In this blog for people with endometriosis, Dr Mathew Leonardi, Surgeon and Sonologist at McMaster University and Dr James Duffy, Clinical Fellow at King’s Fertility, discuss the latest Cochrane evidenceCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. on the use of ultrasound to diagnose endometriosis. They both reflect on the current research evidence, latest developments in the use of ultrasound in the diagnosis of endometriosis, and how the effective use of ultrasound could reduce delays in diagnosis. This blog is the third in our #MyEndometriosisQuestion series running throughout March, with blogs about endometriosis and an invitation to ask your questions, which will be addressed by a panel of experts. More details at the end of this blog.
Featured image: ‘Half My Life’ by Margaret Kalms* https://www.artofwoman.com.au “This woman had bleeding for 2 weeks each month. That is half her life”.
Page last checked: 30 June 2023.

What is endometriosis?

How is endometriosis currently diagnosed?
Diagnosing endometriosis is a critical step in ensuring people receive appropriate treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes.. In a previous blog, ‘Blood tests for diagnosing endometriosis: the latest evidence’ you can read about some of the symptoms of endometriosis and what your first steps might be in consulting your GP.
Ultrasound scan: the first test for diagnosing endometriosis
The National Institute for Health and Care Excellence produce evidence-based guidance and advice for health professionals. The current NICE guidelines for endometriosis recommend people with symptoms suggestive of endometriosis should be examined by an experienced healthcare professional and offered a transvaginal ultrasound scan.
A transvaginal ultrasound scan is a safe and straightforward procedure that uses ultrasound waves to produce images of the womb (uterus), fallopian tubes, ovaries, and in centres specialising in endometriosis, other structures including the bladder and bowels. During the ultrasound scan, you will be asked to lie on your back. A small ultrasound probe with a sterile cover, not much wider than a finger, is then gently passed into the vagina. Many people describe the transvaginal ultrasound scan as uncomfortable, though not painful. If a person has symptoms of endometriosis, sometimes the scan can be described as painful.
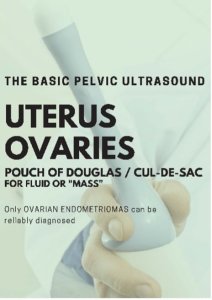
Some people decline a transvaginal ultrasound as they feel uncomfortable. It is important to know this is completely OK and there are alternative options including a transrectal ultrasound, MRI scan, or keyhole surgery.
Diagnosing endometriosis in different areas of the body
Endometriosis is most commonly found inside the pelvis, on the surface of the womb (uterus), around the fallopian tubes, inside the ovaries, and in an area between your womb and the rectum (part of the bowel). In rare cases, endometriosis has been found in other parts of the body including the brain, lungs, and spine.
The three most common types of endometriosis are: superficial endometriosis, ovarian endometriosis, and deep endometriosis (also known as deeply infiltrating endometriosis).
Superficial endometriosis
Superficial endometriosis deposits are located on the surface of pelvic organs, for example the surface of the womb, and are usually on a few millimetres wide and few millimetres deep. It is the most common type of endometriosis and is difficult to diagnose accurately using transvaginal ultrasound or other imaging tests.
Ovarian endometriosis
Endometriosis can cause an ovarian cyst when endometriosis grows in the ovary, which are called endometriomas. They are sometimes known as chocolate cysts because they have a melted chocolate appearance.

