Sarah Chapman gives a round-up of evidence on venous leg ulcers, for nurses, including Cochrane ReviewsCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research., NICE guidance and Medtech innovation briefings, research priorities and more.
This content replaces an earlier article by Sarah Chapman, written for the British Journal of Community Nursing and also posted here in 2017.
Page updated on 1 August 2023 with new evidence on endovenous ablation.
Venous leg ulcers are common
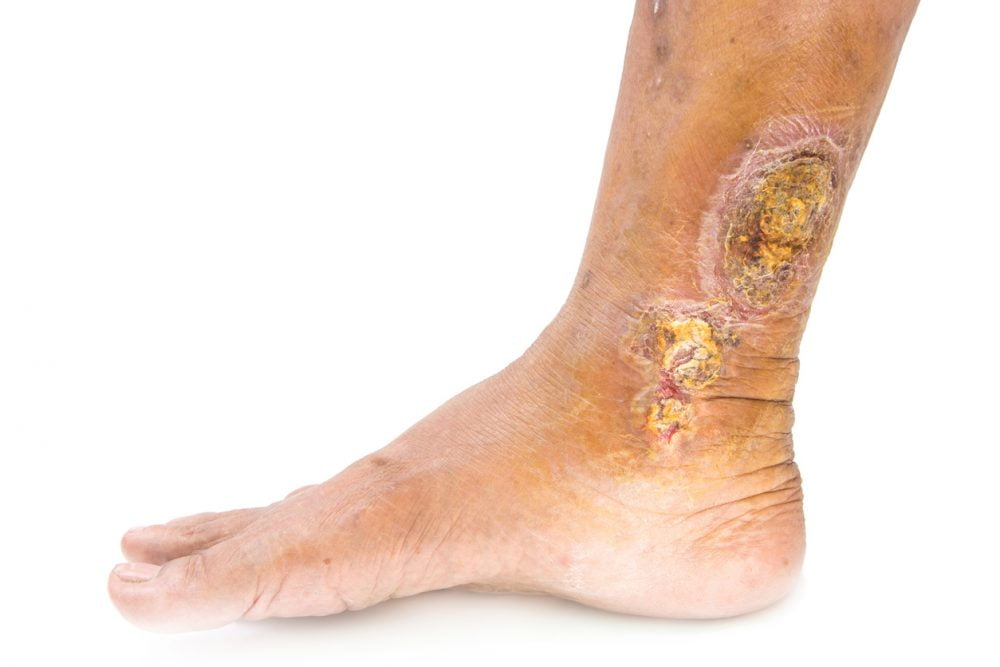
Venous leg ulcers (VLUs) are chronicA health condition marked by long duration, by frequent recurrence over a long time, and often by slowly progressing seriousness. For example, rheumatoid arthritis. wounds, caused by venous insufficiency. They are the most common type of leg ulcer. They most often occur in the gaiter region of the lower leg, from just below the ankle up to mid-calf. They are defined as any break in the skin that has been present for at least six weeks or occurs in someone with a previous history of venous leg ulceration. In their Clinical Knowledge Summary Leg ulcer – venous The National Institute for Health and Care Excellence (NICE) give an estimated prevalenceThe proportion of a population who have a particular condition or characteristic. For example, the percentage of people in a city with a particular disease, or who smoke. of venous leg ulcers in the UK of between 0.1% – 0.3% and this increases with age.
According to NICE, six-month healing rates have been reported as 45% for people treated in the community, and 70% for people treated in specialist clinics. Repeated cycles of ulceration, healing and recurrence are common. Twelve-month recurrence rates range between 26–69%.
Venous leg ulcers are painful, distressing and affect quality of life
Venous leg ulcers are painful, distressing and have a considerable impact on quality of life. Research into how pain can be better controlled in people with venous leg ulcers, and how quicker healing can be promoted, were among the Venous Top 10 Priorities identified by the NIHR James Lind Alliance Priority Setting Partnership Vascular conditions in 2021, while the Wounds Top 10 included questions about how to improve quality of life and about the best way to manage complex, hard to heal, leg ulcers.
Treatments for venous leg ulcers
Cleansing
Wound cleansing is an integral part of managing venous ulcers, recommended in many international guidelines, but it is unclear which is the best method or solution.
The Cochrane Review Wound cleansing for treating venous leg ulcers (published March 2021) was able to include just four studies with 254 people, comparing different cleaning solutions. It highlights an evidence gap, with insufficient evidence to guide decision-making about the effectivenessThe ability of an intervention (for example a drug, surgery, or exercise) to produce a desired effect, such as reduce symptoms. of wound cleansing compared with no cleansing and the best approaches to cleansing of venous leg ulcers.
