies have died.
-Susannah
I had my baby girl at 40+2 , I had a completely normal pregnancy but was booked in for induction at 40+1 because my 2 previous pregnancies (although babies both fine and healthy) I was high risk of bleeding. All through my third pregnancy I waS so anxious and worried I would die, I never once worried about my baby girl emma. I go over and over it, I completely blame myself in lots of different ways. Someone always has an answer for one way I think I caused it and then I think of another. It’s been 2 weeks since I had to have her cremated and I am just struggling. She was our last baby and I’m just utterly devastated. I don’t know how you go on from this, the only thing keeping me going is my other two and even then I’m just hopeless. How do you go on to have any more when she was fine the full pregnancy! I’ve had bloods done and allowed the placenta to be checked but we declined a post mortem for Emma’s sake! I just miss her terribly and having her in my belly, we got to spend some time with her after and have pictures but I just want her! She was perfect and fully grown and beautiful, I just don’t understand
Dear Stacey,
I am so so terribly sorry for your loss of your beautiful Emma. My heart goes out to you. This time period in the immediate vicinity of your devastating loss is debilitating and raw. There is nothing to do but put one foot in front of the other, survive, and keep our babies’ memories green. Simply by sharing your story here you have done that. Emma is in my heart now.
One thing that helped me enormously to manage was finding my dear friend Lisa who had just suffered a loss of her daughter Emily very similar to my loss of Wilder. We got each other through the first few years, and remain special friends, although in 20 years we have only met face-to-face one time. Perhaps there is a support group in person or online that may give you this precious resource.
Courage and strength to you,
Susannah
Thank you for sharing, it helps. My husband and I had a perfectly healthy pregnancy until 35 weeks, 2 days. I passed off the decreased movement as normal/stress-related because of my job as a nurse. My husband (who is a MD) wasn’t too concerned. We waited too long to get checked. Zachary was born 3/13/19. I wish everyday that I could hold him and watch him grow. My heart aches some days more than others, but I always miss my friend.
Hello Shelby,
I am so sorry for the death of your son Zachary. There are really no words. My heart goes out to you and your husband.
With warm regards, and wishes for strength,
Susannah
Thank you so much for your important work.
My parents had two living children followed by a stillborn son in the Netherlands in the 1970s. It horrifies me to think that they were strongly advised not to look at him, that they didn’t get to name him or have his body buried/cremated. He was born prematurely (I don’t know exactly, but probably between 32 and 35 weeks) and the only explanation my parents ever received for his death was that cycling a lot may have caused the membranes to break — implicitly and ridiculously placing blame on my mother.
The above is all I know about my parents’ trauma. They hardly ever talk about it, and certainly not voluntarily. I was born about two years after the stillbirth. My two older living siblings have calm and emotionally stable personalities. I do not: I have ADHD (including trouble regulating my emotions and moods), buckle under stress, and have suffered from depression and anxiety. While I realize that a thousand other factors could be involved, I do wonder sometimes if the stress my mother doubtlessly experienced during her last pregnancy influenced my developing brain.
With all this in mind: I’m happy that family experiences around childbirth receive scientific attention. Thank you so much.
Hello Elisabeth,
Thank you so much for your comment. Your parents’ experience sounds so very hard. These days the Netherlands does some wonderful things for stillborn babies and their parents, such as parents bringing their babies home for a while to say farewell. My doctoral research is on the relationship between maternal stress and stillbirth, so your thoughts are really interesting to me. There are so many factors involved, and the bottom line is that we still know very little about why babies die.
With warm regards,
Susannah
I had a stillbirth on 20.11.2020.my girl was born in 38weeks+. My pregnancy period was absolutely smooth & no complications.even i heard her Heartbeat during my labour pain.after birth she didn’t cry & dr didn’t find her heartbeats.the reason was clueless.after that nicu dr gave her cpr & her heartbeat came back but the oxygen passing way was too slow.that time she needs life support.dr put her on ventilation.but after 38hours she passed away.now i m afraid to get pregnant again..how tho get courage don’t knw??