Deep endometriosis or deeply infiltrating endometriosis
Deep endometriosis generally invades structures within the pelvis including the bowels, bladder, or ligaments. Often, this type of endometriosis leads to substantial scarring between the womb and the bowel which is known as “obliteration of the pouch of Douglas” (also known as “cul-de-sac” or “rectouterine pouch”).
When all three types are combined, they often referred to by gynaecologists as overall pelvic endometriosis.
International experts in the ultrasound diagnosis of endometriosis
There is a vibrant online community of healthcare professionals who share knowledge of diagnosing endometriosis using ultrasound you may want to look at their Twitter pages: Prof George Condous (@GeorgeCondous), Dr Susanne Johnson (@GynaecologyUS) and Joel Naftalin (@JoelNaftalin).
Is a transvaginal ultrasound scan accurate in diagnosing endometriosis?
In the Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research., Imaging modalities for the non‐invasive diagnosis of endometriosis (February 2016), Vicki Nisenblat and colleagues brought together the evidence from all published research studies evaluating the accuracy of transvaginal ultrasound in diagnosing endometriosis. They included research studies which evaluated transvaginal ultrasound as a replacement test for keyhole surgery. They included:
- Five studies, which included a total of 1222 people with suspected endometriosis, evaluated the accuracy of transvaginal ultrasound in diagnosing superficial endometriosis.
- Eight studies, which included a total of 765 people with suspected endometriosis, evaluated the diagnostic accuracy of transvaginal ultrasound in diagnosing ovarian endometriosis.
- Nine studies, which included a total of 934 participants with suspected endometriosis, evaluated the diagnostic accuracy of transvaginal ultrasound in diagnosing deep infiltrating endometriosis.
The researchers concluded that people with pain symptoms suggestive of endometriosis with evidence of endometriosis identified during a transvaginal ultrasound scan were likely to have endometriosis. Unfortunately, a negative transvaginal ultrasound scan did not exclude the possibility of endometriosis and these people will require further investigation.
The researchers commented on the low quality of the published research, for example, significant differences in the people included in the research studies, the use of older ultrasound machines, and limitations in the expertise of the individuals performing the ultrasound scans. These factors made it difficult to draw any firm conclusions about the accuracy of transvaginal ultrasound scan to diagnose endometriosis.
Looking ahead
Transvaginal ultrasound is more than just a diagnostic test. It is a test that can help patients and their doctors understand the severity of endometriosis. In our opinion, when an ultrasound is performed by a colleague who has received high-quality training in the diagnosis of endometriosis, and it is normal, this does not mean there is no endometriosis. In fact, many people with the classic symptoms of endometriosis and a normal scan do have superficial endometriosis. What this ultrasound result tells us is that there is no ovarian endometriosis or deeply infiltrating endometriosis, which is important to know when thinking about treatment options.
On the other hand, when we see endometriosis on ultrasound and can tell that it is ovarian endometriosis or deeply infiltrating endometriosis, this eliminates the need to perform keyhole surgery for diagnosis. The knowledge of severe endometriosis can help a person with endometriosis find an accredited endometriosis centre. In the UK, the British Society for Gynaecological Endoscopy (BSGE) maintains a list of accredited endometriosis centres.
In time, our hope is that all people with symptoms suggestive of endometriosis can access high-quality transvaginal ultrasound by healthcare professionals trained to look for and see endometriosis. When this happens, the keyhole surgery for diagnosis will become a thing of the past. We believe that no person should have to undergo a surgical procedure to receive an endometriosis diagnosis. Finding ultrasound techniques and new bloods tests should help tackle delays in diagnosis.
Until then, as gynaecologists, we recommend that people with symptoms of possible endometriosis should advocate for themselves to have an ultrasound scan performed by a colleague who has undertaken specialised training in endometriosis diagnosis. This advocacy should motivate all colleagues who perform transvaginal ultrasound to learn the necessary skills to provide the required specialised diagnostic service.
Questions to ask your gynaecologist
- What is the most likely cause of my symptoms?
- What could be the other causes of my symptoms?
- Will the ultrasound look for deep endometriosis and adhesions outside of my uterus and ovaries?
- Please explain my transvaginal ultrasound result. Were any causes of pelvic pain identified?
- If endometriosis has been identified, what are my holistic, medical, and surgical treatment options?
- If endometriosis has not been identified what other diagnostic tests can I be offered?
- What are the alternatives to transvaginal ultrasound?
Support for people with endometriosis
There is a vibrant online community of women with endometriosis, commonly known as #endosisters, who share knowledge and offer support, along with charities such as Endometriosis UK and grassroots organisations such as Fair Treatment for the Women of Wales.
More about #MyEndometriosisQuestion – and ask yours
You can find out more in the blog Endometriosis: #MyEndometriosisQuestion – a special series, including how to ask your question on our social media platforms, or you can post your question below this blog. While our experts cannot give specific medical advice, they can provide information about endometriosis, relevant evidence and guidelines, and tips for discussing endometriosis with your own health professional. Our expert panel will do their best to answer your questions individually. They will also reflect on some of the submitted questions in a blog to be published at the end of the month. No individuals will be named or identified in this blog.
Further information about endometriosis
- Cochrane Gynaecology and Fertility: Endometriosis Awareness Month
- Endometriosis UK
- King’s Fertility: What is endometriosis?
- The British Society for Gynaecological Endoscopy (BGSE) maintains a list of accredited endometriosis centres.
- Read the rest of the blogs in this series: #MyEndometriosisQuestion
Join in the conversation on Twitter with @MathewLeonardi @JamesMNDuffy @CochraneUK and @CochraneCGF or leave a comment on the blog. Comments are checked by the Editors before they are made public on the blog.
Please note, we cannot give specific medical advice and do not publish comments that link to individual pages requesting donations or to commercial sites, or appear to endorse commercial products. We welcome diverse views and encourage discussion but we ask that comments are respectful and reserve the right to not publish any we consider offensive. Cochrane UK does not fact check – or endorse – readers’ comments, including any treatments mentioned.
References and further reading (pdf)
*Featured image used with permission and cannot be reused without permission from the artist.
Disclosure of interest: Dr Leonardi reports grants from AbbVie, grants from Australian Women and Children’s Foundation, personal fees from GE Healthcare, personal fees from TerSera, outside of the submitted work. Dr Duffy has nothing to disclose.

Mathew Leonardi’s biography appears below.


I am so saddened by the disrespect shown to women by changing the language and failing to use the term woman in this article. I will be unsubscribing and shan’t be looking at your evidence again. Perhaps you will appeal to three people by taking the “woke” route, but you are disempowering a majority, who are already much disrespected by many in your profession. Are your colleagues in men’s health referring to “people assigned male at birth”? This feels sexist and about rendering women invisible.
Hello Becks,
We are sorry to read that you feel our choice of language is disrespectful – that is not our intention, but rather to show respect, and indeed potentially empower, everyone who comes to these blogs.
Throughout this series, we are using inclusive language (‘people with endometriosis’). This is in recognition that people who do not identify as female can also be affected by endometriosis. Referring to endometriosis as only a ‘women’s problem’ can make things even more difficult for those who do not identify as female, in terms of seeking information and accessing health and support services.
Cochrane is an inclusive organisation and using more inclusive language is something for us as an organisation to consider as a means of demonstrating that and, importantly, championing equity in health care. All of our bloggers are dedicated to raising awareness of endometriosis, and campaigning for more effective and timely diagnosis and treatment, for everyone affected.
Best wishes
Sarah Chapman and Selena Ryan-Vig [Editors]
Thanks for clarifying your position. I am glad to know that, and will send the women in my care elsewhere for information in the future, as many of them have communicated with myself and colleagues that they find so-called inclusive language to be disrespectful. Whether it is your intention or not, it is seen by many as an attempt to render women less important than those who have female bodies but do not want to acknowledge this fact.