In this blog for anyone considering surgery to treat pain associated with endometriosis, Dr Martin Hirsch, Consultant Gynaecologist, and Claire Barker, who had keyhole surgery for endometriosis in 2015, explore the benefits and risks and discuss important aspects to consider when thinking about undergoing surgery.
This blog is the seventh in our #MyEndometriosisQuestion series running throughout March, with blogs about endometriosis and an invitation to ask your questions, which a panel of experts have been addressing throughout the month.
Featured image: ‘Bleeding Burns’ by Margaret Kalms* https://www.artofwoman.com.au
Page last checked 3 July 2023

What is endometriosis?

Diagnosing endometriosis
Diagnosing endometriosis promptly, and reducing the time to diagnosis, is essential so that those affected can access medical or surgical care that is appropriate for them, as soon as possible. This is a national priority identified by the recent All Party Parliamentary Group review on endometriosis care.
The imaging options to confirm diagnosis have variableA factor that differs among and between groups of people. Examples include people’s age, sex, depression score or smoking habits. accuracy and you can read more about the benefits and limitations of pre-operative imaging in this Evidently Cochrane blog Ultrasound for diagnosing endometriosis: the latest evidence.
Claire’s experience of getting a diagnosis
For Claire, this is an all too familiar story: “Since the onset of puberty I experienced extremely painful periods which had made living any kind of normal life extremely difficult. Being incapacitated for at least one week a month is extremely frustrating and debilitating.
Like many endometriosis sufferers I experienced a long diagnostic delay, and over the next decade I began to suffer an increasing number of symptoms such as bowel pain, shoulder pain, fatigue, and bloating. After being referred for testing to investigate these symptoms, an MRI scan detected a growth on my right ovary. I had an initial diagnostic keyhole surgery (laparoscopy), where I was diagnosed with stage four endometriosis; an explanation at last for years of suffering”.
Weighing up whether – and when – to treat endometriosis surgically
When using surgery to diagnose a condition there is a drive to treat abnormalities at the same time, commonly referred to as “see and treat”. However, there are important and complex considerations when weighing up whether to treat endometriosis surgically:
- Has the patient given informed consent relating to the risks and benefits of all procedures that might be undertaken?
- is the surgeon trained to diagnose and treat this form of endometriosis?
- is the hospital equipped with necessary staff?
- is it the correct treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes. for this patient?
After waiting so long for effective treatment, Claire found herself needing to wait even longer:
“My endometriosis was not treated at the time of this surgery, as the surgeon was not experienced in endometriosis care and did not feel confident to remove it. The disease was covering many of my internal organs including my bowel, bladder and diaphragm. With hindsight I am glad that the surgeon took the decision not to remove my endometriosis, as it enabled me to take my time in coming to terms with my diagnosis and to decide on a treatment pathway that was best suited to me and my goals”.
These are all common dilemmas faced as a result of the limited non-invasive diagnostic tests for people with endometriosis. While nobody wants to wait or have repeated surgery, NICE recommend that complex surgery for rectovaginal endometriosis like Claire’s be performed at a BSGE centre with experience.
Treatment options for pain associated with endometriosis
The treatment options for this non-cancerous gynaecological disease are commonly categorised as conservative (painkillers / alternative therapies), medical (hormonal treatments), or surgical excision or ablation (keyhole surgery). There are rare circumstances where surgery may be strongly recommended such as when the person has blockage to the kidneys or bowel. However, in the UK, for most people, all options are available depending on personal preference, following discussion of the risks and benefits of each.
The need for a surgical diagnosis requires a cautious approach because of the risks of surgery. Injuries, albeit rare, do still occur and the Royal College of Obstetricians and Gynaecologists (RCOG) quote a riskA way of expressing the chance of an event taking place, expressed as the number of events divided by the total number of observations or people. It can be stated as ‘the chance of falling were one in four’ (1/4 = 25%). This measure is good no matter the incidence of events i.e. common or infrequent. of three injuries per 1000 operations, with over 50% of all laparoscopic injuries occurring at the time of starting the surgery and entering the abdomen.
The National Institute for Health and Care Excellence produce evidence-based guidance and advice for health professionals. The endometriosis guideline supports the use of surgery for the treatment of endometriosis where medical treatments are not successful or not appropriate for patients, following discussion with an expert.
Sub-types of endometriosis
Pelvic endometriosis can be categorised into three distinct sub-types that cover the majority of disease seen by surgeons.
- Superficial / peritoneal endometriosis
- Ovarian endometriosis
- Deep endometriosis
These can occur in isolation or combination and the presence of bilateral ovarian endometriosis has high concurrence with deep endometriosis.
These disease sub-types are important to consider, as the risks and benefits of treatments vary significantly between them. When treating deep endometriosis behind the womb, there are greater risks of injuring the bowel. When treating endometriosis of the ovary, there are risks of reducing the function of the ovary and response to fertility medicines or treatment. The lowest surgical risks are considered with the treatment of superficial / peritoneal endometriosis, although no surgery is risk free.
Surgery in specialist endometriosis centres
Where surgery is recommended, keyhole surgery (otherwise known as laparoscopy) is preferred. This offers less pain, shorter length of hospital stay, quicker recovery and improved cosmetic appearance for patients compared with open surgery. With risks increasing with increasing disease severity, the British Society for Gynaecological Endoscopy (BSGE) established specialist endometriosis centres in 2007 to centralise the surgical care of people with severe endometriosis.