Dear Sumaiya,
I am so terribly sorry for the death of your dear daughter, just two weeks ago. The agony of her death after 38 hours of life, I cannot imagine. My heart goes out to you. Stillbirth (death before or during birth) and newborn death (death after being born alive, but in the first month after birth) are on a continuum, with similar sorrow, similar grief, and similar bewilderment when our doctors cannot tell us WHY it happened, making us fearful about trying again. I very much relate to your being afraid to try again–the worry that ‘it could happen again’ is so strong. I do believe that one thing that can help is to try, if possible, to find a doctor you are very comfortable with, whom you can discuss your fears with. I know that sometimes it is not possible to have a choice of doctor, though. It can also help a lot to have someone to talk to. As I mentioned in an earlier post, it was amazing to me that once I started to talk even a little bit about Wilder, I found out that so many people I knew had endured something similar. Finally, it can be helpful to have just a little patience with yourself, give yourself permission to have the feelings you have, and just move forward through time.
Warmly,
Susannah
Thanks for sharing just lost my baby boy .it’s more than a week now ,can’t still believe it happend to me I have done a lot of digging and I can’t even understand how it took place.Brian I named him 25/08/2019 the best day and worst day of my life.All I have in mind now it’s how to have a baby an this time a living one.thanks again sites like this gives hope
Hello Mariama, I am so sorry you lost your precious son Brian… Thinking of you and your family.
Warmest wishes,
Sarah [Editor]
Hello Mariama,
I am so sorry for the loss of your son Brian. I have been there. Sending you hope and strength.
Excellent article. I feel like so much is lacking when it comes to treating the whole mother (not just physically) when it comes to pregnancy after loss.
I am so sorry for your loss. Thank you for so openly sharing yours and Wilder’s journey; it will help others.
Hi my name is Elizabeth from South Africa, I had the worst experience as a first time Mom, on the 21september 2019 I was suppose to get induced as I was 42 weeks and baby was not ready to come, when I went into hospital for my induction I was told I wait 3 more days I was booked in hospital to stay in as they don’t take walk in emergency, I stayed and 3 days later it’s was my induction day they booked me in a room they gave me a pill to take , this was around 9:00am by 18:00pm I was bleeding but the baby have not moved he was just sitting at 2cm, by 2 am the next day the doctor decided to break my water I didn’t know better, the baby’s heart was beating fine everything was fine by 4am the baby was still on 2cm I was bleeding my doctor kept telling me”this is normal don’t worry”, I was worried I wasn’t suppose to be bleeding so much i didn’t have any strength left in me I was begging the doctor’s to give me a C-section they told me “No, I’ll be fine stop being weak”, by 6am I was disoriented my water had been leaking all this time I was still bleeding one of the senior doctors came into my room and said “we should take you to the theatre for a C-section” I was praying to God the pain was finally going to be over I will see my boy, but I was sitting there until 8:30am second senior doctor came in and told me “C-section” but no one moved me all doctors and nurses disappeared from my room , by 10:30 I felt the baby’s head pushing down I couldn’t breath I couldn’t push, I had no strength they told me to push which I did with all the strength I had left , when they realized his head was still to far and he was bridging it was too late his heart had stopped. I was able to push him out and give birth to him by 11:30 on the 25th September 2019, they had cut me so badly during the birth process I needed surgery to repair the damage they’ve made, I lost so much blood through out this process. Until today I have nightmares about that day , I can’t sleep without waking up in tears
Dear Elizabeth,
I am so dreadfully sorry for the nightmare that you have endured and for the loss of your beloved baby boy. It has not even been a year and the anguish that you feel, I can also feel with much sharp pain. You tried so hard. I hope so much that you have some loving family or friends around you, to support you in your grief and to share your tears and hold you. Just after I learned that my son Wilder had died, but before I gave birth to him (a period of nearly two days), I got up in the middle of the night because I could not sleep, I went into my mother’s bedroom, and I climbed into bed with her, and she just held me and tried to comfort me as she had when I was little. While it never made the sorrow and grief go away, it did soothe me. I wish for you that the passage of time will be soothing in some small way. Sending you strength and courage,
Susannah
Excellent. Very accurate and honest. Should help others going through the same thing.