Prontosan
Prontosan is available as a solution, a gel and an extra thick gel. The solution is used for rinsing and soaking wounds and can be used alone or with one of the gels – applied after soaking and left in place until the next dressing change.
NICE Medical technologies guidance Prontosan for treating acute and chronic wounds states that “There is some evidence that it is clinically effective but not enough to recommend it for routine use” and recommends more research on the effectiveness of Prontosan compared with saline or water in chronic wounds of different types.
Debridement
Debridement, removing dead or dying tissue from the surface of a wound, is a component of standard wound care management as described in NICE guidelines and there is consensus in the wound care literature that it is necessary to promote healing.
There are six methods of debridement: using an instrument such as a scalpel (surgical or sharp debridement, with or without anaesthesia respectively); washing solutions and dressings (mechanical debridement); maggots (biosurgical debridement); enzymes to break down tissue (enzymatic debridement); and moist dressings and natural agents or both, to stimulate the wound’s own healing processes (autolytic debridement).
The Cochrane Review Debridement for venous leg ulcers (published September 2015) looked at the impact of debridement on venous ulcer healing and the comparative effectiveness of different methods. Although ten small RCTs were included, no meta-analysis was possible and the review authors concluded “There is limited evidence to suggest that actively debriding a venous leg ulcer has a clinically significantClinical significance is the practical importance of an effect (e.g. a reduction in symptoms); whether it has a real genuine, palpable, noticeable effect on daily life. It is not the same as statistical significance. For instance, showing that a drug lowered the heart rate by an average of 1 beat per minute would not be clinically significant, as it is unlikely to be a big enough effect to be important to patients and healthcare providers. impact on healing”.
Compression
Compression therapy, with bandages or stockings, promotes healing through aiding venous return and is the first-line treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes. for venous leg ulcers.
The authors of the Cochrane Review Compression bandages or stockings versus no compression for treating venous leg ulcers (published July 2021) conclude that, compared with no compression bandages or stockings, “If using compression bandages or stockings, people with venous leg ulcers probably experience complete wound healing more quickly, and more people have wounds completely healed. The use of compression bandages or stockings probably reduces pain and may improve disease‐specific quality of life. There is uncertainty about adverse effects, and cost effectiveness.”
There is a Cochrane Clinical Answer on this: “For people with venous leg ulcers, what are the effects of compression bandages?”
Dressings and topical agents
Dressings are usually applied to open ulcers. As well as offering protection, dressings may be chosen for other reasons, such as antimicrobial properties or absorption of exudate. As well as a wide range of types of dressings available, there are a number of topical products, used to reduce infection riskA way of expressing the chance of an event taking place, expressed as the number of events divided by the total number of observations or people. It can be stated as ‘the chance of falling were one in four’ (1/4 = 25%). This measure is good no matter the incidence of events i.e. common or infrequent., aid exudate absorption or promote wound healing by other means, as well as topical painkilling agents. Having reliable evidence to guide choices is important.
The authors of the Cochrane Review Dressings and topical agents for treating venous leg ulcers (published June 2018) conducted a network meta-analysisThe use of statistical techniques in a systematic review to combine the results of included studies. Sometimes misused as a synonym for systematic reviews, where the review includes a meta-analysis. (NMA) on dataData is the information collected through research. from 59 of the 78 studies included in the review (you can read more about NMA and the review on dressings and topical treatments for pressure ulcers in the blog Dressings and topical agents for healing pressure ulcers: which should we choose?). Unfortunately, it highlights continued uncertainty about whether particular dressings or topical agents improve the likelihood of healing. You can listen to a Cochrane podcast about this review.
More recently, the Cochrane Review Hydrogel dressings for venous leg ulcers (published August 2022) found “inconclusive evidence to determine the effectiveness of hydrogel dressings compared with gauze and saline, alginate dressing, manuka honey or hydrocolloid on venous leg ulcer healing”.
NICE has found that there is evidence to support the use of UrgoStart dressings to treat venous leg ulcers (and diabetic foot ulcers), as “they are associated with increased wound healing compared with non-interactive dressings”. In Manchester, nurses used this guidance to introduce a new pathway for the management of venous leg ulcers, using UrgoStart dressings, and this example was highly commended in the Shared Learning Awards 2020.
