David Crowe shares his experience of living with sleep apnoea and exploring treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes. options.
Page last updated: 12 November 2021 and last checked 15 March 2023.
We know the importance of sleep, even if we don’t always allow ourselves the luxury of eight hours, but what happens if we have slept eight, nine, or ten hours and still feel absolutely shattered when we wake up? This was my experience around eight years ago, around the time I turned 50; waking up exhausted, dreading doing the work I loved facilitating groups, running training and doing one-to-one work with people.
After musing about it for several months, (midlife crisis, chronicA health condition marked by long duration, by frequent recurrence over a long time, and often by slowly progressing seriousness. For example, rheumatoid arthritis. fatigue and other more serious alternatives all popped up in my consciousness) and like a lot of men with some reluctance to seek help, I went to the GP. I ended up in front of a Locum who told me I needed to lose weight and avoid stress, which I kind of knew and wasn’t a helpful consultation because it felt so literal. I did try to follow a regime with more exercise and less food, but because of waking up constantly tired, a lot of the time I reached for a quick hit of carbs and sugars. I went back to the GPs again and got to see my regular doctor and ended up going down the route of chronic fatigue syndrome (CFS) with a specialist referral, but over time this didn’t help and I was still very tired.
A while later my wife said to me one morning “I’m really struggling with your snoring; I haven’t wanted to tell you for a while, but it’s getting worse”. Given the possibility of having to move rooms, I was at the end of my tether with tiredness. I ended up doing lots of internet searches and came up with this strange condition called “OSA” (what I now know as obstructive sleep apnoea) where the walls of the throat relax and narrow during sleep, interrupting normal breathing. On further searching, it affects larger people with big necks (yes that’s me) and the effect of it is profound: the lack of oxygen triggers your brain to pull you out of deep sleep – either to a lighter sleep or to wakefulness – so your airway reopens and you can breathe normally. The result is that you spend the night constantly waking up or being in light sleep and exhausted the following day.
I ended up doing lots of research on OSA research studies on effective interventions through NICE and SIGN guidelines. I went back to the GP, and ended up going for a sleep studyAn investigation of a healthcare problem. There are different types of studies used to answer research questions, for example randomised controlled trials or observational studies. and was finally formally diagnosed with mild sleep apnoea. From looking at some of the different studies, 40% of the UK populationThe group of people being studied. Populations may be defined by any characteristics e.g. where they live, age group, certain diseases. snore, and there is an estimated 5% of the UK adult population thought to have undiagnosed OSA; over 2.5 million people. That is a lot of blighted lives when those people don’t even know the cause of their suffering, and even though more is known about it now than a decade ago, there is still a lot of work to do in both awareness of the condition and getting help.
Managing sleep apnoea
Once the sleep study had confirmed a diagnosis, the interventions were effectively threefold.
Continuous positive airway pressure (CPAP)
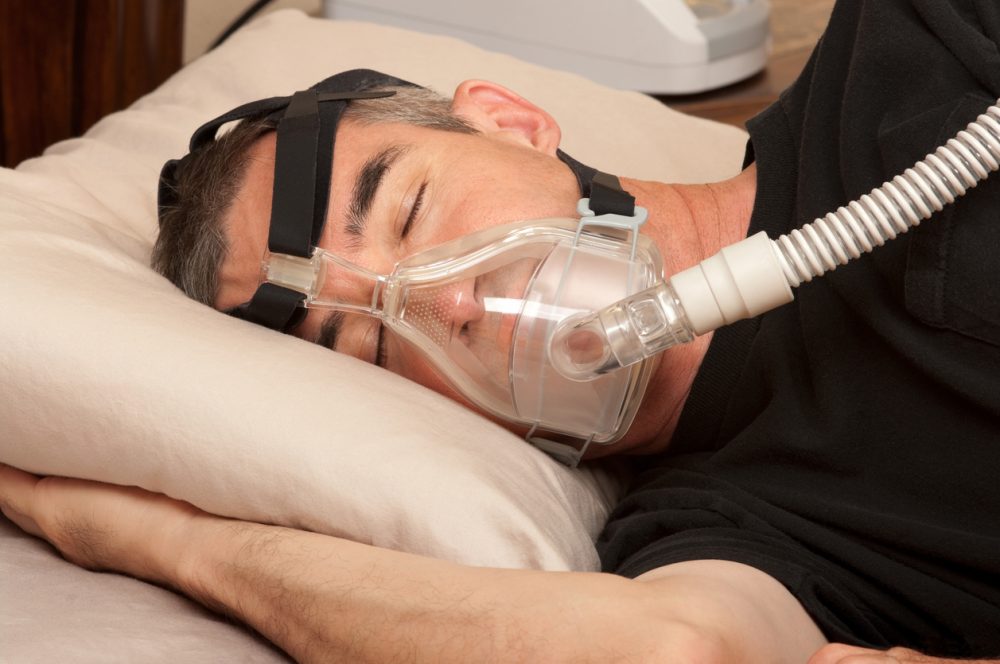
The current gold standardThe intervention that is widely accepted as being the best available, against which new developments should be compared. For example, a particular medicine. treatment is something called a CPAP machine (continuous positive airway pressure device) which prevents the airways in the throat from closing. A Cochrane Review on CPAP for OSA in adults, which has informed the NICE and SIGN guidelines, found that CPAP may reduce daytime sleepiness and improve quality of life in people with moderate and severe OSA.