This progressive approach to delivering care ensures that these centres and surgeons work to meet pre-specified criteria to be eligible to deliver specialist surgical treatments to people with severe endometriosis. These include: a minimum number of procedures per year per surgeon, a dedicated nurse specialist, a named urological and colorectal colleague for surgical support, and an annual video assessment of their surgical practice. This rigorous governance structure ensures standards of clinical and surgical care are maintained through regular assessment.
The wait to see an expert at the BSGE specialist centre provided Claire with time to consider her options and process the diagnosis of stage 4 severe endometriosis:
“After processing my new diagnosis for several weeks, and doing some research (via some helpful friends in my local support group and the Endometriosis UK website), I decided to seek a referral to an endometriosis specialist BSGE centre, through my GP. As I live in Hertfordshire the nearest centre to myself at the time was in London.
I decided that surgery was the right path for me at this time for two reasons. Firstly, I felt that hormonal contraceptives were no longer providing adequate symptom relief for me, and so I was willing to try a more radical approach to alleviating my pain (you can read more about my experiences of using hormonal contraceptives for pain here). Secondly, I was hoping to try for a baby soon, and my endometriosis diagnosis had caused me to worry about my fertility. I hoped that having the keyhole surgery (laparoscopy) would improve my chances of conceiving.
Choosing to have surgery is a huge deal for anyone, and the time leading up to it was extremely nerve-wracking. Confiding my concerns to my doctors and friends really helped me to overcome my worries.
Recovering from the procedure was nowhere near as difficult or painful as I had anticipated. Within a few months I was feeling the full benefits of the procedure. Having the surgery completely and radically changed my life for the better – reducing my pain down to virtually nothing and allowing me to naturally conceive a much longed for baby boy.
I am still astounded that I have painless periods after so many years of suffering, something I had honestly never believed was possible. Six years later I am still feeling really well”.
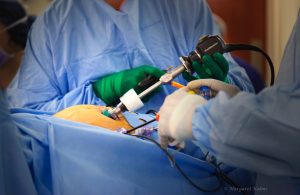
Is there evidence that surgery improves pain associated with endometriosis?
For the Cochrane Gynaecology and Fertility Review ‘Laparoscopic surgery for endometriosis‘ (October, 2020), the review authors including Dr James Duffy (@jamesmnduffy) collected all the best available research evidence comparing surgery to treat endometriosis with only diagnostic surgery (no treatment). They evaluated 14 trialsClinical trials are research studies involving people who use healthcare services. They often compare a new or different treatment with the best treatment currently available. This is to test whether the new or different treatment is safe, effective and any better than what is currently used. No matter how promising a new treatment may appear during tests in a laboratory, it must go through clinical trials before its benefits and risks can really be known. including 1563 women. The reviewers concluded that it was uncertain whether laparoscopic surgery reduces overall pain associated with endometriosis.
Despite it being offered widely, it is unclear whether surgery improves endometriosis associated pain. In this Cochrane ReviewCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research., there was also insufficient research evidence on adverse events to draw any conclusion on the safetyRefers to serious adverse effects, such as those that threaten life, require or prolong hospitalization, result in permanent disability, or cause birth defects. of the procedure.
We know that this may come as a surprise to many readers, however many international guidelines which draw upon wider sources of research continue to recommend surgery as an effective treatment for pain associated with endometriosis.
When considering the decision of whether to go ahead with surgery, it is important to discuss with your endometriosis specialist the risk that your pain may not get better with surgery and discuss a contingency plan for this undesired situation.
Claire’s reflections
“I know I am somewhat ‘lucky’ and that some people with endometriosis do not have such all encompassing success stories from having surgery as myself. Many women in my local endometriosis support group have had temporary relief from surgery at best and don’t feel like the benefits have outweighed the huge physical and financial burden that having surgery can sometimes entail. I am keeping my fingers crossed that the pain relief I have experienced will be long lived”.
Questions to ask your gynaecologist about keyhole surgery
- What are the risks of surgery based on my endometriosis?
- Should I consider hormonal treatment before or after surgery?
- If my pain does not improve what are the next steps?
Future research on keyhole surgery
Professor Andrew Horne (@horne_research), and the team based at Edinburgh University, have set up a research trial, called ESPriT2, to assess whether women with pain symptoms due for a laparoscopic surgery would be willing to be randomly allocated to either treatment of endometriosis or no treatment for people with pain associated with superficial/peritoneal endometriosis. This is a landmark trial and may help internationally guide and patients towards knowing whether surgery for this form of endometriosis is safe and beneficial. More information about how people may be able to get involved will be available soon on the Edinburgh University website.
Support for people with endometriosis
There is a vibrant online community of women with endometriosis, commonly known as #endosisters, who share knowledge and offer support, along with charities such as Endometriosis UK and grassroots organisations such as Fair Treatment for the Women of Wales.
Further information about endometriosis
- Cochrane Gynaecology and Fertility: Endometriosis Awareness Month
- Endometriosis UK
- The British Society for Gynaecological Endoscopy (BGSE) maintains a list of accredited endometriosis centres.
References and further reading (pdf)
Claire Barker and Martin Hirsch have nothing to disclose.
*Images used with permission and cannot be reused without permission from the artist.

Join in the conversation on Twitter with @EndoLadyUK, @MartinHirsch100 @CochraneUK and @CochraneCGF or leave a comment on the blog.
Please note, we cannot give medical advice and do not publish comments that link to individual pages requesting donations or to commercial sites, or appear to endorse commercial products. We welcome diverse views and encourage discussion but we ask that comments are respectful and reserve the right to not publish any we consider offensive. Cochrane UK does not fact check – or endorse – readers’ comments, including any treatments mentioned.


