In a blog for those supporting older people who are on multiple medications, including relatives, carers and health professionals, Sarah Chapman looks at new Cochrane evidenceCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. on approaches to help them take them as prescribed and also considers the importance of ‘careful and kind care’.
Page last checked 26 June 2023.
Take-home points
As my mum declined with dementia, keeping on top of taking her medicines as prescribed was something that cost her a good deal of effort and us some worry. We were urged to get her to use a seven-day pill dispenser box, but Mum rejected that in favour of keeping on with her long-established system, putting pills into egg cups and upending the cups when she’d taken them. It worked for her, for a good while. Then, after a brief, unsuccessful spell with a pill box, the task overwhelmed her, and it was one of the first things to be taken over by visiting carers. I wonder now if my mum, ever gracious and grateful for any help provided, minded the loss of control over this activity, another bit of her independence chipped away; or perhaps she was relieved not to be responsible for it any more.
Taking medicines as prescribed is important if they are to be effective and also safe. However, incorrect use – whether deliberate or unintentional – is a very common problem, particularly (though not exclusively) among older people, as I’ve discussed in this earlier blog where I looked at multiple Cochrane Reviews on strategies to improve medication adherence. People who are prescribed self-administered medication typically take around half of their prescribed doses and may stop treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes. early (Nieuwlaat, 2014). They may take too much or too little, take it at the wrong times or in the wrong way. The consequences include health problems and wasted resources, such as hospital visits and prescriptions that could otherwise have been avoided, and unused medicines that get thrown away.
Self-administering multiple medications and following a treatment plan, with obstacles presented by physical and cognitive problems, is hard work. It’s no wonder many people become overwhelmed by it. What can help them manage it?
Cochrane evidence on helping older people take medication correctly
A new Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. was published this month, pulling together the best available research evidence on medication-taking ability and adherence in older adults prescribed multiple medications.
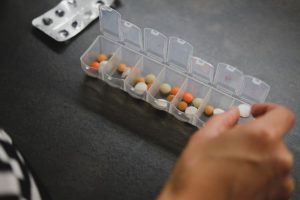
The review authors were able to include 50 studies with over 14,000 older people (most aged 65 and older), all comparing interventions intended to help them take their medication as prescribed with ‘usual care’, while six also compared interventions with each other. Interventions were grouped according to whether they had educational components only, behavioural components only, or both. Educational interventions included giving people information about their medication or a health professional reviewing their treatment regime. Behavioural interventions were things like text reminders or the use of multi-compartment pill boxes.
What did they find?
The studies had problems in how they were done and also varied in important ways, such as what the interventions were and how or when medication adherence or medication-taking ability was measured. This review highlights the lack of high-certaintyThe certainty (or quality) of evidence is the extent to which we can be confident that what the research tells us about a particular treatment effect is likely to be accurate. Concerns about factors such as bias can reduce the certainty of the evidence. Evidence may be of high certainty; moderate certainty; low certainty or very-low certainty. Cochrane has adopted the GRADE approach (Grading of Recommendations Assessment, Development and Evaluation) for assessing certainty (or quality) of evidence. Find out more here: https://training.cochrane.org/grade-approach, reliable evidence. The results are likely to change if more and better studies can be added later on.
Medication-taking ability
This is used here to mean a person’s ability to accurately follow a prescribed medication regimen, including knowing what to take, when to take it and being able to carry that out. The review authors were unable to determine the effects of interventions on medication-taking ability, with low-certainty evidence from just five studies, each measuring it in a different way.
Medication adherence
This refers here to the extent to which a person’s medication-taking behaviour aligns with the agreed-upon treatment recommendations from a healthcare provider. Most of the studies looked at this.
They found that, compared with usual care, interventions using behavioural or mixed (educational and behavioural) strategies may increase the proportion of people who are adherent. The effects of education-only interventions are uncertain.
Have interventions been shown to make a difference in other ways?
Mixed interventions may reduce the number of emergency department visits or hospital admissions but may have little or no effect on health‐related quality of life. Educational interventions probably have no effect on these things, while the effects of behavioural interventions remain uncertain.
How do the interventions compare with each other?
Very few studies made head-to-head comparisons between different interventions and the review authors were not able to draw conclusions about these.
Something else to think about – careful and kind care
I hope that better evidence will become available and that this will guide healthcare providers and others supporting older people in working out how they might best help them manage their medications. But I am thinking too about the words of Victor Montori, Professor of Medicine at the Mayo Clinic in the US and proponent of ‘careful and kind care’. He said that evidence is one of the tools that helps us get care right but not the first thing we should think about. Rather, we should start with the problems of the patient, THIS patient, not patients like him or her. He talks about the importance of clinicians caring, rather than providing care, considering the circumstances of the individual, their ‘biology and biography’, making shared decisions with them about the way forward, things that make sense to them intellectually, emotionally and practically. This kind care, centred on the individual, is at the heart of the Patient Revolution – you can read more about it here.
I’m remembering too what Victor Montori has to say about Maria Luisa, an elderly woman with multiple health problems, on multiple medications and other treatments for them. She is struggling with it all. He describes her as being overwhelmed, not just by her health problems but by her health care.

He says, “in the case of Maria Luisa, we wouldn’t be calling her ‘non-compliant’. We would be describing her situation as one in which what we’ve been asking her to do has exceeded her capacity to do it. An imbalance of workload and capacity…. In kind care, we recognise that the patient’s most precious resource is their time, their energy and their attention and we don’t waste that. We try to boost the possibility of that capacity so not only do they have more capacity to do more health care, but they have more capacity to do more life.”
Wise words. I remember Mum and her egg cups too. The multi-compartment pill box (a behavioural interventionA treatment, procedure or programme of health care that has the potential to change the course of events of a healthcare condition. Examples include a drug, surgery, exercise or counselling. in some of these studies) made sense to the person urging us that Mum should use one, and according to the evidence in this review, it may increase the likelihood that people like her adhere to their medication regimes. But it didn’t make sense to Mum. It comes back to those three pillars of evidence-based practice – the best available evidence, clinical judgement, and the patient’s preferences and values. Evidence can help, but don’t let’s lose sight of the individual.
Join in the conversation on Twitter with @CochraneUK @SarahChapman30 @CochraneCCRG or leave a comment on the blog. Please note, we cannot give medical advice and we will not publish comments that link to commercial sites or appear to endorse commercial products.
Sarah Chapman has nothing to disclose.