I tried it for a few nights, but couldn’t stand the mask over my mouth and the noise of the pump; I understand there is quite a high rejection rateThe speed or frequency of occurrence of an event, usually expressed with respect to time. For instance, a mortality rate might be the number of deaths per year, per 100,000 people. of patients with OSA using these machines, though the job they do is really effective; it just didn’t work for me.
Another Cochrane Review looked at different ways of delivering CPAP. Whilst it doesn’t provide clear answers, the evidence suggests that nasal pillows or an oral mask may be useful for people who can’t tolerate conventional nasal masks.
Could anything have helped me to get used to CPAP? Maybe! A Cochrane Review looking at educational, supportive and behavioural interventions to improve use of CPAP machines (updated in April 2020) found these help people to use CPAP for longer, though whether this translates into less sleepiness and improved quality of life remains unclear.
Oral appliances
For people with a mild condition, there are things called mandibular advancement devices that are fitted by specialist dentists who take a mould of the upper and lower mandible and create acrylic devices that can be adjusted to move the lower mandible forward, so clearing the back of the throat to breathe. This is what I have ended up using for the last 8 years, with more than average success, though it has introduced me to a whole other world of charlatans and snake oil sellers of such devices in a pretty unregulated market, as well as solid and dependable dentists who are trying to come up with devices that work.
An interesting paradox of the NHS is that they are prepared to offer me maxillofacial surgery to move my lower mandible forward at the cost of several thousand pounds and a less than 50% chance of a successful outcomeOutcomes are measures of health (for example quality of life, pain, blood sugar levels) that can be used to assess the effectiveness and safety of a treatment or other intervention (for example a drug, surgery, or exercise). In research, the outcomes considered most important are ‘primary outcomes’ and those considered less important are ‘secondary outcomes’. due to age, but Clinical Commissioning Groups will not support the mandibular advancement device costs. It would be timely to have an update of the Cochrane Review on oral appliances for OSA which, back in 2006, highlighted increasing evidence that they improve sleepiness and sleep-disordered breathing.
A healthier lifestyle
Get fit, eat less and lose weight. So, the easy part…! With the ongoing tiredness I had struggled with keeping fit and losing weight and had strayed from a healthy regime, but I made a concerted effort which I have kept up to the present and will continue to do, of high-impact cardio exercise at least 3-4 times a week involving a combination of running, football (5 a side and walking football!) and spinning and keeping a food diary to watch the calorie intake. Like many people, there are recidivist gaps in the food diary when I forget or have a bad food day, but the discipline around eating and exercise keeps me on the straight and narrow of good health. And, a hard thing to do, I gave up alcohol, as it isn’t conducive to good sleep.
What are my overall reflections on dealing with sleep apnoea?
- I take some responsibility for not doing something sooner for sure. Perhaps in those middle years after my twenties and thirties when I played lots of sports I lost the habit of exercise and was much too work-focused. Health is now at the top of my priorities instead of work
- However, I do feel that I wasn’t properly supported by the GP practice, and ended up knowing a lot more than the average GP about sleep apnoea. I appreciate they have to have a handle on hundreds of conditions, but a more in-depth initial diagnosis and quicker specialist referral may well have got me to a resolution quicker
- An awareness that with a lot of conditions, there is a largely unregulated marketplace out there ready to take your money and not offer much in return. Like all commercial setups there are the basic mandibular advancement devices almost like “boil in the bag” type plastic that you then mould to your teeth for around £30-40 that don’t help much. I have ended up having to spend around £500 every 12-18 months for a fitted acrylic device, and have recently had a fitted metal device well over twice that price that ended up not working for me
- I would really like to see more contemporary research in this area, perhaps through an organisation like the James Lind Alliance working with patients and professionals to find out more about appropriate and evidence-based interventions
Editor’s note:
Readers may be interested to know that:
- A Cochrane Review on drugs for sleep apnoea has found insufficient evidence to support drug treatments.