Protease-modulating matrix (PMM) treatments
It has been suggested that one cause of non-healing, or delayed healing, of chronic ulcers is prolonged high concentrations of proteases (enzymes that break down proteins into peptides and amino acids) in the wound. Protease modulating treatments (PMM) treatments aim to aid healing by modulating protease activity.
The authors of the Cochrane Review Protease activity as a prognostic factor for wound healing in venous leg ulcers (published September 2018) found “very low validity evidence regarding any associationA relationship between two characteristics, such that as one changes, the other changes in a predictable way. For example, statistics demonstrate that there is an association between smoking and lung cancer. In a positive association, one quantity increases as the other one increases (as with smoking and lung cancer). In a negative association, an increase in one quantity corresponds to a decrease in the other. Association does not necessarily mean that one thing causes the other. between protease activity and VLU healing and there is complete uncertainty regarding the relationship.”
The authors of the Cochrane Review A ‘test and treat’ strategy for elevated wound protease activity for healing in venous leg ulcers (published January 2016) found that there is no evidence from randomized trialsClinical trials are research studies involving people who use healthcare services. They often compare a new or different treatment with the best treatment currently available. This is to test whether the new or different treatment is safe, effective and any better than what is currently used. No matter how promising a new treatment may appear during tests in a laboratory, it must go through clinical trials before its benefits and risks can really be known. on the effectiveness of a ‘test and treat’ strategy, a test to detect high levels of protease activity followed by protease-modulating treatments for ulcers with high levels, on venous leg ulcer healing.
There is a lack of clarity in the literature about what constitutes a PMM treatment. The treatments investigated in the 12 studies included in the Cochrane Review on Protease-modulating matrix treatments for healing venous leg ulcers (published December 2016) were all dressings. The evidence is low certainty and the review authors conclude that uncertainty remains about the benefits and harms of PMM dressings compared with non-PMM dressings, and about differences in resource use and total costs.
Antimicrobial prescribing for leg ulcer infection
NICE guidance on Leg ulcer infection: antimicrobial prescribing (published February 2020) includes a two page visual summary of recommendations including tables to support prescribing decisions.
It points out that while most leg ulcers are colonised by bacteria, few are clinically infected, and that antibiotics don’t promote healing when a leg ulcer is not clinically infected.
Other drug treatments
Oral aspirin
A Cochrane Review Oral aspirin for treating venous leg ulcers (published February 2016) found insufficient evidence to draw firm conclusions about the possible benefits and harms of aspirin on the healing and recurrence of venous leg ulcers. Since then, a Phase II pilot randomised trial (AVURT) (published July 2019) has found no evidence that aspirin is effective in promoting venous leg ulcer healing, but the authors note their analysis was underpowered due to low recruitment.
Sulodexide
Sulodexide, a highly purified glucosaminoglycan, has been proposed as an adjunctive treatment for venous leg ulcers, as it is claimed to have anti-thrombotic, profibrinolytic and anti-inflammatory effects. Given orally or parenterally, it is mostly given to people with thrombotic risk diseases. The Cochrane Review Sulodexide for treating venous leg ulcers (published June 2016) found only low certainty evidence that it may increase venous ulcer healing, used along with local wound care. The route, frequency and dosage of sulodexide were poorly reported and it is unclear whether it is associated with adverse effects.
Endovenous ablation (using heat or medication to permanently close veins) for treating venous leg ulcers
Endovenous ablation is a minimally‐invasive technique that treats venous disease by blocking certain veins. Medication is injected into the vein, or a device is inserted into the vein and then heated up to permanently close it. Endovenous ablation combined with compression therapy aims to further reduce pressure in the veins of the leg, which may impact ulcer healing.
The Cochrane Review Endovenous ablation for venous leg ulcers (July 2023) has high-certaintyThe certainty (or quality) of evidence is the extent to which we can be confident that what the research tells us about a particular treatment effect is likely to be accurate. Concerns about factors such as bias can reduce the certainty of the evidence. Evidence may be of high certainty; moderate certainty; low certainty or very-low certainty. Cochrane has adopted the GRADE approach (Grading of Recommendations Assessment, Development and Evaluation) for assessing certainty (or quality) of evidence. Find out more here: https://training.cochrane.org/grade-approach evidence that endovenous ablation and compression together reduce time to complete ulcer healing compared with compression alone. There is also evidence that endovenous treatment and compression together probably increase the proportion of ulcers healed at 90 days, but may not change ulcer recurrence or the number of ulcer‐free days at one year.
