In a blog for people expecting or caring for a new baby, Sarah Chapman looks at some common concerns and tackles fads, fashions and hard evidence!
Page last updated 08 August 2022; page last checked 9 May 2023.
Take-home points
When I was first left alone with my new baby (our first), husband back at work and Mum gone home, I had a letter from my Nan. She wrote: “You were in my thoughts so much on Monday – your first day alone with such a responsibility! – and hoping you were doing better than I did when in the same situation. One thing I can promise you is that it’s never so frightening again.”
She was quite wrong, I discovered. But for Nan, memories of how worried she was as a new mum to each of her babies, back in the 1930s, remained strong in her old age. She also recalled how pressured she felt to abide by the rules of the baby care guru of the day, Sir Frederic Truby King, though ill at ease with his regimented approach.
Many parents will relate to this. The needs of babies don’t change, after all, and each generation gets its Truby King (my mum followed Dr Spock while I ignored Gina Ford) to add to the other anxieties of whether we’re doing it right. There’s also a bewildering array of products that promise to fix just about anything that ails the new mum and her baby, from sore nipples to colic.
I’ve taken a look at the evidence from Cochrane ReviewsCochrane Reviews are systematic reviews. In systematic reviews we search for and summarize studies that answer a specific research question (e.g. is paracetamol effective and safe for treating back pain?). The studies are identified, assessed, and summarized by using a systematic and predefined approach. They inform recommendations for healthcare and research. that might help you as you care for your baby and yourself in those early days and weeks after birth. Cochrane Reviews look for all the research studies that meet a predefined set of criteria that could help answer a question about, for example, treatments for breast engorgement. This gives us a more reliable ‘answer’ than single studies can, about the possible benefits and harms of treatments, or they may show that there’s no hard evidence behind the claim that this thing or that is good for your baby or for you.

Breastfeeding
According to Unicef, in the UK we have some of the lowest breastfeeding rates in the world, with eight out of ten women stopping breastfeeding before they want to. Whilst not all women are able to breastfeed, or not for as long as they would like, and others choose not to, the benefits of breastfeeding for both women and babies are well-established. The World Health Organization recommends that, where possible, breastfeeding should start within an hour of birth, that all babies should be exclusively breastfed from birth to the age of six months and that breastfeeding should continue as part of the infant’s diet for two years or longer.
We gathered lots of resources that summarise Cochrane Reviews on breastfeeding on this page for our 2019 series Maternity Matters, and we have a number of blogs on different aspects of breastfeeding, and a blog for parents of preterm babies about getting them feeding by mouth, so do take a look. Meanwhile, I want to highlight a few things.
Getting going: skin-to-skin contact with your baby
If you’re awaiting the arrival of your baby you may be interested to know that there is evidence of the benefits of skin-to-skin contact for establishing breastfeeding, among other things. Skin-to-skin contact involves putting the dried, naked baby on the mother’s bare chest (often with a blanket on top of the baby), ideally straight after birth and until the end of the first breastfeed. When this happens, evidence shows that women who have skin-to-skin contact with healthy babies are probably more likely to be breastfeeding at one to four months and to exclusively breastfeed, both at the time of going home from hospital and between six weeks and six months.

Baby-led or scheduled breastfeeding?
My Nan, and the many other women who were assured that feeding their babies by the clock was the right way to do it, might have been interested to know that there is no reliable evidence (from randomized trials) investigating how scheduled (or a mixture of scheduled and baby-led) breastfeeding compares with baby-led breastfeeding in healthy newborns.
The fashion for scheduled feeding in Nan’s day was driven by bottle feeding but recommended for breastfeeding too. Now, baby-led breastfeeding is encouraged in guidelines issued by the WHO and the United Nations Children’s Fund (WHO 2009), through the Baby Friendly Hospital Initiative. Do we still need to be talking about this and looking for evidence? The authors of this review are clear that we do. They note that the impact of scheduled feeding practices from the last century is still influential, that women often get conflicting advice and that many guidelines are not based on high-quality evidence. The review authors call for research exploring “all aspects of the frequency and duration of breastfeeding”.

Preventing mastitis (inflammation of the breast)
Mastitis, which is inflammation of the breast, with or without infection, is a common problem among lactating (milk-producing) women. It is a cause of significant misery and a common reason for women to give up breastfeeding. A Cochrane Review on interventions for preventing mastitis after childbirth (published September 2020) has found that there is a lack of robust evidence and continued uncertainty on the potential harms and benefits of preventive measures.
Does dummy use affect breastfeeding?
Some people have strong feelings about the use of dummies, or pacifiers (and do you remember that weird ‘90s trend for pacifier necklaces?). One concern is that babies might confuse dummies with nipples and stop breastfeeding earlier as a result. A Cochrane Review Effect of restricted pacifier use in breastfeeding term infants for increasing duration of breastfeeding (published August 2016) explored the effects of restricting dummy use in healthy babies whose mothers intended to exclusively breastfeed. It shows that unrestricted use of a dummy probably makes no difference to how many babies are breastfeeding (exclusively or partially) at three and four months old. There was little or no information on potential harms, or on any impact of pacifier use on breastfeeding problems, mothers’ satisfaction, infant crying or other potential problems like misalignment of teeth.

More drinks for you, more milk for baby?
I remember being so thirsty when I was breastfeeding my babies, and so delighted when anyone brought me a cup of tea – but then I’m always pretty happy when that happens. Does increasing the amount you drink result in more breast milk? A Cochrane Review Extra fluids for breastfeeding mothers for increasing milk production (published June 2014) found only one small trial – so uncertainty remains (but maybe don’t share that if you’re enjoying being brought drinks when you feed your little one!).