- A Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. on the effects of pressure modification or humidification on CPAP usage (published in December 2019), concluded that “In adults with moderate to severe sleep apnoea starting positive airway pressure therapy, auto‐CPAP probably increases machine usage by about 13 minutes per night. The effects on daytime sleepiness scores with auto‐CPAP are not clinically meaningful… The evidence available for other pressure modification strategies does not provide a reliable basis on which to draw firm conclusions.”
- Another Cochrane Review has looked at Myofunctional therapy (oropharyngeal ‐ mouth and throat ‐ exercises) for people with OSA (published November 2020). Myofunctional therapy teaches people to do daily exercises to strengthen their tongue and throat muscles. The review authors found 9 studies with 347 people (mainly men) with OSA. The evidence suggests that, compared to sham therapy, myofunctional therapy probably reduces daytime sleepiness and may increase sleep quality in the short term in patients with OSA, but may have little or no effect on snoring frequency.
David Crowe has nothing to disclose.


I needed to know that mandibular advancement devices, which are fitted by trained dentists, are available for those with moderate conditions. You mentioned that they make acrylic devices that can be adjusted to shift the lower jaw forward, clearing the back of the throat to breathe, using molds of the top and lower mandibles. My best friend is bound to visit a sleep apnoea clinic soon after showing signs of this so I wish this can help her with the treatment after the diagnosis.
Hi David, what a great blog. Thanks for the insights – I read all the Airways reviews (as the managing editor) but these perspectives bring it to life. Jani I have been having my own experiences as a healthcare user: it seems that there is a lot for users to piece together in any area of healthcare.
I am trying to get the oral applicance review updated. Please get in touch if you have any wish to be involved as an author or in some other way. Any readers also welcome to get in touch! Wishing you all the best in finding something that works for you, Emma.
Hi David. I totally sympathize. It is the strangest feeling having to exhale against a constant airflow pushing back. I was told that SCUBA divers take to CPAP like fish to water. Which makes total sense. I guess I will have to try if SCUBA diving is now easy for me! It was interesting to see this one guy commenting on Twitter that he was looking for an alternative for CPAP because he hates it. I can’t say I’m overjoyed by having to use it. It is uncomfortable and inconvenient. Almost like wearing the Facehugger from Alien. But the effect is so clear and a massive improvement that I can’t imagine what alternative could come close even theoretically. There is an easy analogy: a turbo-charged engine. You get more horse power by forcing more air into the engine intake. There is no amount of exercise to boost the lungs or mandibular device that will fully take away the problem of airway constriction. CPAP does that and more. It forces the airways from relaxed/constricted to maximum capacity and pushes more content through. I hope it works for you too.
Hi Jani a really interesting perspective thanks for sharing.The “MAD” device as a mild OSA sufferer seems to work for me, but listening to what you said, I wonder if I might go back and try CPAP again as only tried for a few nights and really hated it; in all the reviews it is the gold standard for treatment. You too, and glad you have found a workable solution. My heart goes out to those who know they are constantly tired (and according to statistics there are thousands of them), but don’t know why
If you can do cardio, run and play football, I’m flabbergasted and saddened you received a diagnosis of Chronic Fatigue Syndrome (ME/CFS). Those patients get much sicker from even minimal physical or mental exertion (“post-exertional malaise”), and certainly don’t benefit from increasing exercise (in the US, the CDC no longer recommends graded exercise therapies for ME/CFS due to lack of effectiveness and potential for patient harm).
Uninformed doctors continue to conflate Chronic Fatigue and the systemic neuroimmune disease Chronic Fatigue Syndrome, resulting in both under and over diagnosis of ME/CFS, and consequently inappropriate treatment such as you experienced.
Hi John, just to clarify, I started the exercise regime after finally getting an OSA diagnosis. The points you make on conflating chronic fatigue well made
Hi David, you wrote a good and timely post. I wholeheartedly agree that we sleep apnoeists are mostly left alone to figure out our way out of the bog of constant drowsiness. I tried the mandibular advancement thing first but ended up with such fierce pains when the jaw joint started slowly moving out of its socket what with the heavy pulling going on. The next option I was offered was surgery. However, like with yourself, the main indication for which the procedure is used is to fix the non-alignment of teeth (and resulting havoc caused to teeth, headaches, etc.) and as such there was no guarantee of success with OSA. So I said no thanks and let’s try CPAP. Thankfully the nurse instructing me on how to use the infernal contraption said I’m not allowed to bring it back without having tried it for a minimum of two weeks. The first three nights were hell. But then it got slowly better and better. Now I’ve used the thing for three years now and recommend it to everyone. Everywhere I travel, I carry the CPAP machine with me. However, I had to figure out myself that the machine on itself doesn’t work unless I use medication to ensure adequate airflow through the nose. That’s why it was so awful to begin with as the machine furiously tried to inflate me like a balloon through severely blocked nasal passages. So my recommendation is to use CPAP combined with the right pharmaceuticals. Sweet dreams dude!