Other treatments for venous leg ulcers
Cochrane Reviews of several other treatments have highlighted large gaps in the evidence.
The Cochrane Review Therapeutic ultrasound for venous leg ulcers (published May 2017) found that it is unclear whether therapeutic ultrasound improves ulcer healing and the review authors say that any effect is likely to be small. There is a Cochrane Clinical Answer on this review: “For people with venous leg ulcers, how does therapeutic ultrasound affect outcomes?”
The authors of the Cochrane Review Electromagnetic therapy for treating venous leg ulcers (published July 2015) concluded that “It is not clear whether electromagnetic therapy influences the rateThe speed or frequency of occurrence of an event, usually expressed with respect to time. For instance, a mortality rate might be the number of deaths per year, per 100,000 people. of healing of venous leg ulcers”.
The role of Subfascial endoscopic perforator surgery (SEPS) for treating venous leg ulcers (March 2019) also remains uncertain.
There were no randomisedRandomization is the process of randomly dividing into groups the people taking part in a trial. One group (the intervention group) will be given the intervention being tested (for example a drug, surgery, or exercise) and compared with a group which does not receive the intervention (the control group). trials meeting the criteria for inclusion in the Cochrane Review Extracorporeal shock wave therapy for the healing and management of venous leg ulcers (published June 2018).
For ulcers caused by varicose veins
A UK multi-centre randomised controlled trial, EVRA, found that “For patients with leg ulcers caused by varicose veins, early interventionA treatment, procedure or programme of health care that has the potential to change the course of events of a healthcare condition. Examples include a drug, surgery, exercise or counselling. to treat the veins results in faster healing of ulcers than standard compression therapy alone” (July 2018). It also “increases ulcer-free time and is highly likely to be cost-effective”.
NICE Medtech innovation briefings
Advice from NICE on several treatments for venous leg ulcers can be found in their Medtech innovation briefings (MIBs). These are designed to support NHS and social care commissioners and staff who are considering using new medical devices and other medical or diagnostic technologies. There are MIBs on:
Granulox for managing chronic non-healing wounds
WoundExpress to manage lower leg wounds
Join in the conversation on Twitter with @SarahChapman30 @CochraneUK and @CochraneWounds or leave a comment on the blog.
Please note, we cannot give specific medical advice and do not publish comments that link to individual pages requesting donations or to commercial sites, or appear to endorse commercial products. We welcome diverse views and encourage discussion but we ask that comments are respectful and reserve the right to not publish any we consider offensive. Cochrane UK does not fact check – or endorse – readers’ comments, including any treatments mentioned.
Sarah Chapman has nothing to disclose.


cycloidal vibration (CV) therapy e.g. vibro-pulse?
[…] https://www.evidentlycochrane.net/venous-leg-ulcers-evidence/ […]
I am suffering from two calf leg ulcers and a foot ulcer for the last 15 months I’ve never had an infirmity in my life please help! Dan Graham
ran across this summary! Excellent
role of the lymphatics in VLU?
NIRFLI clearly shows lymphatic impairment in all VLU yet still don’t see mention in the discussion of VLU management
Thoughts?
Thank you, I’ve recently been searching for information approximately this subject for a while and
yours is the best I have discovered till now. But, what concerning the bottom line?
Are you positive in regards to the supply?
Not a word about hyperbaric oxygen therapy. Results are variable, but there is a possible role as adjunctive treatment. We need good RCTs comparing usual care vs usual care plus HOT.
Indeed, the authors of the Cochrane review on hyperbaric oxygen therapy for chronic wounds state that “There is a strong case for investigation of the effects of HBOT on chronic wounds due to venous disease, arterial disease and pressure damage, in large, rigorous randomised clinical trials.”
Sarah Chapman.
Another good and useful summary of the research evidence. I would probably quibble with the statement about VenUS IV that “However, the investigators caution that there is too little evidence to draw firm conclusions about relative effectiveness”. Not sure which bit of the results this relates to* – quite possibly the recurrence rates (where the statement is true as the comparison is not truly randomised as it depends who initially healed and then had the potential to recur). In terms of healing we are satisfied that there is probably no meaningful difference in healing rates but the stockings were more cost-effective.
*The HTA report for this trial covered several studies including the actual trial. We did some modelling of all the available compression and overall there is uncertainty about which compression system is best but within this trial we are content that the stockings are more cost-effective and similarly clinically effective.
Thank you Nicky, this is helpful.
Sarah