Breast engorgement
Prepare to be surprised and possibly disappointed. As we enter the third decade of the 21st century, we’re still asking whether treatments that range from applying cabbage leaves to breasts (popular in England several hundred years ago) to the ancient Chinese technique of Gua-Sha (scraping therapy – ouch!) help reduce breast engorgement and we still haven’t got any good evidence to go on, as this Cochrane Review on Treatments for breast engorgement during lactation (published September 2020) shows. The endurance of cabbages in the British medical repertoire is a triumph for cabbage marketing but there are no prizes for its evidence base. Probably best kept for the cooking pot (along with the scraping perhaps!), which brings to mind my Nan’s instructions to “stay with your cabbage”. I’m not sure what purpose that serves either, but maybe to prevent its ruination by overcooking.

Other common problems
Colic
If you’ve had a colicky baby, you’ll remember the misery. If you have one now, you have my sympathies! Infantile colic is a common problem, only rarely indicative of a serious underlying problem, which is typically defined as full‐force crying for at least three hours per day, on at least three days per week, for at least three weeks. Even at that threshold, it can feel like much more.
I’m afraid the bottom line here is that several Cochrane Reviews on different ways of trying to prevent or relieve colic have highlighted a lack of reliable evidence and continued uncertainty about whether they work and are safe. This is the case for probiotics, changes to babies’ diets, manipulative therapies (chiropractic, osteopathy and cranial manipulation) and pain-relieving agents, such as drugs, sugars and herbal preparations, and also parent training programmes to help parents manage infantile colic.

Gastro-oesophageal reflux: those ‘sicky’ babies
Gastro-oesophageal reflux, where babies bring their stomach contents back up, is very common in babies and gets better by itself. However, for formula-fed babies with this problem, thickening the feed is a common practice to try to reduce it. There is evidence from eight studies in this Cochrane Review Feed thickener for infants up to six months of age with gastro‐oesophageal reflux (published December 2017) that feed thickeners probably result in two fewer episodes or regurgitation or vomiting per day, based on comparison with babies who did not have thickened feeds and who had on average three episodes of regurgitation or vomiting per day. Thickeners may also make it more likely that a baby will be free of reflux symptoms. None of the studies reported any serious harms from feed thickeners.

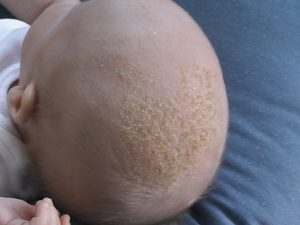
Cradle cap
You’ve probably heard of ‘cradle cap’ but perhaps not its formal name, infantile seborrhoeic dermatitis (ISD). ISD is a chronicA health condition marked by long duration, by frequent recurrence over a long time, and often by slowly progressing seriousness. For example, rheumatoid arthritis., inflammatory skin condition which causes a red, greasy, scaly rash on infant skin – and when it’s on the scalp it’s commonly known as cradle cap. It gets better by itself after a few weeks or months, but parents may worry about it.
A Cochrane Review Interventions for infantile seborrhoeic dermatitis (including cradle cap) (published March 2019) looked for evidence from clinical trialsClinical trials are research studies involving people who use healthcare services. They often compare a new or different treatment with the best treatment currently available. This is to test whether the new or different treatment is safe, effective and any better than what is currently used. No matter how promising a new treatment may appear during tests in a laboratory, it must go through clinical trials before its benefits and risks can really be known. on any treatmentSomething done with the aim of improving health or relieving suffering. For example, medicines, surgery, psychological and physical therapies, diet and exercise changes. for ISD. It is disappointing that there was only very low-certaintyThe certainty (or quality) of evidence is the extent to which we can be confident that what the research tells us about a particular treatment effect is likely to be accurate. Concerns about factors such as bias can reduce the certainty of the evidence. Evidence may be of high certainty; moderate certainty; low certainty or very-low certainty. Cochrane has adopted the GRADE approach (Grading of Recommendations Assessment, Development and Evaluation) for assessing certainty (or quality) of evidence. Find out more here: https://training.cochrane.org/grade-approach evidence from a few small trials and nothing at all on common treatments such as mineral oils or antifungals. So we are uncertain about whether treatments work, if they are safe, and how they compare to each other.
Enjoy your baby…
Nan ended that letter, after reporting on seeing my cousin’s baby (“She had on her head a navy beret… Where have all the bonnets gone?”), with a comment on mine: “I get the feeling that Emily has brought a lot of happiness with her, but just you wait until I see her!” As you navigate all the challenges, I hope you get to enjoy your baby too.
Back to you
We already have some really useful blogs here on some common problems for new mums.
- Jennifer Hanratty has written here about her own experiences of perineal pain after birth and at the evidence on what can help.
- If you’re breastfeeding and are troubled by sore nipples, read this blog before rushing to spend your money on the products claiming to have the answers.
- Finally, whether you’re pregnant, newly delivered or anyone for whom constipation is a problem, do read this very popular blog by pelvic physiotherapist and comedian Elaine Miller.
Join in the conversation with @SarahChapman30 @CochraneUK or leave a comment on the blog. Please note, we will not publish comments that link to commercial sites or appear to endorse commercial products.
Sarah Chapman has nothing to disclose.




Very interesting and insightful.
Fantastic review Sarah!!
What a fabulous summary. Thank you Sarah.